Table of Contents >> Show >> Hide
- What Is the Appendix, Exactly?
- What Does the Appendix Do?
- Appendicitis: When the Appendix Becomes a Problem
- How Doctors Diagnose Appendix Problems
- Treatment Options: Surgery, Antibiotics, or Both?
- Appendectomy Recovery: What Most People Can Expect
- Appendix FAQs (Because Your Brain Will Ask Anyway)
- Real-World Experiences: What Appendicitis and Recovery Often Feel Like
- Conclusion
- SEO Tags
The appendix is one of the most famous “mystery guests” in the human body: small, quiet, and usually minding its own businessuntil it absolutely is not.
If you’ve ever heard someone say, “My appendix tried to kill me,” they’re only being a little dramatic. Appendicitis is a real medical emergency, and it can escalate fast.
But the organ itself? That’s where things get interesting.
For decades, the appendix was treated like the body’s spare change: a leftover piece from evolution with no job and no résumé.
Modern research has complicated that story. While you can live a perfectly normal life without an appendix, scientists have found strong clues that it may help the immune system and support healthy gut bacteriaespecially earlier in life.
So is the appendix useless? Not exactly. Is it essential? Also not exactly. Welcome to anatomy’s favorite gray area.
What Is the Appendix, Exactly?
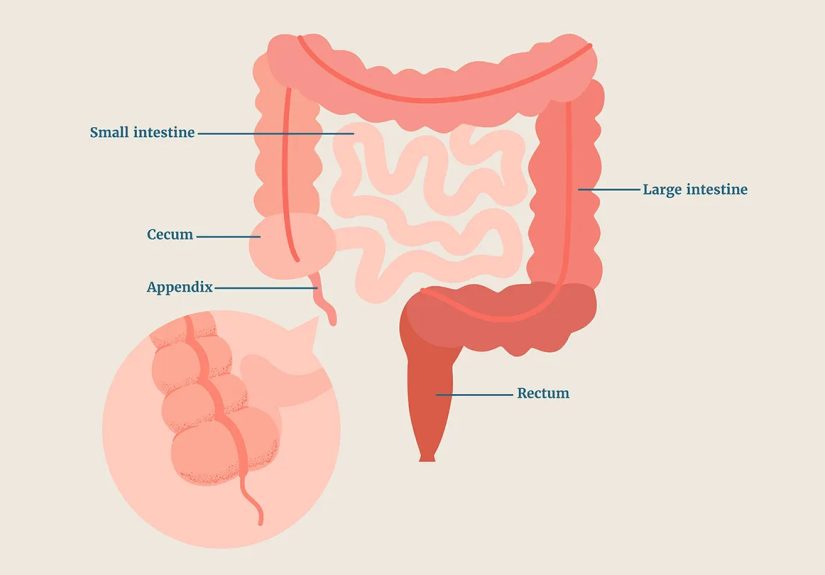
The appendix (more formally, the vermiform appendix) is a narrow, tube-like pouch connected to the first part of the large intestine (the cecum).
It typically sits in the lower-right part of your abdomen. In many people, it’s “finger-sized,” but its length and position can vary.
That variability is one reason appendix problems don’t always read like a textbook.
Where is the appendix located?
Most often, the appendix is found in the right lower quadrant (RLQ) of the abdomen.
However, it can point in different directions (for example, behind the colon), which can change how pain feels and where it shows up.
Translation: your appendix doesn’t always follow the map you saw in health class.
What does the appendix look like?
Think of it as a small, worm-like tube with a hollow inside (called a lumen).
When that lumen gets blocked, pressure builds, blood flow can be affected, bacteria can multiply, and inflammation ramps upthe perfect storm known as appendicitis.
What Does the Appendix Do?
Here’s the honest answer: we still don’t have a single, universally agreed-upon “main purpose” for the appendix.
Many reputable medical sources describe it as having no essential functionmeaning removing it doesn’t usually cause noticeable health problems.
But “not essential” is not the same as “does nothing.”
Possible job #1: Immune system support (especially in childhood)
The appendix contains a good amount of immune tissue (part of what’s called gut-associated lymphoid tissue, or GALT).
This kind of tissue helps the body recognize and respond to microbes in the digestive tract.
Some researchers think the appendix may play a role in immune “training,” especially earlier in life when the immune system is still learning what’s normal and what’s trouble.
Possible job #2: A “safe house” for helpful gut bacteria
One of the most talked-about modern theories is that the appendix may serve as a protected home base for beneficial gut bacteria.
In this idea, the appendix can help “re-seed” the gut after severe diarrhea or intestinal infections that flush out normal microbes.
Researchers have described bacterial biofilms in and around the appendix that may support this reservoir function.
Possible job #3: A role in gut balance and inflammation
Scientists are also exploring links between the appendix, the microbiome, and inflammatory conditions in the gut.
