Table of Contents >> Show >> Hide
- First: when “bumps” are totally normal
- A quick self-check: what do your tongue bumps look and feel like?
- Common causes of tongue bumps (and what they usually mean)
- 1) “Lie bumps” (inflamed taste buds / transient lingual papillitis)
- 2) Minor trauma: biting, burning, or friction
- 3) Canker sores (aphthous ulcers) on or under the tongue
- 4) Geographic tongue (map-like patches that come and go)
- 5) Oral thrush (yeast overgrowth)
- 6) Oral lichen planus (inflammatory patches or sores)
- 7) White patches that shouldn’t be ignored: leukoplakia (and “hairy” leukoplakia)
- 8) Nutritional deficiencies and inflammation (glossitis / “smooth” sore tongue)
- 9) When a bump needs a closer look: persistent lumps or sores
- What you can do at home (safe, practical comfort measures)
- Treatments a clinician may recommend (depending on the cause)
- When to see a dentist or doctor (don’t “wait it out” forever)
- Prevention: keeping your tongue from becoming the main character
- Bottom line
- Experiences people commonly report (and what they learned)
Your tongue is basically a tiny, muscular doormat that never gets a break. It tastes, talks, swallows, and bravely
withstands everything from jalapeños to “mystery-hot” coffee. So when you notice bumps on it, your brain does what
it does best: panic-Google at 2 a.m.
Here’s the good news: many tongue bumps are normal (your tongue is supposed to be bumpy), and many “new” bumps are
temporary irritations that clear up on their own. Here’s the more responsible news: some bumps can signal an
infection, inflammation, nutritional issue, or (rarely) something more serious that deserves a professional look.
This guide breaks down the most common causes, what you can do at home, and when to stop playing detective and call
a dentist or doctor.
First: when “bumps” are totally normal
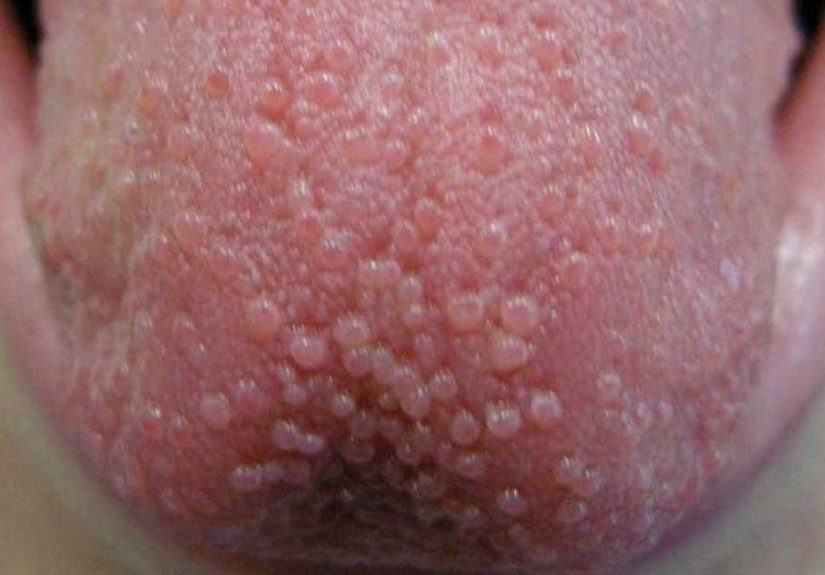
The surface of your tongue is covered in tiny projections called papillae. They’re part of how your tongue grips
food and houses taste buds. In other words, your tongue isn’t meant to be smooth like glassit’s more like a
well-used bath towel (but hopefully cleaner).
Normal papillae can look more noticeable if your tongue is dry, irritated, mildly swollen, or if you’ve been
“taste-testing” spicy, salty, or acidic foods. Sometimes a change in lighting, hydration, or attention makes you
suddenly notice what’s been there all along.
A quick self-check: what do your tongue bumps look and feel like?
You don’t need to become a tongue sommelier, but a few details help you sort harmless from “get it checked”:
- Timing: Did it show up overnight? Has it been there more than 2 weeks?
- Pain: Tender and angry, or painless and just… present?
- Color: Red, white, yellow, or mixed patches?
- Location: Tip of the tongue, sides, underneath, or everywhere?
- Texture: Smooth sore, raised bump, rough patch, or “cottage cheese” coating?
- Triggers: Recent burn, bite, new mouthwash, braces, illness, antibiotics, or inhaler use?
Common causes of tongue bumps (and what they usually mean)
1) “Lie bumps” (inflamed taste buds / transient lingual papillitis)
These are the classic small, painful red or white bumpsoften near the tip of the tonguethat show up suddenly and
make eating feel like a personal attack. Despite the dramatic nickname, they’re typically caused by irritation or
minor inflammation of the papillae (think: biting your tongue, rough foods, stress, hot drinks, or random bad luck).
Typical pattern: hurts, looks alarming, then improves within a few days. If yours behave like a
tiny tantrum that resolves quickly, “lie bumps” are a prime suspect.
