Table of Contents >> Show >> Hide
- What EB does to the body (the “effects” part)
- Types of epidermolysis bullosa (and why “where it blisters” matters)
- Common symptoms of EB (the checklist your skin never asked for)
- Why EB symptoms can look different from one person to another
- Triggers: what tends to set EB off
- How EB is diagnosed (briefly, because guessing is unfair)
- When symptoms need urgent medical attention
- Living with EB: of real-world experiences (what families often describe)
- Conclusion
Medical note: This article is for education, not diagnosis. If you think you (or your child) might have epidermolysis bullosa (EB), a clinicianoften a dermatologist and/or genetic specialistshould evaluate it.
Epidermolysis bullosa (EB) is a group of rare conditions where skin (and sometimes mucous membranes) are so fragile that everyday frictionlike a sock seam, a diaper change, or even a well-meaning back rubcan cause blisters, raw areas, and wounds. EB is sometimes nicknamed “butterfly skin” because the skin can tear as easily as a butterfly wing. Cute nickname, brutal reality.
EB isn’t one single disease. It’s an umbrella term for multiple types and subtypes, usually caused by inherited changes in genes that make “skin glue” proteins. Those proteins normally hold skin layers together. In EB, that glue is weak, missing, or flawedso layers separate under stress and form blisters.
What EB does to the body (the “effects” part)
EB effects range from mild and localized to severe and life-altering. The big picture is recurrent blistering + slow-healing wounds, but the ripple effects can involve multiple body systems.
Skin effects
- Blisters and erosions after minor rubbing, pressure, heat, or scratching
- Chronic wounds that may bleed, ooze, and heal slowly
- Pain and itching that can be constant (and exhausting)
- Scarring and skin changes in some types (thickened areas, pigment changes, miliatiny white bumps)
- Nail changes (thickened nails, deformed nails, or nail loss)
Mucous membrane and internal effects
Depending on the type, EB can affect tissue beyond the skin:
- Mouth and throat blisters, leading to feeding pain or swallowing problems
- Esophageal involvement (in some severe forms), potentially causing narrowing/strictures and significant dysphagia
- Eye irritation or injury from fragile surface tissues
- Dental problems (like enamel defects and cavities) in certain types
Whole-body complications (especially in moderate-to-severe EB)
- Infections (open skin is an easy entry point; repeated infections can become serious)
- Anemia from chronic inflammation and/or blood loss from wounds
- Poor growth in children due to increased calorie needs, feeding difficulties, and chronic illness
- Contractures (tightening of skin and tissues) and reduced mobility in scarring types
- Fusion of fingers/toes (sometimes called “mitten” deformity) in severe scarring subtypes
- Higher risk of aggressive squamous cell carcinoma in certain severe dystrophic forms, often in adulthood
Real-life example: A child with localized EB simplex might mostly get painful foot blisters after sports practice or long walks. Meanwhile, someone with a severe dystrophic form may need daily wound care, nutrition support, and monitoring for strictures, infections, anemia, and skin cancer risk over time.
Types of epidermolysis bullosa (and why “where it blisters” matters)
Clinicians categorize EB partly by the skin layer where the blister forms. That location correlates with typical symptoms, severity, scarring, and complications.
| Major Type | Where Blistering Happens | Typical Clues | Scarring? |
|---|---|---|---|
| EB simplex (EBS) | Within the epidermis (upper skin) | Often hands/feet; friction-triggered; can be mild to severe | Usually minimal |
| Junctional EB (JEB) | At the basement membrane zone (“junction”) | May be widespread; can involve mucosa; severity varies | Variable |
| Dystrophic EB (DEB) | Below the basement membrane (deeper separation) | Scarring common; nail loss; strictures/contractures in severe forms | Often yes |
| Kindler EB | Mixed levels (can “move around”) | Skin fragility + photosensitivity; pigment changes may appear | Variable |
1) EB simplex (EBS)
EBS is often described as the most common major EB type. Many cases are milder and centered on the palms and solesplaces where friction is basically a lifestyle. Blisters may flare with heat, sweating, and activity. In some subtypes, blistering can be more widespread or severe.
Typical scenario: A teen gets recurring foot blisters after walking the mall or playing basketball. The shoes aren’t “bad”the skin’s structural support just can’t handle the normal shear forces.