The appendix appears to interact with intestinal bacteria in ways that may influence immune responses and inflammation.
This is active research, and it’s not a simple “appendix good” or “appendix bad” storymore like “appendix complicated.”
Bottom line: the appendix probably isn’t a random factory defect. But it also isn’t a VIP organ like your heart or liver.
It’s more like a helpful coworker who doesn’t always show up on the org chart.
Appendicitis: When the Appendix Becomes a Problem
Appendicitis is inflammation of the appendix, usually caused by blockage inside the appendix.
When the opening gets cloggedby hardened stool (sometimes called an appendicolith), swelling of tissue, or other causesbacteria can overgrow and the appendix can become infected.
Without prompt treatment, it can rupture, spreading infection through the abdomen. That’s why appendicitis is treated as an emergency.
Common symptoms of appendicitis
Appendicitis often begins as vague belly pain that changes over time. A classic pattern is:
pain starting near the belly button and then moving to the lower-right abdomen.
But not everyone gets the “classic pattern,” and children, older adults, and pregnant people may present differently.
- Abdominal pain that may start near the belly button and move lower-right
- Pain that worsens with movement, coughing, deep breathing, or bumps (yes, even a pothole can be rude)
- Loss of appetite
- Nausea and/or vomiting
- Fever
- Bloating or swelling of the abdomen
- Bowel changes such as constipation, diarrhea, or trouble passing gas
When to seek emergency care
If you suspect appendicitisespecially with worsening right-sided abdominal pain, fever, and nauseaseek medical care right away.
Appendicitis can worsen within hours, and a rupture can happen within a couple of days after symptoms begin in some cases.
This is not a “sleep it off” situation.
How Doctors Diagnose Appendix Problems
Diagnosing appendicitis is part detective work, part science, and part “your appendix didn’t read the script.”
Doctors typically combine symptoms, a physical exam, lab tests, and imaging.
They also work to rule out other causes of abdominal painlike stomach viruses, urinary problems, or (in some people) gynecologic conditions.
Physical exam and lab tests
A clinician may check for tenderness in the lower-right abdomen, pain with certain movements, and signs of irritation inside the abdomen.
Blood tests may show signs of infection or inflammation. Urine tests can help rule out urinary tract issues that can mimic appendicitis.
Imaging: Ultrasound, CT, and MRI
Imaging often helps confirm the diagnosis and check for complications.
The choice depends on age, pregnancy status, and the clinical situation:
- Ultrasound is commonly used first in children and pregnant people because it avoids radiation.
- CT scans are frequently used in adults because they are highly accurate for appendicitis.
- MRI may be used when radiation should be avoided (for example, pregnancy or younger patients) and when expertise is available.
Treatment Options: Surgery, Antibiotics, or Both?
The “traditional” treatment for appendicitis is an appendectomysurgery to remove the appendix.
For many people, especially with more severe or complicated appendicitis, surgery is still the standard.
But in some cases of uncomplicated appendicitis, antibiotics may be an optionoften with trade-offs.
Appendectomy: The classic fix
An appendectomy removes the inflamed appendix, eliminating the immediate source of infection.
It may be done in two main ways:
- Laparoscopic appendectomy: several small incisions, a camera, and surgical tools. Often less pain and faster recovery.
- Open appendectomy: a larger incision in the lower-right abdomen. This may be needed in some complicated cases (like widespread infection).
Many hospitals give antibiotics before surgery, and sometimes after, depending on severity and whether complications like rupture or abscess are present.
Most appendectomies happen quickly after diagnosis because the risk of rupture increases over time.
Antibiotics-first: A real option for some people
Research in recent years has shown that some people with uncomplicated appendicitis can improve with antibiotics aloneat least initially.
The upside: avoiding surgery right away.
The downside: a higher chance the appendicitis comes back or that surgery is needed later, plus more follow-up and uncertainty.
In real life, the decision is often about priorities: Do you want the “one-and-done” approach (surgery), or do you strongly prefer trying to avoid an operation (antibiotics), understanding the chance of recurrence?
This is where shared decision-making with a clinician matters.
What if the appendix has ruptured or an abscess forms?
Complicated appendicitis can involve rupture, infection spread (peritonitis), or a localized pocket of infection (abscess).
In these cases, treatment may include urgent surgery and/or drainage of an abscess plus antibiotics.
The key point: complicated appendicitis is not a “watch and wait” problem.
Appendectomy Recovery: What Most People Can Expect
Recovery depends on the surgical method and how advanced the infection was.
Generally, laparoscopic surgery has a shorter recovery time than open surgery.
Many people start walking soon after surgery (often the same day or the next), because gentle movement helps reduce complications.
Typical recovery timeline (varies by person)
- After laparoscopic appendectomy: many people limit strenuous activity for several days and gradually resume normal routines.
