Table of Contents >> Show >> Hide
- What Is an Orzuelo (Stye), Exactly?
- Orzuelos: Common Causes and Risk Factors
- Symptoms: What You’ll Usually Notice (and What You Shouldn’t Ignore)
- Prevention: How to Make Styes Less Likely (Without Becoming a Monk)
- Treatments That Actually Work
- How Long Does a Stye Last?
- When to See a Doctor (and What to Expect)
- Common Myths (Let’s Retire These)
- Conclusion
- Real-World Experiences (What People Commonly Run Into) 500+ Words
“Orzuelo” is the Spanish word for what most Americans call a stye (medical name:
hordeolum)a small, tender bump that shows up on or inside your eyelid like it owns the place.
It usually arrives at the worst possible time (photos, presentations, first dates, you name it) and then dares you
to poke it. Don’t. A stye is one of those problems where patience, heat, and good hygiene beat heroics almost every time.
This guide explains what causes styes, how to prevent them from crashing your week again, and which
treatments actually helpplus when it’s time to hand the situation over to a clinician instead of your bathroom mirror.
What Is an Orzuelo (Stye), Exactly?
A stye is usually an infection and inflammation involving an eyelid oil gland or hair follicle.
Think of it as a tiny “pimple-like” problem in a very dramatic location. Most styes are linked to common skin bacteria
(often Staphylococcus) getting into the wrong spot.
External vs. internal stye
- External stye: forms near the eyelashes, often at a lash follicle or glands close to the lash line.
It’s usually easier to see and can look like a red bump along the lid edge. - Internal stye: forms deeper in the eyelid, often involving meibomian (oil) glands.
It can cause more diffuse lid swelling and tenderness.
Stye vs. chalazion (the bump look-alike)
Styes get confused with chalazia all the time. A simple rule of thumb:
styes tend to hurt (active infection/inflammation), while chalazia tend to be less painful
and feel like a firm lump from a clogged oil gland. A stye can sometimes evolve into a chalazion after the “hot and angry”
phase cools down.
Orzuelos: Common Causes and Risk Factors
The main cause: bacteria + a blocked gland
Your eyelids contain multiple glands that produce oils to keep your tear film stable and your eyes comfortable.
When one of these glands gets clogged or irritated, bacteria can multiply and trigger inflammationhello, stye.
Everyday risk factors that quietly set the stage
- Touching or rubbing your eyes (especially with unwashed hands)
- Blepharitis (chronic eyelid margin inflammation)
- Meibomian gland dysfunction (MGD) or oily gland blockage
- Wearing contact lensesespecially with imperfect cleaning habits
- Eye makeup (old mascara, shared products, sleeping in makeup, or not removing it well)
- Skin conditions like rosacea, seborrheic dermatitis, or eczema
- Recent stye history (recurrence is common)
- Systemic factors that may increase susceptibility in some people, such as diabetes or immune compromise
None of this means you did something “wrong.” It just means your eyelids are a busy intersection of oil, skin, bacteria,
and frictionso small shifts in hygiene or inflammation can tip the balance.
Symptoms: What You’ll Usually Notice (and What You Shouldn’t Ignore)
Typical symptoms
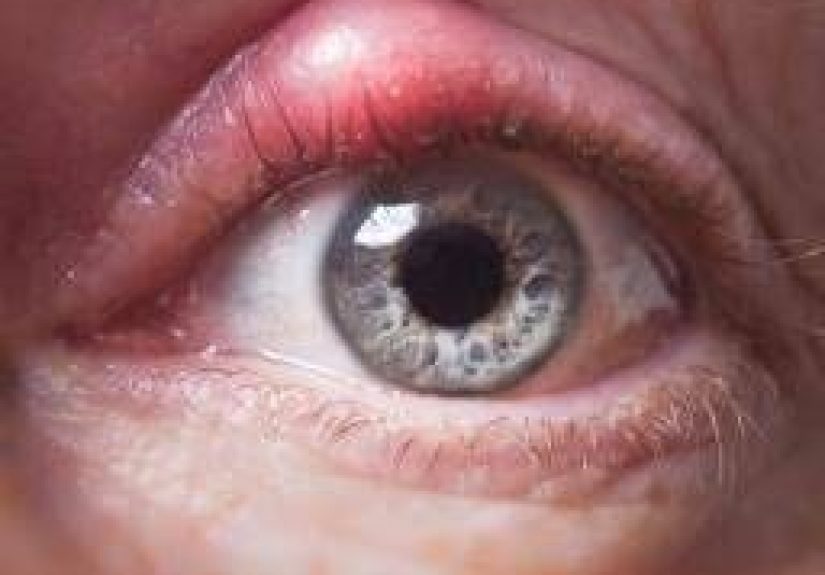
- A tender, red bump on the lid margin or inside the lid
- Swelling of part of the eyelid
- Warmth, irritation, tearing, or a gritty “something’s in my eye” feeling
- Sometimes a small yellowish spot at the center of the bump
Red flags that deserve prompt medical attention
- Vision changes (blurry vision that isn’t just tears)
- Severe swelling that closes the eye or spreads across the face
- Fever or feeling ill
- Increasing pain or rapidly worsening redness
- Pus-like discharge plus expanding redness around the eyelid
- A “stye” that doesn’t improve in 1–2 weeks or keeps coming back
These signs can indicate complications (like preseptal cellulitis) or that the bump is something else that needs evaluation.