2) Minor trauma: biting, burning, or friction
A surprisingly large number of tongue problems are caused by your tongue being in the wrong place at the wrong
time. Accidentally biting the side, burning it on hot food, rubbing against a sharp tooth edge, or irritation from
dental work can create swollen spots, small bumps, or a sore area.
Typical pattern: you remember the moment it happened (or you strongly suspect it), and the area
gradually improves as it heals.
3) Canker sores (aphthous ulcers) on or under the tongue
Canker sores are shallow, painful ulcers that form inside the mouth (unlike cold sores, which typically occur on
or around the lips). They can pop up on the tongue, under it, or on the inner cheeks and gums. Triggers vary:
stress, minor injury, certain foods, hormonal shifts, and sometimes underlying conditions.
Typical pattern: a round/oval sore with a pale or yellowish center and a red halo; painful with
spicy, salty, or acidic foods; usually heals within 1–2 weeks.
4) Geographic tongue (map-like patches that come and go)
Geographic tongue is an inflammatory but harmless condition where patches on the tongue lose some papillae, leaving
smooth red areas with slightly raised borders. The “map” pattern can shift over timelike a weather radar, but for
your mouth.
Typical pattern: irregular red patches that move or change; sometimes burning or sensitivity, often
no symptoms at all; usually doesn’t need treatment beyond comfort measures.
5) Oral thrush (yeast overgrowth)
Thrush can cause creamy white patches that may stick to the tongue or inner cheeks and can leave redness underneath
if wiped. It’s more likely after antibiotics, with inhaled steroids (especially without rinsing afterward), or when
the immune system is weakened.
Typical pattern: white patches/coating, soreness, taste changes, and sometimes a cottony feeling.
In healthy adults, thrush is less commonso it’s worth a professional evaluation.
6) Oral lichen planus (inflammatory patches or sores)
Oral lichen planus can show up as white, lacy patterns or patches, and sometimes painful erosive sores on the
tongue, gums, or inner cheeks. It’s a chronic inflammatory condition that often needs a clinician’s diagnosis and a
tailored management plan.
Typical pattern: persistent white lacy changes, soreness, sensitivity with certain foods, and flare-ups.
7) White patches that shouldn’t be ignored: leukoplakia (and “hairy” leukoplakia)
Some white patches in the mouth can be related to irritation (like tobacco) or other conditions. Oral hairy
leukoplakia, for example, is linked to Epstein–Barr virus and is more common in people with significant immune
suppression. These conditions can look similar to other issues, so diagnosis matters.
Typical pattern: persistent white patch(es), sometimes on the sides of the tongue; may cause little
discomfort. Because a small number of white lesions can be associated with precancerous changes, persistent patches
deserve evaluation.
8) Nutritional deficiencies and inflammation (glossitis / “smooth” sore tongue)
Low levels of certain nutrientsespecially vitamin B12, and sometimes iron or folatecan contribute to tongue
inflammation and changes in the tongue surface. Some people describe burning, tenderness, or a smoother-looking
tongue due to loss of papillae.
Typical pattern: soreness, burning, redness, or smooth areas, often along with other symptoms
(fatigue, anemia-related clues) depending on the deficiency.
9) When a bump needs a closer look: persistent lumps or sores
Most tongue bumps are benign, but a sore or lump that doesn’t healespecially if it persists beyond a couple of
weeksshould be checked. Cancer is not the most common explanation, but early evaluation is the smart move, not the
dramatic one.
Typical pattern that needs attention: a non-healing sore, a firm lump, thickening, unexplained
bleeding, numbness, or symptoms that worsen instead of improve.
What you can do at home (safe, practical comfort measures)
If your symptoms are mild, recent, and you don’t have red flags, supportive care can help your tongue calm down:
Gentle mouth care
- Warm saltwater rinse: soothing and simple (think: “ocean, but less sandy”).
- Soft brushing: keep up oral hygiene, but don’t scrub the sore like it owes you money.
- Avoid irritants: spicy, acidic, crunchy, very hot foods, alcohol-based mouthwashes, and tobacco.
Targeted relief for sores and tender spots
- Protective pastes or gels: over-the-counter oral gels can reduce friction and sting.
- Cold therapy: ice chips or a cold smoothie can reduce swelling and discomfort.
- OTC pain relief: follow label directions; consider avoiding NSAIDs if you have contraindications.
Home tips you may hear about (use thoughtfully)
Some reputable medical references mention options like a baking soda-and-water paste or diluted hydrogen peroxide
rinses for mouth sores. If you try these, keep it mild, never swallow rinses, and stop if it burns or irritates
further. When in doubt, a pharmacist or dentist can steer you toward safer, purpose-made options.
Treatments a clinician may recommend (depending on the cause)
The “right” treatment depends on the diagnosisso the goal is to match the remedy to the culprit:
For lie bumps or minor irritation
- Time and avoiding triggers are often enough.
- Topical comfort measures (cold, gentle rinses) can help you eat without suffering.
For canker sores
- Topical anti-inflammatory treatments may be prescribed for painful or frequent sores.
- If sores are severe, recurrent, or unusual, clinicians may evaluate for contributing factors.
