Table of Contents >> Show >> Hide
- What Is a Gingivectomy?
- Why Someone Might Need a Gingivectomy
- What Happens Before the Procedure?
- What to Expect During a Gingivectomy
- Does a Gingivectomy Hurt?
- Recovery: Timeline, Foods, and What Normal Healing Looks Like
- When to Call the Dentist
- How Much Does a Gingivectomy Cost?
- Are the Results Permanent?
- Possible Risks and Complications
- Questions Worth Asking Before You Book It
- Bottom Line
- Patient Experience and Recovery Stories: What People Commonly Notice
If the word gingivectomy sounds like something out of a dental sci-fi movie, take a breath. It is much less dramatic than it sounds. A gingivectomy is a procedure that removes excess or diseased gum tissue. Dentists and periodontists use it to treat certain gum problems, reduce deep gum pockets, and sometimes improve the look of a “gummy smile.” In many cases, the procedure is quick, done with local anesthesia, and followed by a fairly manageable recovery.
Still, no one gets excited when a dental professional says the word “surgery.” You probably want the practical version: Will it hurt? How long will healing take? What can you eat? How much does it cost? And do your gums just decide to make a comeback tour afterward? This guide breaks down what to expect before, during, and after a gingivectomy in plain English, with real-world context and a few reality checks along the way.
What Is a Gingivectomy?
A gingivectomy is the surgical removal of part of the gingiva, which is the gum tissue around your teeth. The procedure may be done with a scalpel, laser, or another soft-tissue technique, depending on the dentist’s training, your gum condition, and the treatment goal.
It is commonly used for two main reasons. First, it can help treat gum disease when excess or damaged tissue creates deep pockets that trap plaque and bacteria. Second, it can be used for cosmetic reshaping when too much gum tissue covers the visible part of the teeth and makes them appear short or boxy.
In simple terms, a gingivectomy removes tissue. That is different from a gingivoplasty, which mainly reshapes gum tissue, and different from crown lengthening, which may involve both gum and bone contouring to expose more tooth structure. These procedures can overlap, but they are not interchangeable.
Why Someone Might Need a Gingivectomy
To Treat Periodontal Problems
When gum disease progresses, the tissue around the teeth can become swollen, overgrown, or detached in a way that creates periodontal pockets. Those pockets are hard to clean with normal brushing and flossing, which lets bacteria hang out like unwanted houseguests. A gingivectomy can reduce those pockets and make home care more effective.
To Remove Overgrown Gum Tissue
Some people develop gum enlargement because of inflammation, orthodontic appliances, genetics, or certain medications. Drug-related gingival overgrowth is especially associated with some anticonvulsants, calcium channel blockers, and immunosuppressants. In mild cases, better hygiene and medication review may help. In more severe cases, surgery may be needed.
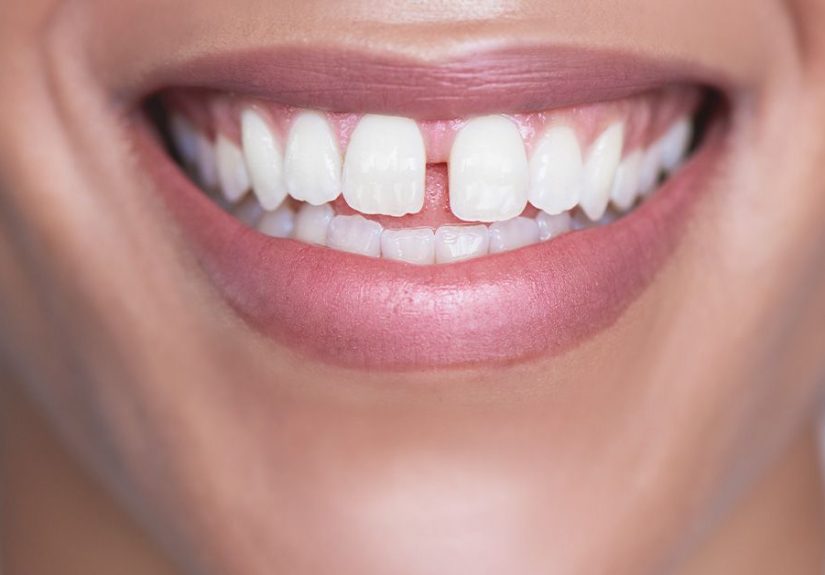
To Improve Smile Aesthetics
If your teeth look unusually short because extra gum tissue covers too much of the enamel, a gingivectomy may be part of cosmetic smile improvement. This is often called gummy smile correction. The goal is not to create a fake “Hollywood smile,” but to make the gum line look more balanced and let more of the natural tooth show.
What Happens Before the Procedure?
