Table of Contents >> Show >> Hide
- What “rare neurodegenerative disorder” actually means
- The diagnostic odyssey: when “it’s probably stress” stops being funny
- Building the care team (and accepting that your calendar is now a co-worker)
- Symptom management in real life: small wins that add up
- When love meets logistics: the relationship shift couples don’t get warned about
- Paperwork: the villain nobody cast, but everyone has to deal with
- Research and clinical trials: hope, but with a seatbelt
- Caring for the caregiver (because burnout is not a badge of honor)
- FAQ: quick answers couples actually ask
- Conclusion: the journey is hardand still yours
- Experiences: what couples say the journey actually feels like (and what helps)
- 1) The early phase feels like living inside a question mark
- 2) The diagnosis brings both relief and griefat the same time
- 3) The “invisible work” becomes the real workload
- 4) Couples grieve roles, not just abilities
- 5) The best days aren’t always the easiestthey’re the most supported
- 6) Humor becomes a coping strategywhen it’s aimed at the problem, not the person
The first time the word “neurodegenerative” enters a couple’s life, it rarely arrives with a drumroll. It usually shows up
disguised as something annoyingly ordinary: a clumsy stumble, a stubborn case of dizziness, a “why can’t I focus my eyes on the
stairs?” moment, or a hand that won’t cooperate when it’s time to button a shirt.
Then come the appointments. The tests. The “Let’s try this medication” detours. The medical acronyms that multiply like rabbits.
And somewhere in the middle of it all, two people who once argued about what to watch on Friday night find themselves negotiating
bigger questions: How do we plan? How do we stay us? How do we keep hope without falling for hype?
This article walks through the journey many couples face when a rare neurodegenerative disorder enters the relationshipwhat the
diagnosis often involves, how care tends to evolve, and how partners can protect quality of life (and their sanity) along the way.
It’s written with respect, real-world practicality, and just enough humor to keep the paperwork from winning.
What “rare neurodegenerative disorder” actually means
“Neurodegenerative” means the condition involves progressive damage to the nervous systemoften specific brain regions or nerve
pathways that control movement, balance, speech, thinking, swallowing, or the body’s automatic functions like blood pressure and
bladder control. “Rare” means fewer people have it, which sounds like a fun exclusivity club until you realize it can also mean:
fewer specialists nearby, less public awareness, and a longer road to the right diagnosis.
Rare neurodegenerative disorders come in different “families.” Some look like Parkinson’s disease at first but aren’t Parkinson’s.
Examples include multiple system atrophy (MSA) and progressive supranuclear palsy (PSP), sometimes grouped under “Parkinson-plus”
or “atypical parkinsonism.” Others may be inherited ataxias (balance/coordination disorders), certain frontotemporal dementia
syndromes, leukodystrophies, or other uncommon neurological conditions. The details vary, but the couple’s challenge often rhymes:
new symptoms appear, roles shift, and both partners need support.
One tricky truth: “rare” doesn’t mean “mysterious forever.” It means the right clinicians and the right pattern recognition
matter a lotand getting there may take persistence.
The diagnostic odyssey: when “it’s probably stress” stops being funny
Early signs couples tend to notice first
Couples often become accidental detectives. One partner experiences changes; the other partner notices patterns. In disorders like
MSA or PSP, early signs can include balance problems, falls, stiffness, changes in walking, and slowed movements. Some conditions
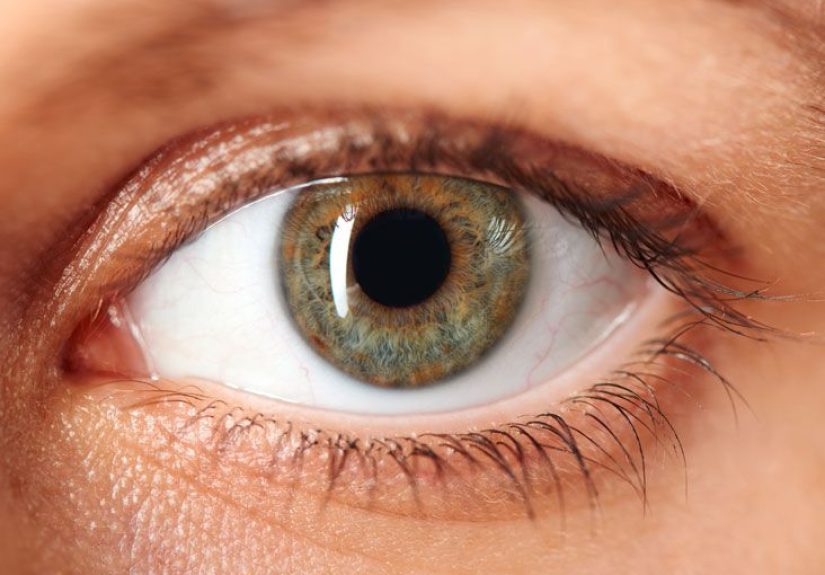
also affect eye movements (for instance, PSP can involve difficulty moving the eyes, especially vertically), which can show up as
trouble reading, navigating stairs, or maintaining steady vision.