2) Junctional EB (JEB)
JEB involves separation at the skin’s “junction” where layers connect. Severity ranges widely: some people have localized disease; others have extensive blistering and mucosal involvement. Because the separation can be at a critical anchoring zone, wounds may be more significant than in mild EBS.
3) Dystrophic EB (DEB)
DEB tends to blister deeper in the skin, which is one reason scarring is more common. Subtypes can be inherited in dominant or recessive patterns. Severe recessive forms can lead to chronic wounds, nail loss, scarring that limits movement, and complications like esophageal strictures, anemia, and increased skin cancer risk later in life.
Plain-English version: If EBS is like the top layer of a cake sliding, DEB is like the cake separating lower downmessier, more likely to leave a lasting mark.
4) Kindler EB
Kindler EB is rarer and can involve blistering at multiple skin levels. People may also have photosensitivity (skin reacting strongly to sun exposure) and evolving pigment changes. Symptoms can shift over time.
A quick note on “acquired EB” (EBA)
Most EB is inherited and often starts in infancy or childhood. There is also a distinct condition called epidermolysis bullosa acquisita (EBA), which is autoimmune and usually begins in adulthood. It can look EB-like on the surface (blistering with minor trauma), but the cause and treatment approach differso clinicians separate it from the inherited EB types.
Common symptoms of EB (the checklist your skin never asked for)
Symptoms depend on type and severity, but these are common across the EB spectrum:
Skin symptoms
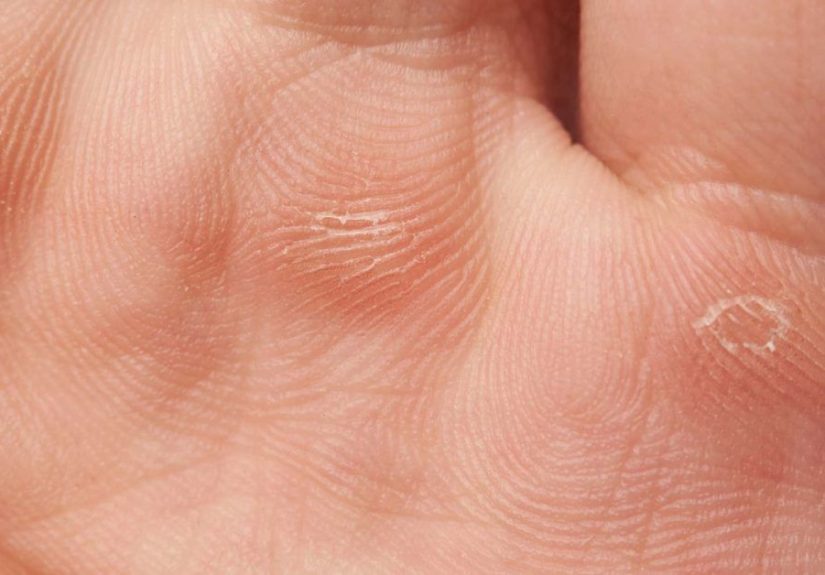
- Blisters (clear, blood-filled, or tense) that may burst quickly
- Open sores that can be slow to heal
- Fragile skin that tears with friction or minor bumps
- Itching, which can be intense (and yes, scratching can worsen blistering)
- Pain from wounds, dressing changes, and inflammation
- Milia (tiny white bumps) on healed or healing skin
- Thickened skin/calluses, especially on hands/feet in some EBS types
- Nail problems (thickened, misshapen, or missing nails)
- Hair/scalp involvement in some forms (including scarring alopecia)
Mouth, throat, and digestive symptoms
- Blisters in the mouth causing feeding pain
- Hoarseness or airway irritation in certain cases
- Difficulty swallowing (dysphagia) or food “sticking” if the esophagus is affected
- Constipation can happen indirectly (pain, reduced mobility, diet limits, dehydration)
Growth, blood, and energy symptoms
- Slow weight gain or growth delays in children with more severe disease
- Anemia symptoms (fatigue, pallor, shortness of breath with activity)
- Low energy from chronic pain, inflammation, and sleep disruption
Why EB symptoms can look different from one person to another
Two people can both have “EB” and still have wildly different daily realities. Differences often come down to:
- Which gene/protein is involved (the “skin glue” isn’t one single ingredient)
- Where the blister forms (superficial vs deeper separation)
- Inheritance pattern (dominant vs recessive) and the specific subtype
- Environmental triggers (heat, humidity, activity level, friction points)
- Wound care access and infection prevention support
Triggers: what tends to set EB off
EB doesn’t need a dramatic cause. It’s more like: “Congratulations, you wore socks.” Common triggers include:
- Friction from clothing seams, tags, or shoes
- Heat and sweating
- Scratching (especially when itching is intense)
- Pressure points (knees, elbows, hands, feet)
- Medical tape or adhesives (often a no-go unless specifically designed for fragile skin)
- Minor bumps or normal toddler activities like crawling
How EB is diagnosed (briefly, because guessing is unfair)
Because EB overlaps with other blistering conditions, diagnosis typically involves a combination of:
- Clinical exam and history (when it started, where it blisters, family patterns)
- Skin biopsy for specialized testing (to identify the blister level and affected proteins)
- Genetic testing to confirm type/subtype and guide counseling
When symptoms need urgent medical attention
Seek urgent care if EB symptoms include:
- Signs of infection (spreading redness, warmth, pus, fever, increasing pain)
- Difficulty breathing, choking, or severe swallowing problems
- Dehydration signs (especially in infants/children)
- Rapidly worsening wounds or uncontrolled bleeding
Living with EB: of real-world experiences (what families often describe)
EB isn’t just “skin blisters.” It’s logistics, emotions, and planning that would make a wedding coordinator sweat. Families often describe mornings as a carefully choreographed routine: choosing clothes that are soft, tag-free, and seam-minimized; checking yesterday’s friction points; and planning the day around dressing changes. Many caregivers say they become experts in suppliesnonstick dressings, soft wraps, moisturizers, and the art of securing bandages without adhesives that can tear fragile skin.
One of the most repeated themes is pain management. Dressing changes can be the hardest part of the day. People talk about finding “small wins”: warming a room so bandages come off more gently, timing changes after medication when prescribed, or using distraction (music, videos, breathing techniques) to make the process less overwhelming. It’s not about being tough; it’s about being practical and kind to a body that’s working overtime.
School and social life can be a mixed bag. Some kids with milder EB report that the most annoying part is the constant foot blister cyclewalk, blister, heal, repeatlike an unwanted subscription service. Others with more severe EB describe needing accommodations: extra time between classes, avoiding contact sports, permission to carry wound-care items, and a plan for handling infections or fatigue. Parents often mention that educators who understand EB can be game-changingsimple adjustments like cushioned seating, careful handling, and flexibility around absences can help a child stay included.
Adults with EB often talk about the “invisible labor” of chronic wound care: the time, the costs, the mental load of monitoring for infection, and the effort required to do everyday things without triggering new blisters. Many describe learning their personal trigger map: which shoe brands work, which fabrics behave, which temperatures are “safe,” and which activities require trade-offs. There can be grief in those trade-offsbut also pride in adaptability.
Emotionally, EB can test patience and identity. People mention frustration when others treat it like a simple rash, or when strangers stare at bandages. Support groups and EB organizations are often described as lifelines, not just for medical tips but for the relief of being understood without explanation. Many families say the most helpful friends aren’t the ones with perfect words; they’re the ones who show upoffering a meal, childcare, a ride to appointments, or simply respecting boundaries about touch.
And yes, humor shows up here toooften as a survival tool. Not the kind that makes light of suffering, but the kind that says: “We’re still here, and we still get to laugh.” When someone with EB jokes about their wardrobe being “approved by the Soft Fabric Council,” it’s not denial. It’s resilience with personality.
Conclusion
Epidermolysis bullosa is a complex group of conditions defined by fragile skin that blisters from everyday friction. Understanding the type (EBS, JEB, DEB, Kindler EBand the separate autoimmune EBA) helps explain the likely symptoms and long-term effects, from localized foot blisters to severe chronic wounds and systemic complications. If EB is suspected, professional evaluation mattersbecause in EB, details aren’t trivia; they shape care, comfort, and quality of life.