Your dentist or periodontist will first examine your gums, teeth, bite, and overall oral health. They may measure gum pockets, check for inflammation, review your medical history, and take X-rays if needed. This step matters because not every gummy smile or gum issue should be treated with a gingivectomy alone.
You will also discuss your medications and health conditions. This is especially important if you smoke, have diabetes, take blood thinners, have a history of heart valve problems, or have had certain cardiac procedures. Some dental procedures that involve manipulation of gum tissue call for preventive antibiotics in a small group of patients with specific high-risk heart conditions. That is not routine for everyone, so your provider will decide whether it applies to you.
If your dentist plans to use local anesthesia only, prep is usually simple. If sedation is part of the plan, you may need someone to drive you home. In many cases, the procedure is done in one visit and you go home the same day.
What to Expect During a Gingivectomy
Most gingivectomies are outpatient procedures and usually take about 30 to 60 minutes, though treatment on multiple teeth can take longer. Here is the typical sequence:
1. Numbing the Area
Your provider will use local anesthesia to numb the gums. If you are nervous, sedation may also be offered. During the procedure, you should feel pressure and movement, but not sharp pain.
2. Removing the Excess Tissue
The dentist or periodontist removes the extra or diseased gum tissue using a scalpel or laser. The amount removed depends on the treatment goal, whether it is infection control, pocket reduction, or cosmetic reshaping.
3. Reshaping the Gum Line
Once the excess tissue is gone, the remaining gums are contoured so the gum line looks and functions more naturally. In some cases, minor bone reshaping may also be needed to create the right proportions or reduce the chance of tissue rebound.
4. Closing and Protecting the Site
If a scalpel is used, stitches may be placed. A protective periodontal dressing may also be applied for several days. With some laser procedures, sutures may be minimal or unnecessary.
Does a Gingivectomy Hurt?
During the procedure itself, local anesthesia usually prevents pain. Afterward, mild discomfort, swelling, minor bleeding, and tooth sensitivity are common. Most people describe the recovery as more annoying than unbearable. Think “my gums are complaining” rather than “I have entered a medieval torture chamber.”
Over-the-counter pain relief may be enough for some patients, while others may receive prescription pain medication or antibiotics depending on the case. Your provider will tell you exactly what to take and what to avoid.
Recovery: Timeline, Foods, and What Normal Healing Looks Like
The First 24 to 72 Hours
This is when swelling, tenderness, and light oozing are most noticeable. Cold compresses on the outside of the jaw can help. You will usually need to avoid hard brushing directly on the surgical site and follow cleaning instructions closely.
About One Week
Initial healing often takes around one week. Many people return to school or office work within a day or two, though heavy physical activity should wait at least 48 hours or longer if your provider advises it. If your job involves strenuous labor, you may need more time off.
Several Weeks
Your gums continue maturing after the first week, even if you already feel better. Some sources note that most patients resume a normal oral care routine within a month, especially once tenderness settles down and follow-up care confirms that healing is going well.
What to Eat After Gingivectomy
Soft foods are your friends. Great options include yogurt, scrambled eggs, mashed potatoes, oatmeal, smoothies, soup that is warm rather than blazing hot, cooked vegetables, pasta, and applesauce. Crunchy chips, crusty bread, spicy foods, sticky candy, very acidic drinks, and extremely hot foods are usually a bad idea early on.
Also, wait until the numbness wears off before eating. Accidentally biting your cheek because your mouth feels like it belongs to someone else is not the kind of post-op memory you want.
Oral Care During Recovery
You will need to keep the area clean without irritating it. That often means gentle brushing, using any prescribed antimicrobial rinse, and continuing normal brushing and flossing on the untreated teeth. Do not poke the site with your fingers or tongue. Your tongue is curious, but it is not a surgeon.
When to Call the Dentist
Some bleeding, soreness, swelling, and sensitivity are expected. But you should call your provider if you have:
- Bleeding that does not stop
- Pus or drainage from the surgical area
- Severe pain that is not improving
- Persistent facial swelling
- Fever or signs of infection
Smoking is a big recovery spoiler. It weakens the body’s ability to fight gum infection and makes healing harder, so avoiding tobacco before and after treatment can make a real difference.
How Much Does a Gingivectomy Cost?
The honest answer is: it depends. Cost varies based on how many teeth are involved, whether the procedure is medical or cosmetic, the technique used, your location, and whether a general dentist or periodontist performs it.
For medically necessary treatment related to periodontal disease, insurance may cover part of the cost. For cosmetic reshaping, coverage is much less likely. Consumer-facing U.S. sources often describe pricing by the tooth. Some quote about $200 to $400 per tooth for out-of-pocket cost, while other gum contouring estimates range from roughly $50 to $350 per tooth for smaller cosmetic reshaping, and some laser cosmetic procedures may be priced higher per tooth. In broader periodontal surgery discussions, total treatment costs can be much higher depending on complexity.