In MSA specifically, the “autonomic nervous system” can be involvedmeaning problems with blood pressure regulation (like dizziness
or faintness when standing), bladder dysfunction, and other automatic body functions may show up alongside movement symptoms.
Couples may describe it as “a grab bag of weirdness” because symptoms don’t always follow a neat order.
How clinicians usually narrow it down
Diagnosing rare neurodegenerative disorders can be hard because symptoms overlap with more common conditions. Specialists often rely
on a combination of detailed history, neurological exams, and targeted testing. For suspected MSA, evaluations may include autonomic
testing (to assess blood pressure/heart rate control), bladder assessment, sleep history, and brain imaging such as MRI to support
the diagnosis or rule out other causes. For suspected PSP, clinicians look for characteristic patterns involving balance, eye
movements, and progression.
Here’s the part couples should know: a clear diagnosis sometimes takes time, not because anyone is “missing it,” but because certain
features may become more obvious as the condition evolves. That’s emotionally brutal, but it’s also why tracking symptoms over time
can be genuinely useful.
Genetics: when family history becomes a tool, not a blame game
Not all rare neurodegenerative disorders are inherited. Still, when symptoms suggest a genetic conditionor when there’s a strong
family historygenetic counseling can help couples understand what testing can (and can’t) tell them. A genetics professional
typically reviews personal and family medical history, explains inheritance patterns, discusses testing options, and helps people
make informed decisions without pressure. For couples, this can reduce the “doom-scrolling” impulse and replace it with an actual
plan.
Building the care team (and accepting that your calendar is now a co-worker)
Rare neurodegenerative disorders often require a team approach. A typical care squad may include:
- Neurology: ideally a movement disorders specialist or a neurologist experienced with the specific condition.
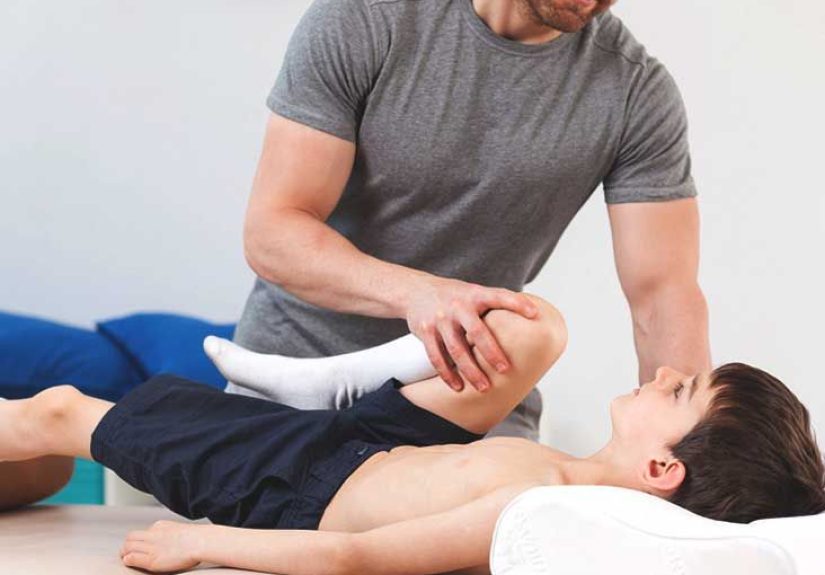
- Physical and occupational therapy: to maintain mobility, reduce fall risk, and adapt daily tasks.
- Speech-language pathology: for speech clarity, swallowing safety, and communication tools.
- Urology/Autonomic specialists: when bladder issues or blood pressure regulation are major problems.
- Social work/care coordination: for resources, equipment, benefits, and caregiver support.
- Palliative care: focused on symptom relief, quality of life, and goal-settingoften helpful long before end-of-life.
Palliative care deserves a special shout-out because it’s frequently misunderstood. It’s not the same as hospice. Palliative care
can be provided alongside other treatments at any stage of a serious illness, focusing on comfort and quality of life. Hospice is a
type of palliative care typically reserved for the final months of life when the focus shifts away from curative treatment. Couples
who involve palliative care earlier often report feeling more supported and less alone in decision-making.
Symptom management in real life: small wins that add up
Movement, balance, and fall prevention
Falls are more than “oops.” They can change independence overnight. Couples often find that the most effective approach is layered:
targeted exercises from PT, mobility aids introduced sooner (not as “giving up,” but as “staying in the game”), and home adjustments
that reduce risk.
