Table of Contents >> Show >> Hide
- Quick refresher: what shingles is (and why it can return)
- Can you get shingles more than once?
- Why shingles can recur: the immune-system “guard shift”
- Risk factors that can make shingles more likely to come back
- Shingles recurrence or something else? How it typically feels
- What to do if you think shingles is coming back
- Does the shingles vaccine help prevent recurrence?
- How to reduce your recurrence risk (without going full “wellness influencer”)
- When recurrent shingles is a bigger “check this out” signal
- FAQ: fast answers to common recurrence questions
- Real-life experiences with shingles recurrence (what people commonly report)
- The “I recognized it before the rash” moment
- The “I’m healthywhy me?” surprise
- The “it hit during a stressful season” pattern
- The immunocompromised experience: “I don’t have the luxury of waiting”
- The lingering worry: “Is it going to keep coming back?”
- A grounded mindset that many people find helpful
- Conclusion
If you’ve already had shingles once, you’ve earned the right to say, “No thanks, I’ve met that virus and it was rude.”
Unfortunately, shingles can come back. The good news: recurrence isn’t the norm for most people, and there are
concrete ways to lower the odds of a repeat performance.
In this guide, we’ll break down why shingles can recur, how common it is, who’s most at risk, what to do if symptoms
return, and how vaccination and smart prevention strategies fit into the picturewithout panic, without hype, and with
a healthy respect for your nervous system.
Quick refresher: what shingles is (and why it can return)
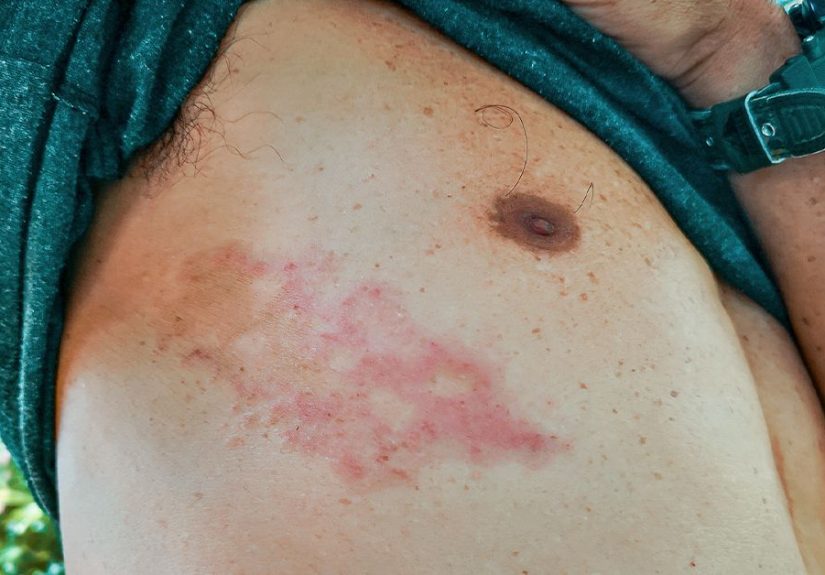
Shingles (also called herpes zoster) happens when the varicella-zoster virusthe same virus
that causes chickenpoxreactivates later in life. After you recover from chickenpox, the virus doesn’t fully “leave.”
It goes dormant in nerve tissue, basically taking a long nap. Years (or decades) later, it can wake up and travel along
a nerve pathway, causing pain, tingling, and a blistering rashoften in a band on one side of the body.
The key word is reactivates. Shingles isn’t something you “catch” from a doorknob. It’s usually your own
dormant virus getting a second wind when your immune defenses are distracted, stressed, or weakened.
Can you get shingles more than once?
Yes. Most people only have shingles one time, but recurrent shingles is absolutely possible. That’s not meant
to scare youit’s meant to prepare you. If you’ve had shingles and start feeling that familiar burning, tingling, or
skin sensitivity again, it’s worth paying attention instead of assuming, “It can’t be shingles because I already did that.”