Prevention: How to Make Styes Less Likely (Without Becoming a Monk)
Stye prevention is mostly about reducing bacteria transfer and keeping eyelid glands flowing normally.
Think “clean, gentle, consistent”not “scrub your eyelids like a cast-iron skillet.”
Daily habits that help
- Wash hands before touching eyes, contacts, or applying skincare near the eyelids.
- Remove eye makeup fully before bed (yes, even on the “I’m too tired” nights).
- Replace old eye makeup (especially mascara and liquid liners) and avoid sharing products.
- Keep contact lenses clean and follow your eye professional’s disinfection guidance.
- If you have blepharitis or MGD, consider regular warm compresses and lid hygiene
as a maintenance routine.
Quick prevention checklist for frequent repeat offenders
- Warm compress once daily (or as advised) to support oil gland flow
- Gentle eyelid cleansing (commercial lid wipes or clinician-approved routine)
- Manage rosacea/blepharitis with your clinician’s plan
- Stop rubbing eyes (easier said than donetry cold compresses for allergies/itch)
Treatments That Actually Work
1) Warm compresses: the MVP
The most widely recommended at-home treatment is a warm, clean compress applied to the closed eyelid.
Warmth can help soften clogged oils, encourage drainage, and ease discomfort.
- How: Use a clean washcloth soaked in warm (not scalding) water.
- How long: About 10–15 minutes per session.
- How often: 3–5 times a day is commonly recommended.
- Pro tip: Re-warm the cloth as it cools so you’re not applying “lukewarm regret.”
2) Gentle lid hygiene (especially if blepharitis is involved)
If you’re prone to styes or have eyelid inflammation, gentle lid cleansing can reduce debris and bacteria along the lash line.
Many clinicians suggest commercially prepared lid wipes or a simple routine approved by your eye care provider.
3) “Do not do this” list (your future self will thank you)
- Don’t squeeze, pop, or lance the stye. That can worsen inflammation or spread infection.
- Don’t wear eye makeup until it heals (and consider replacing anything used near the infection).
- Don’t wear contact lenses until symptoms resolveglasses are your temporary peace treaty.
- Don’t share towels, and wash pillowcases if you’ve been touching the area a lot.
4) Pain relief and comfort
Over-the-counter pain relievers may help if discomfort is significant (follow label directions and your clinician’s advice,
especially for children or if you have medical conditions). Artificial tears can sometimes soothe irritationbut avoid medicated
eye drops unless recommended by a clinician.
5) When antibiotics or procedures come into play
Many styes improve with warm compresses alone. But clinicians may recommend additional treatment when:
the stye is persistent, there’s concern for spreading infection, or there are signs of complications.
- Topical antibiotic ointment/drops: Sometimes used when there’s associated drainage or eyelid infection.
- Oral antibiotics: Considered if there’s concern for cellulitis or more extensive infection.
- In-office drainage: For stubborn cases, a clinician can drain a lesion safelythis is not a DIY project.
- Steroid injection or chalazion management: More relevant when the bump is a chalazion rather than an active stye.
How Long Does a Stye Last?
Many uncomplicated styes improve within about 1–2 weeks, often sooner with consistent warm compresses.
If you’re not seeing improvement after a week, or if it’s worsening, that’s a good time to get medical guidance.