Practical examples couples swear by:
- Rearranging furniture so walking paths are wide and uncluttered.
- Adding grab bars in bathrooms and sturdy rails on stairs.
- Switching to shoes with better grip and avoiding slippery socks (cute socks are not worth the ER visit).
- Using a walker or cane before falls become frequentconfidence matters.
Autonomic symptoms: dizziness, blood pressure swings, bladder issues
In conditions like MSA, autonomic dysfunction can be a major driver of day-to-day stress. Standing dizziness, faintness, urinary
urgency, or retention can disrupt routines and sleepthen everything else feels harder.
Care teams may recommend specific strategies depending on the symptom pattern (and the person’s overall health). The key for couples
is to describe real-world impact clearly: “This happens every time we stand after meals,” or “We’re up five times a night.” That
kind of detail helps clinicians target support.
Swallowing, choking risk, and communication
Swallowing difficulty can show up in several neurodegenerative disorders and should be taken seriously because it can increase the
risk of aspiration (food or liquid entering the airway). Speech-language pathologists can evaluate swallowing and recommend safer
textures, posture techniques, and pacing strategies.
Communication changes are also commonsometimes speech becomes softer, slower, or harder to understand. Couples often benefit from a
“communication toolbox,” which might include:
- Simple pacing rules: one person talks at a time, slower than feels necessary.
- Low-tech supports: note cards, whiteboards, or a shared notes app.
- High-tech options: text-to-speech or other assistive communication tools when recommended.
The goal isn’t perfect speech. The goal is staying connected without turning every conversation into a frustrating guessing game.
When love meets logistics: the relationship shift couples don’t get warned about
Rare neurodegenerative disease doesn’t just change a body; it changes the “operating system” of a household. The partner who drove
everywhere might stop driving. The one who handled finances might struggle with planning or fatigue. The other partner gradually
becomes the organizer, the advocate, the schedule keeper, and sometimes the interpreter in medical visits.
Couples who navigate this best often do two things consistently:
- They name the shift out loud. “This is harder,” “I miss how it used to be,” “I’m scared,” “I’m tired.” Naming it reduces shame.
- They protect “partner time.” Not every moment can be medical. Even 20 minutes of non-illness conversation matters.
A gentle but important note: the caregiver partner’s identity matters too. You’re allowed to be a person, not just a role.
Paperwork: the villain nobody cast, but everyone has to deal with
Couples often say the emotional load is heavybut the administrative load is sneakily exhausting. Legal and planning steps can feel
intimidating, yet they can also bring relief by turning unknowns into decisions.
Many families start with advance care planning: discussing preferences for medical care in the future and putting key decisions in
writing through advance directives. This typically includes naming a healthcare proxy (someone to make decisions if the person can’t)
and documenting treatment preferences. Doing this early helps ensure the person living with the condition keeps a voice in their
future care.
Couples also often explore:
- Financial planning: benefits, disability resources, insurance coverage, and budgeting for home adaptations.
- Equipment planning: mobility aids, bathroom supports, home safety tools.
- Work planning: job adjustments, leave options, and caregiver work flexibility where possible.
If this section makes you want to lie down on the floor dramatically, that’s normal. Bring help into the processsocial workers,
patient advocacy organizations, and legal professionals can be worth their weight in perfectly organized binders.
Research and clinical trials: hope, but with a seatbelt
Rare disorders often come with active research communities, but the “trial landscape” can be confusing. Clinical trials may study
symptom treatments, disease progression markers, or potential disease-modifying therapies. Participation can be empowering for some
couplesand not the right fit for others, depending on travel, eligibility, and personal priorities.
A practical mindset: treat clinical trial searches like shopping for hiking boots. Don’t buy the first pair you see. Compare
requirements, talk with your clinicians, and consider how participation affects daily life.
Patient advocacy organizations and rare disease networks can also help families understand opportunities, find specialists, and
connect with support servicesespecially when the diagnosis is uncommon enough that local resources feel thin.
Caring for the caregiver (because burnout is not a badge of honor)
Caregiving can be meaningful and deeply lovingand still be exhausting. Major health organizations emphasize caregiver self-care
because stress, sleep disruption, and isolation can accumulate quickly.
Couples who last the long haul often build a “support scaffold,” such as:
- Respite breaks: even short, scheduled breaks protect mental health.
- Support groups: online or local groups reduce isolation and provide practical tips.
- Health maintenance: the caregiver keeps their own medical appointments and sleep habits on the radar.
- Delegation: friends and family often want to help; specific tasks (“pick up groceries Tuesday”) work better than vague offers.
The caregiver’s well-being isn’t a “nice-to-have.” It’s part of the care plan.