For thrush
- Antifungal medication is often needed.
- Clinicians may check for underlying triggers (recent antibiotics, inhaler technique, diabetes, immune issues).
For geographic tongue
- Often no treatment is required.
- If sensitive, topical options may be suggested to reduce burning with certain foods.
For lichen planus or persistent white patches
- Diagnosis may involve a careful oral exam and sometimes biopsy to rule out other causes.
- Management can include topical treatments and ongoing monitoring.
When to see a dentist or doctor (don’t “wait it out” forever)
Consider getting evaluated if any of the following apply:
- It lasts longer than 2 weeks (or keeps returning in the same spot).
- You have a firm lump, thickening, or a sore that won’t heal.
- Unexplained bleeding, numbness, or severe pain.
- Trouble swallowing, speaking, or persistent hoarseness.
- Fever, swelling, or you can’t eat/drink well.
- White patches that don’t wipe off or recurespecially if you smoke or use tobacco.
- You suspect thrush (especially if you’re an otherwise healthy adult).
If you’re unsure, a dental exam is often a great starting point. Dentists routinely evaluate mouth sores and can
refer you appropriately if anything looks suspicious.
Prevention: keeping your tongue from becoming the main character
- Be kind to your mouth: avoid repeated trauma (sharp foods, aggressive brushing, irritating rinses).
- Rinse after inhaled steroids: if you use a steroid inhaler, rinse and spit afterward.
- Address dental irritants: fix sharp tooth edges, ill-fitting appliances, or irritating orthodontic wires.
- Manage dry mouth: hydration and addressing causes can reduce irritation.
- Reduce cancer risk: avoid tobacco, limit heavy alcohol use, and keep up with routine dental visits.
- HPV prevention: talk with your clinician about HPV vaccination and risk reduction strategies.
Bottom line
Most tongue bumps are either normal papillae doing their job or temporary inflammation from irritation, minor
injuries, or common mouth conditions. The winning strategy is simple: soothe what’s irritated, remove obvious
triggers, and track the timeline. If it’s persistent, worsening, unusually painful, or paired with red-flag
symptoms, get it checked. Your tongue works hardreturn the favor.
Experiences people commonly report (and what they learned)
To make this topic feel less clinical, here are a few “real life” patterns that clinicians hear all the time.
These aren’t medical diagnoses for you (your mouth deserves its own storyline), but they can help you recognize
common scenarios and respond calmly.
Experience #1: “I woke up with a painful bump and now I’m spiraling.”
A lot of people notice a single tender bump near the tip of the tongue first thing in the morningusually after a
weekend of crunchy snacks, spicy food, or accidentally biting the tongue while eating too fast (because adulthood).
The bump feels huge, but when you look closely it’s tiny. The best lesson here is that pain exaggerates size. Many
people report that cold drinks, softer meals for a day or two, and skipping the hot sauce temporarily helped more
than constantly poking it with their teeth. The bump often fades within a few days, and the biggest challenge is
resisting the urge to keep “checking it,” which just irritates it more.
Experience #2: “It’s not one bumpmy tongue feels raw after antibiotics.”
Another common story: someone finishes antibiotics for a sinus or dental issue and then notices a sore mouth,
a coated tongue, or white patches that feel uncomfortable. People often assume it’s just “dry mouth,” so they try
stronger mouthwashonly to make it sting worse. What many learn (sometimes the hard way) is that after antibiotics,
it’s worth considering yeast overgrowth. Getting evaluated can save a lot of discomfort because thrush often needs
targeted antifungal treatment rather than more “scrubbing.” People also frequently mention that gentle rinsing,
staying hydrated, and avoiding alcohol-based rinses made the mouth feel less inflamed while they waited for care.
Experience #3: “The weird red patches come and go, and spicy food feels like lava.”
People with geographic tongue often describe a cycle: the tongue looks normal, then suddenly develops red “map”
areas with pale borders, and certain foods burn more than usual. Many say the shifting pattern is what really
bothers themtoday it’s on the side, next week it’s near the centerso they worry it’s spreading. The most helpful
takeaway is that movement and change can actually be a hallmark of benign conditions. People often report that
dialing back acidic foods (tomatoes, citrus), spicy seasonings, and very salty snacks during flare-ups makes eating
tolerable again. Over time, many stop chasing a “cure” and focus on trigger management and reassurance, especially
once a clinician confirms the diagnosis.
Experience #4: “This spot won’t go away, so I finally got it checked.”
It’s also common to hear: “I thought it would heal, but it’s been weeks.” Sometimes it’s a sore that keeps getting
re-injured (a sharp tooth edge, a habit of chewing one side, or a rough dental surface). Sometimes it’s a persistent
patch that needs evaluation. People often say the hardest part was making the appointment, but the relief came from
having a clear planwhether that meant smoothing a rough tooth, treating inflammation, or (when needed) doing a
biopsy to rule out serious causes. If there’s one “experience-based” tip to remember, it’s this: time matters.
Anything that lingers beyond a couple of weeks deserves professional attentionnot because it’s automatically
dangerous, but because you deserve certainty and appropriate treatment.