How common is shingles recurrence?
Estimates vary because studies follow different groups of people for different lengths of time (and because “recurrence”
can be defined in different ways). In general, recurrence appears to be uncommon but not rare. Some sources
summarize that a small percentage of peopleroughly low single digits up to around 10% in certain populationsmay experience
shingles again, especially as the years go on.
What matters most is who you are and what’s going on with your immune system. A healthy adult may never see shingles
again. Someone whose immune system is weakened (by certain medications or medical conditions) has a higher chance of recurrence.
Why shingles can recur: the immune-system “guard shift”
Think of your immune system as the security team that keeps the varicella-zoster virus in its dorm room. Over time, that
security team can get smaller or less coordinatedespecially with agingso the virus gets an opportunity to reactivate.
Shingles recurrence isn’t always a sign of something scary, but it’s often a signal that your immune system isn’t
operating at full “keep-the-virus-asleep” capacity. That could be due to normal aging, temporary stressors, or a medical
issue that reduces immune function.
Risk factors that can make shingles more likely to come back
The biggest theme is simple: weakened immunity. But there are several common ways that can happen.
1) Age (especially 50 and older)
Shingles becomes more common as we age because immune defenses naturally decline over time. That same “immune aging” can
also contribute to the risk of shingles coming back.
2) Immunocompromising conditions or treatments
Recurrence risk rises when the immune system is weakened by disease or therapy. Examples include:
- Cancer treatments (like chemotherapy)
- Organ or stem cell transplant and anti-rejection medications
- HIV or other conditions that affect immune function
- Long-term or high-dose steroids and certain immune-modulating drugs
- Some autoimmune conditions (and the medications used to treat them)
3) Certain chronic health conditions
Some chronic illnesses are associated with higher shingles risk in general. That doesn’t guarantee recurrence, but it’s
part of the overall risk pictureespecially when combined with age or immune-suppressing medications.
4) A tougher first episode (especially long-lasting pain)
People who have more severe shingles symptoms or prolonged nerve pain may represent a group whose immune response didn’t
fully “slam the door” on the virus afterward. That can be one reason recurrence shows up in research studies.
5) Shingles on the face or near the eye
Shingles affecting the eye area (often called shingles ophthalmicus) is a big “don’t wait and see” situation. Even if it
turns out not to be shingles, eye symptoms deserve fast medical attention because complications can affect vision.
Shingles recurrence or something else? How it typically feels
One tricky thing about recurrent shingles is that the early symptoms can look like other issuesespecially before the rash
appears. A recurrence may start with:
- Burning, tingling, itching, or electric “zaps” in one area
- Skin sensitivity (even clothing feels offensive)
- Localized pain on one side of the body or face
- Fatigue or feeling “off” before the rash
Then the rash often shows up in a cluster of blisters that follows a nerve path. That “one-sided, band-like” pattern is a classic clue.
Common look-alikes
- Herpes simplex (cold sores or genital herpes) can recur and cause blisters toobut often in different patterns/locations.
- Contact dermatitis (an allergic reaction) can itch and blister, but doesn’t usually come with nerve pain the same way.
- Skin infections or insect bites can mimic early rash changes.
If you’ve had shingles before, you may recognize the “signature” feeling. Still, it’s smart to confirm with a clinicianespecially if it’s on
your face, near your eye, or spreading quickly.
What to do if you think shingles is coming back
Recurrence isn’t something to tough out in silence. Early treatment can make a real difference in how miserable the episode becomes.
Act fast: antivirals work best early
Prescription antiviral medications (like acyclovir, valacyclovir, or famciclovir) are commonly used for shingles. They’re most effective when
started as soon as possible, ideally within the first few daysoften cited as within about 72 hours of rash onset.
If you suspect shingles and symptoms are ramping up, call your healthcare provider promptly.