FAQ: quick answers couples actually ask
Is palliative care the same as hospice?
No. Palliative care focuses on symptom relief and quality of life at any stage of serious illness and can occur alongside other
treatments. Hospice is typically for the final months of life when the focus is comfort rather than curative treatment.
How do we find experts if the condition is rare?
Ask your neurologist about specialty clinics or centers with experience in the condition. Rare disease organizations and NIH-backed
resources can also guide families to reliable information and support networks.
What should we track between visits?
Track symptoms that affect safety and daily function: falls, dizziness when standing, swallowing issues, sleep disruptions, bladder
problems, medication side effects, and any notable changes in speech, walking, or thinking. Real examples (“three near-falls after
showering”) are more useful than general statements (“worse lately”).
How do we talk to family without scaring everyone?
Many couples do best with a clear, honest update and a specific ask. “This condition is progressive; here’s what it affects; here’s
what helps us right now.” People handle uncertainty better when they can be helpful.
Conclusion: the journey is hardand still yours
A rare neurodegenerative disorder can feel like a thief: it steals predictability, time, and sometimes abilities you assumed would
always be there. But couples are not powerless. Good care is often built from many small, practical choicessafer routines, stronger
support, earlier planning, better symptom management, and honest conversations.
If you’re in this journey, you deserve a care team that takes you seriously, resources that make life easier, and a community that
reminds you you’re not doing this in isolation. And yesyou also deserve a moment of laughter when your shared calendar looks like
it’s training for the Olympics.
Experiences: what couples say the journey actually feels like (and what helps)
The medical facts explain the “what,” but couples live in the “how.” Below are common experiences many partners describeshared here
as real-world patterns (not one specific story), with practical lessons that often make the road more manageable.
1) The early phase feels like living inside a question mark
Before diagnosis, couples often cycle through theories: inner ear issues, stress, “maybe it’s just aging,” “maybe it’s a pinched
nerve.” There’s a strange whiplash between serious worry and ordinary life. One day you’re researching neurologists; the next day
you’re arguing about which detergent to buy like nothing is happening.
What helps in this stage is building structure without panicking:
- Keep a simple symptom log: dates, triggers, what improved it, what didn’t.
- Bring a partner to appointments if possible; two sets of ears catch more details.
- Ask for clear next steps: “What are we ruling out?” and “What should make us call sooner?”
2) The diagnosis brings both relief and griefat the same time
Couples frequently report an unexpected mix: relief that it has a name, anger that it took so long, and grief for what the future
might hold. Some partners feel guilty for feeling relieved (“Is that terrible?”), but it’s not. A name can unlock better care,
support organizations, and a path forward.
What helps here is allowing two truths to coexist: you can be devastated and still ready to plan.
3) The “invisible work” becomes the real workload
People picture caregiving as lifting or helping someone walk. Couples say the heavier part is often invisible:
coordinating appointments, tracking medications, calling insurance, filling out forms, following up on referrals, managing home
safety, and translating symptoms into useful medical language. It’s like running a small business, except the product is “daily life.”
What helps:
- Create a shared “care hub” (a notebook or digital folder) for meds, test results, and appointment notes.
- Use checklists for recurring tasks (refills, therapy scheduling, equipment maintenance).
- Automate what you can: pharmacy reminders, calendar alerts, and a running question list for the next visit.
4) Couples grieve roles, not just abilities
A lot of loss isn’t dramatic. It’s subtle: the person who always drove now asks for rides; the partner who handled taxes now needs
help with bills; one person can’t be spontaneous anymore because fatigue and symptoms “vote no” in advance.
Many couples say it helps to hold a monthly “state of the union” conversation:
- What got harder this month?
- What’s one thing we can change to make next month easier?
- What do we missand how can we still get a version of it?
These conversations don’t fix everything, but they reduce resentment and prevent one partner from silently carrying the whole load.
5) The best days aren’t always the easiestthey’re the most supported
Couples often learn that “a good day” is less about symptoms magically disappearing and more about supports being in place:
the right mobility aid, a safer bathroom setup, a therapy plan that matches real life, and a backup person who can step in.
One of the most repeated lessons: accept help earlier than you think you “deserve” it. Support isn’t a reward for suffering enough.
It’s a tool to keep life livable.
6) Humor becomes a coping strategywhen it’s aimed at the problem, not the person
Couples often use humor to survive the endless logistics: calling the shared calendar “our third roommate,” naming the walker,
or joking that they’ve earned an honorary degree in Medical Phone Tag. The key is keeping humor kindlaughing at the absurdity of
systems and situations, not at symptoms.
And sometimes the funniest win is genuinely small: an appointment where someone finally explains things clearly, or the day a new
tool makes showering less scary. In a progressive condition, small wins aren’t small. They’re everything.