When to See a Doctor (and What to Expect)
Consider seeing an optometrist, ophthalmologist, or primary care clinician if:
- The stye doesn’t improve after 1–2 weeks of home care
- You get recurrent styes (time to talk prevention and underlying eyelid inflammation)
- The eyelid is very swollen, painful, or red, or you have fever
- You notice vision changes or significant light sensitivity
- The bump looks unusual or keeps returning in the same spot
In a visit, clinicians may check the eyelid margin, look for blepharitis/MGD, and confirm whether it’s a stye or chalazion.
Treatment might range from “keep doing compresses” to topical medication or a minor in-office procedure if needed.
Common Myths (Let’s Retire These)
Myth: “If I pop it, it’ll heal faster.”
Tempting, but risky. Squeezing can push infection deeper and increase swelling. Let it drain naturallyor let a clinician handle it.
Myth: “Styes are super contagious.”
A stye itself usually isn’t “catchy” like the flu, but bacteria can spread through contact.
That’s why handwashing and not sharing towels/makeup matter.
Myth: “Warm compresses are optional.”
Warm compresses are the closest thing styes have to a universally loved treatment. It’s simple, low-risk, and often effective.
Conclusion
Orzuelos (styes) are common, annoying, and usually manageable at home with a surprisingly boringbut effectivecombo:
warm compresses, hands-off patience, and solid eyelid hygiene.
The key is consistency and knowing when to escalate careespecially if symptoms worsen, your vision is affected,
or the problem keeps coming back. If styes are frequent visitors, a clinician can help you target underlying issues
like blepharitis or meibomian gland dysfunction so your eyelids stop throwing surprise parties.
Real-World Experiences (What People Commonly Run Into) 500+ Words
If you’ve ever had a stye, you already know the emotional arc: denial (“It’s just a sleepy eye”), bargaining (“If I blink hard enough,
it’ll go away”), and finally acceptance (“Fine, I’ll do the warm compress thing”). Real-life stye experiences often have a few
predictable plot twistsso let’s talk about what typically happens and what people say they wish they knew earlier.
First, the timing is suspiciously awful. Many people notice early tenderness right when they’re about to be on camera:
a family event, a big meeting, or the one day they decided to try a bold eyeliner wing. Styes can start as a subtle soreness at the lid edge,
then ramp up into a visible bump within a day. That quick shift makes people assume it’s acneand that assumption is where bad decisions begin.
Second, the mirror becomes a negotiator. People often report spending way too long in the bathroom thinking,
“If I just get the angle right…” The problem is that eyelid skin is delicate and swelling is easy to worsen. A common experience is that
repeated checking and touching makes the eyelid puffier, redder, and more irritatedcreating a feedback loop where the stye looks worse,
which leads to more checking, which makes it look worse. The best “hack” here is not a hack at all: wash hands, apply the compress,
and stop auditioning the bump for a reality show.
Third, warm compress consistency is harder than it sounds. People often start strongone compress, maybe twothen get busy.
But many clinicians recommend multiple sessions per day, and that routine is what helps most. A practical pattern many people find workable is
“morning, after work/school, and before bed,” with an extra session if it’s comfortable. Another common lesson: if the cloth cools fast,
the “warm compress” becomes a “mildly comforting damp cloth,” and results feel slower. Re-warming the compress during the session is a small change
that people say makes the routine feel more effective.
Fourth, makeup and contacts become the main villains. Contact lens wearers often describe feeling forced to switch to glasses
for a few days, which can be inconvenientbut it’s usually worth it. Makeup users frequently mention frustration that concealer doesn’t really
help because the bump changes the eyelid shape, and covering it can irritate the area. A common “I wish I knew” moment is realizing that
old mascara is not a loyal friend. Many people decide to replace mascara or eyeliner used around the time of infection to reduce the chance
of reintroducing bacteria.
Fifth, recurrent styes lead to smarter prevention. People who get styes repeatedly often discover they also have eyelid inflammation
(like blepharitis) or meibomian gland issues. Once they adopt a light, regular eyelid hygiene routineespecially during allergy season or periods of
heavy screen timethey often feel more in control. Not everyone needs daily maintenance forever, but many find that small habits (handwashing before
eye touching, removing makeup completely, occasional warm compresses) reduce repeat episodes.
And finally: people often feel relieved after a clinician visit when a stye is stubborn. Knowing whether it’s truly a stye, a chalazion,
or something else can take the mental load off. If you’re stuck in “week two” with no improvement, getting checked isn’t overreactingit’s just choosing
the faster lane back to normal.