Ask about pain control (because nerves have opinions)
Shingles pain can be intense, and the goal is to keep you functioning while your body clears the outbreak. Depending on the situation, options
may include:
- OTC pain relievers (when appropriate for you)
- Prescription pain strategies if pain is severe
- Topical approaches for itching or discomfort
- Discussion of nerve-pain medications if symptoms linger
Know the major complications to watch for
The most well-known complication is postherpetic neuralgia (PHN), where nerve pain continues after the rash heals. Risk increases
with age and severity. Another high-stakes complication: shingles involving the eye, which can affect vision.
Seek urgent care if you have shingles symptoms with any of the following:
- Rash or pain near the eye or on the tip of the nose
- New vision changes
- Severe headache, confusion, or widespread rash
- Weak immune system and rapidly worsening symptoms
Does the shingles vaccine help prevent recurrence?
For many people, the most powerful prevention tool is vaccination. In the U.S., the primary shingles vaccine is
Shingrix (recombinant zoster vaccine).
Who should consider Shingrix?
- Adults 50+: commonly recommended even if you’ve had shingles before.
- Adults 19+ who are immunocompromised: recommended for many people who are or will be immunodeficient or immunosuppressed due to disease or therapy.
Timing: how long should you wait after shingles?
In general, there isn’t a strict “must wait exactly X months” rule after having shingles. A common practical approach is:
wait until the shingles rash has resolved and you’re no longer in the middle of an acute episode, then discuss
vaccination timing with your clinicianespecially if you’re immunocompromised or planning immune-suppressing therapy.
How well does Shingrix work?
Shingrix performed very well in clinical studies, with high efficacy in preventing shingles across age groups. Like any medical tool,
it’s not a magical force field, but it substantially lowers the odds of shinglesand by preventing shingles, it also reduces the chance
of shingles complications such as PHN.
Important detail: Shingrix is a two-dose series. If you only do dose one and ghost dose two, you’re leaving protection on the table.
Side effects: normal, annoying, usually brief
Many people report arm soreness, fatigue, muscle aches, or low-grade fever after vaccination. These effects are typically short-lived.
It’s like your immune system doing push-ups: uncomfortable, but purposeful.
How to reduce your recurrence risk (without going full “wellness influencer”)
Let’s keep this grounded. You can’t control everything, but you can stack the odds in your favor:
1) Get vaccinated if you’re eligible
Vaccination is the most direct strategy to reduce the risk of shingles and potential recurrence. If you’ve already had shingles,
ask specifically about Shingrix and when it makes sense for you.
2) Treat outbreaks early
If shingles returns, prompt treatment can reduce severity and may lower the risk of lingering pain. Don’t wait for the rash to “prove itself”
if the symptoms are classic and escalating.
3) Review immune-suppressing medications with your care team
Don’t stop medications on your ownbut do make sure every prescriber knows your shingles history. For people who are immunocompromised,
vaccine timing and prevention planning may be especially important.
4) Support immune health the boring-but-effective way
You don’t need a shelf full of expensive supplements. Basics matter:
- Consistent sleep
- Balanced nutrition
- Regular movement you can sustain
- Stress management (not because stress “causes shingles,” but because chronic stress can affect immune function)
When recurrent shingles is a bigger “check this out” signal
If shingles recurs multiple times, appears at a young age without obvious explanation, is unusually severe, or is widespread,
it’s worth a deeper conversation with a healthcare professional. Sometimes, recurrence can be a clue that the immune system needs evaluation.
FAQ: fast answers to common recurrence questions
Can shingles come back in the same place?
It can, but many people experience it in a different location the next time because it can reactivate along different nerve pathways.
Either way, similar nerve-type pain and a blistering rash pattern should be checked.
Is recurrent shingles more contagious?
The contagious rules are basically the same: shingles can spread varicella-zoster virus through direct contact with fluid from the blisters.
Someone who hasn’t had chickenpox (or isn’t immune) could develop chickenpoxnot shinglesafter exposure. Once lesions crust over, the risk drops.
Does having shingles once protect you from getting it again?