The safest takeaway is this: do not trust a random number on the internet more than a written treatment estimate from your own dental office. Ask whether the fee includes anesthesia, follow-up visits, dressings, imaging, and any needed reshaping or maintenance care.
Are the Results Permanent?
In many cases, yes. Surgically removed gum tissue generally does not grow back in the same way once healing is complete. However, that does not mean your mouth gets permanent immunity from future problems. If the underlying issue is poor plaque control, smoking, uncontrolled inflammation, or medication-related enlargement, gum problems can still return in nearby areas or recur to some degree over time.
That is why follow-up care matters. Many patients are advised to keep up routine maintenance visits, sometimes every three months if they have a history of periodontal disease.
Possible Risks and Complications
A gingivectomy is generally considered low risk, but it is still surgery. Possible side effects and complications include:
- Mild bleeding
- Swelling and bruising
- Temporary tooth sensitivity
- Post-op discomfort
- Infection
- Delayed healing
- Rare nerve-related issues or more serious infection complications
Your provider will also decide whether another procedure would serve you better. For example, if too much gum shows because of tooth eruption patterns or bone position, crown lengthening or another periodontal approach may be more appropriate than simple tissue trimming alone.
Questions Worth Asking Before You Book It
- Is this procedure being done for health, cosmetic reasons, or both?
- Will you use a scalpel, laser, or another method?
- Will I need sutures or a periodontal dressing?
- How much gum tissue will be removed?
- Will bone reshaping also be needed?
- What is the expected recovery time for my specific case?
- What will insurance likely cover?
- What signs of complications should make me call right away?
Bottom Line
A gingivectomy is one of those dental procedures that sounds scarier than it usually is. For the right patient, it can make gums healthier, teeth easier to clean, and smiles more balanced. The procedure is usually done with local anesthesia, healing often starts settling down within about a week, and many people get back to normal routines quickly.
The biggest keys to a smooth experience are a proper diagnosis, realistic expectations, careful aftercare, and good long-term oral hygiene. If your dentist or periodontist has recommended a gingivectomy, it is worth asking exactly why, what result they expect, and how they plan to keep your gums healthy after the procedure. Because the goal is not just prettier gums for five minutes. It is a healthier mouth that sticks around for the long haul.
Patient Experience and Recovery Stories: What People Commonly Notice
Experience 1: “The procedure was easier than the anticipation.” A lot of patients say the worst part happened before the appointment even started: worrying about it. Once the local anesthetic kicks in, the procedure itself often feels more like pressure, water, and strange dental noises than pain. People who expected a dramatic, all-day ordeal are often surprised that the visit is relatively short and that they are heading home the same day.
Experience 2: “The first few meals require creativity.” Recovery tends to feel most real when it is time to eat. Patients often report that day one and day two are full of soft foods, careful chewing, and sudden appreciation for mashed potatoes, yogurt, scrambled eggs, and smoothies. Hot coffee lovers sometimes learn patience the hard way. Crunchy snacks usually move from “tempting” to “absolutely not” for at least several days.
Experience 3: “My gums looked weird before they looked great.” This is a common one. Right after surgery, gums may look swollen, uneven, or a little dramatic. Some people worry that something has gone wrong when the gum line looks puffy at first. In many cases, that early appearance is just part of normal healing. As swelling drops and tissue settles, the shape becomes more refined. Translation: do not judge your final result by your bathroom mirror on day two.
Experience 4: “Tenderness was manageable, but sensitivity surprised me.” Some patients expect pain and prepare for it, yet they are more bothered by tooth sensitivity or tenderness when brushing near the area. Cold drinks, spicy foods, or vigorous brushing can feel annoying for a while. This is one reason dentists emphasize gentle cleaning, prescribed rinses, and gradual return to a regular oral care routine. It is not glamorous, but being gentle is usually smarter than trying to prove you are tough.
Experience 5: “The real success came after healing.” Patients treated for gum disease often say the biggest benefit was not cosmetic at all. Once the bulky or inflamed tissue was removed, brushing and flossing became easier. Food stopped getting trapped so easily. Follow-up cleanings felt more productive. Patients treated for a gummy smile, on the other hand, often describe a boost in confidence once their smile looked more balanced in photos. Different reasons, same theme: the best outcome is when the result feels natural and easier to live with every day.
Experience 6: “Maintenance matters more than I thought.” One overlooked part of the gingivectomy experience is what happens after the initial healing phase. Patients who keep their follow-up visits, improve their brushing and flossing habits, and stop smoking if possible usually feel more satisfied long term. Patients who assume surgery “fixed everything forever” can be disappointed if inflammation returns. A gingivectomy can create a healthier setup, but your daily habits still decide whether that setup stays healthy.