- After open surgery: activity limits may last longer because the incision is larger and healing takes more time.
Your medical team will give personalized instructionsespecially about wound care, pain control, and when you can return to work, school, sports, or heavy lifting.
If you had a rupture or abscess, recovery may involve a longer hospital stay and a longer course of antibiotics.
Signs to call a doctor after surgery
- Fever, worsening pain, or swelling
- Redness, drainage, or increasing tenderness around the incision
- Persistent vomiting or inability to keep fluids down
- Symptoms that feel like “something is getting worse,” not better
Appendix FAQs (Because Your Brain Will Ask Anyway)
Can you live without an appendix?
Yes. People live normal lives after appendectomy.
Even if the appendix has immune and microbiome-related roles, it isn’t typically considered essential for day-to-day health.
Is appendicitis preventable?
There’s no guaranteed way to prevent appendicitis.
It often starts with a blockage inside the appendix, and why that blockage happens isn’t always clear.
The most important “prevention” strategy is recognizing symptoms and seeking care quickly.
Is appendicitis always obvious?
Not always. Some people have atypical symptoms, and pain can show up in slightly different places depending on appendix position.
That’s why clinicians often combine exam findings, labs, and imagingrather than relying on one symptom alone.
What’s the difference between the appendix and an “appendix” in a book?
In a book, an appendix is extra information at the end.
In your body, the appendix is extra information attached to your colon.
Both can cause confusion, but only one might send you to the emergency room. (Choose your reading material wisely.)
Real-World Experiences: What Appendicitis and Recovery Often Feel Like
Medical descriptions of appendicitis are helpful, but they can sound oddly tidylike the body politely sends a calendar invite that says,
“Hello, please note: inflammation has been scheduled for 2:00 p.m.”
Real life is messier. People’s experiences vary, and that variability is exactly why appendicitis can be tricky.
Many people describe the beginning as “something feels off” rather than “I have textbook appendicitis.”
The pain might start as a general stomachache near the belly button, the kind you’d blame on a questionable snack or stress.
Then, over hours, it changes: it sharpens, it localizes, and it becomes harder to ignore.
Some people notice that movement makes it worsestanding up, walking, coughing, even laughing.
Others say they suddenly lose their appetite and feel nauseated, even if they didn’t think the pain was that serious at first.
A common storyline is the “false reassurance loop”: someone waits because they hope it’s just a stomach bug, then they wait longer because they’re worried about “overreacting,”
and then they end up in urgent care thinking, “Okay, now I’m reacting.”
That’s not a character flawabdominal pain is one of the hardest symptoms to interpret on your own.
And because appendicitis can progress quickly, clinicians often say it’s better to get checked and be told “not appendicitis” than to wait until it becomes complicated.
In the emergency department, people often remember two things vividly: (1) how many times they were asked to rate pain from 1 to 10, and (2) how fast the process can move once appendicitis is suspected.
Imaging and lab tests can feel like an obstacle course, but they’re there for a reason: other conditions can mimic appendicitis,
and the treatment plan changes a lot depending on whether the appendix looks uncomplicated or potentially ruptured.
After an appendectomyespecially laparoscopicmany people are surprised by what recovery is actually like.
They expect the pain to be “only” where the appendix was, but discomfort can be more general at first.
Some people describe feeling sore when they stand up straight or when they try to sit up from bed, because the abdomen is involved in so many basic movements.
Fatigue is also common: anesthesia, infection, disrupted sleep, and stress can make even a short walk feel like a marathon.
On the brighter side, people often say they feel a clear turning point within days: appetite begins to return, pain becomes more manageable, and walking becomes easier.
The most consistent “experience-based” advice from patients tends to be simple: follow your discharge instructions, take pain control seriously (but safely),
walk a little as recommended, and don’t rush back into heavy lifting or intense workouts just because you feel impatient.
Recovery isn’t a contest. It’s more like rebuilding a routine one normal activity at a timestanding comfortably, walking without wincing, eating without nausea, sleeping through the night.
And if something feels like it’s getting worse instead of betterfever, increasing pain, or concerning incision changespeople who had smooth recoveries will tell you the same thing:
call your clinician. Peace of mind is a legitimate part of healing.
Conclusion
The appendix may be small, but it has earned a big reputationpartly because appendicitis can be serious, and partly because scientists still debate what the appendix actually does.
The best current understanding is this: the appendix isn’t essential for survival, but it likely plays a supporting role in the immune system and gut microbiome, especially earlier in life.
And when it becomes inflamed, fast evaluation matters because complications can develop quickly.
If there’s one practical takeaway, it’s this: unexplained, worsening abdominal painespecially pain that migrates or settles in the lower right abdomendeserves medical attention.
Your appendix may be a mystery, but appendicitis shouldn’t be.