Not completely. Your body does develop an immune response, which likely helps explain why many people don’t get shingles againbut it isn’t a lifetime guarantee.
That’s one reason vaccination is still recommended for many people who already had shingles.
Can stress trigger shingles recurrence?
Stress doesn’t work like a light switch (“I had a rough week, therefore shingles”). But immune function can be affected by major stress, poor sleep,
and illness, which may help explain why some people notice shingles symptoms after periods of strain.
Real-life experiences with shingles recurrence (what people commonly report)
Shingles recurrence isn’t just a medical factit’s an experience. And if you’ve been through shingles once, the emotional reaction to a possible
recurrence is often immediate: “Not again.” Below are realistic, commonly described experiences people share with clinicians and support communities.
They’re not meant to diagnose you, but to help you feel less alone and more prepared.
The “I recognized it before the rash” moment
Many people with a second episode say the earliest clue wasn’t a visible rashit was the sensation. They describe a patch of skin that suddenly felt
sunburned, prickly, or hypersensitive, sometimes with a deep ache underneath. Because they’d felt it before, they didn’t dismiss it as “just a weird itch.”
The most helpful takeaway from this story pattern: if the sensation feels familiar and localized, reaching out early can speed up treatment.
The “I’m healthywhy me?” surprise
Another common experience comes from people who consider themselves generally healthymaybe in their 50s or 60s, exercising, eating reasonably well,
and not dealing with major health conditions. A second shingles episode can feel unfair, like the virus is ignoring the rules. In these cases, clinicians
often talk about immune aging (which happens to everyone) and the fact that recurrence can happen even without a dramatic trigger. For many in this group,
vaccination becomes a “let’s not roll the dice again” decision.
The “it hit during a stressful season” pattern
People frequently connect recurrence to periods where life got heavycaregiving, grief, job strain, travel exhaustion, or weeks of poor sleep. It’s not that
stress automatically “causes” shingles; it’s that stress can coincide with lower resilience (less sleep, more inflammation, more vulnerability to illness),
which can give dormant viruses an opening. The practical lesson people share: if you’re in a high-stress stretch, it may be worth prioritizing recovery habits
and checking in with your healthcare provider about prevention, especially if you’re eligible for Shingrix.
The immunocompromised experience: “I don’t have the luxury of waiting”
For people undergoing chemotherapy, living with autoimmune disease on immune-modulating therapy, or recovering from a transplant, recurrence can feel less
like a surprise and more like a known risk. A common theme is acting quickly: they tend to contact their care team early, document symptoms, and start
treatment promptly. They may also have more detailed discussions about vaccine timing (because the immune system’s calendar matters), pain control strategies,
and what symptoms should trigger urgent evaluation.
The lingering worry: “Is it going to keep coming back?”
After recurrence, many people worry that shingles will become a regular visitor. In reality, frequent recurrence is considered uncommon, but the worry makes
senseshingles pain can be intense, and uncertainty is stressful. What often helps is a clear prevention plan: confirm the diagnosis, address immune risk
factors when possible, and discuss vaccination and follow-up. People also report that having a “next time checklist” (who to call, what symptoms to watch,
how quickly to seek treatment) reduces anxiety because they’re not improvising when they’re already uncomfortable.
A grounded mindset that many people find helpful
A recurring theme in patient experiences is shifting from self-blame (“Did I cause this?”) to strategy (“What’s the best next step?”). Shingles recurrence
is usually about biology and immunity, not personal failure. The most effective approach is practical: recognize symptoms early, treat promptly, protect your
future risk with vaccination when eligible, and work with a clinician if recurrence raises questions about immune health.
Conclusion
Shingles recurrence is possible, but it isn’t inevitable. For most people, the best plan is straightforward: take symptoms seriously, get evaluated early
(especially if the rash is on the face or near the eye), treat promptly, and use prevention toolsparticularly vaccinationwhen appropriate. If shingles
keeps returning or appears unusually severe, it’s worth checking whether your immune system needs extra attention.