Table of Contents >> Show >> Hide
- What Is Brain Herniation?
- Why It Happens: Pressure Inside a Locked Box
- Types of Brain Herniation (The “Where Did the Tissue Go?” Map)
- Brain Herniation Symptoms: Warning Signs to Know
- How Doctors Diagnose Brain Herniation
- Treatment: How Doctors Reduce Pressure and Protect the Brain
- Recovery and Prognosis
- When to Seek Emergency Care
- FAQ
- Real-World Experiences (About ): What It Can Feel Like, and What Families Often Notice
“Herniation” is one of those medical words that sounds like it should come with a sirenand in this case, it kind of does.
Brain herniation happens when pressure inside the skull pushes brain tissue out of its usual position.
Because the skull is basically a hard, non-stretchy helmet you can’t take off, rising pressure has only a few “escape routes.”
When brain tissue shifts through those openings, vital areas (especially the brainstem) can get squeezed.
Translation: this is a medical emergency, not a “sleep it off and see how you feel tomorrow” situation.
This guide explains what brain herniation is, the most common symptoms, how doctors diagnose it, and the treatments used to lower pressure fast.
We’ll keep it clear, practical, and just lightly humorousbecause your brain deserves respect, but you deserve to understand what’s happening.
What Is Brain Herniation?
Brain herniation occurs when something inside the skull (like swelling, bleeding, or a mass) increases pressure and
forces brain tissue to shift from one compartment to another. Think of the brain as living in a tight studio apartment:
if a new “roommate” moves in (blood from a hemorrhage, fluid buildup, swelling), everyone gets shoved aroundfast.
Herniation isn’t a single disease. It’s usually the result of another problem, such as a traumatic brain injury,
stroke, brain tumor, infection, or hydrocephalus (too much cerebrospinal fluid).
Why It Happens: Pressure Inside a Locked Box
Your skull holds three main things: brain tissue, blood, and cerebrospinal fluid (CSF).
When the volume of one increases and the others can’t compensate enough, intracranial pressure (ICP) rises.
High ICP can reduce blood flow to the brain and can trigger herniation.
Common Causes
- Traumatic brain injury (TBI) from falls, crashes, sports injuries, or blows to the head
- Bleeding in or around the brain (hemorrhage, subdural/epidural hematoma)
- Stroke, especially large strokes that cause swelling
- Brain tumors (primary or metastatic) that add mass or cause swelling
- Brain infection or abscess that creates swelling and pressure
- Hydrocephalus (CSF buildup) or blocked CSF flow
- Severe lack of oxygen to the brain (hypoxia), which can cause swelling
- Structural conditions such as Chiari malformation (sometimes discussed as Arnold-Chiari)
The important takeaway: brain herniation usually means the brain is under dangerous pressure for a specific reason.
Treatment focuses on both relieving the pressure and fixing the underlying cause.
Types of Brain Herniation (The “Where Did the Tissue Go?” Map)
Doctors classify herniation based on where the brain shifts. You don’t need to memorize these terms,
but knowing the basics helps you understand what clinicians mean when they speak urgently (and in acronyms).
1) Subfalcine (Cingulate) Herniation
Brain tissue slides under a rigid membrane (the falx). This can compress blood vessels and reduce blood flow,
potentially worsening injury.
2) Transtentorial Herniation (Including Uncal Herniation)
Tissue moves downward past another membrane (the tentorium). Uncal herniation is a well-known subtype
involving the temporal lobe. It can compress nerves that control pupil size and eye movement, leading to
an unequal pupil or a poorly reactive pupil.
3) Central Herniation
The brain shifts straight downward, which may affect alertness and breathing as deeper structures become compressed.
4) Tonsillar Herniation
Tissue from the lower part of the brain (cerebellar tonsils) pushes through the opening at the base of the skull
(foramen magnum). This can compress the brainstem, which controls breathing and heart ratemaking it especially dangerous.
5) Upward Herniation
Less common, but it can happen when pressure in the back of the skull pushes tissue upward.
It’s still a “call everyone now” event in the hospital.
6) External Herniation
Tissue bulges outward through an opening in the skull (for example, after trauma or surgery).
This can still be serious because swelling may continue and circulation can be affected.
Brain Herniation Symptoms: Warning Signs to Know
Symptoms depend on the cause and the type of herniation, but there’s a general pattern:
worsening pressure leads to worsening brain function.
Some signs are early and non-specific; others are late and very concerning.
Possible Early Signs (Still Urgent)
- Severe or rapidly worsening headache
- Nausea and vomiting (especially repeated or “out of nowhere”)
- Increasing sleepiness, confusion, or difficulty staying awake
- Changes in vision (blurred vision, double vision)
- Weakness or numbness, especially on one side
- Seizures
Late / Emergency Signs (Call Emergency Services)
- Unequal pupil size or pupils that don’t react normally to light
- Abnormal breathing patterns
- Very high blood pressure with a slow heart rate (often discussed as “Cushing’s triad” when paired with irregular breathing)
- Loss of consciousness
- Coma
Not every person shows every symptom. But if someone has a serious head injury or known brain condition and starts
becoming increasingly confused, hard to wake, or develops unusual eye/pupil changes, treat it like an emergency.
How Doctors Diagnose Brain Herniation
Diagnosis is based on a combination of the patient’s story (what happened), a neurological exam, and imaging.
The goal is to identify dangerous pressure and the underlying cause quickly.
Neurological Exam
Clinicians look at alertness, speech, strength, coordination, reflexes, and eye findings (including pupil size and reaction).
Those details help localize which areas of the brain may be affected.
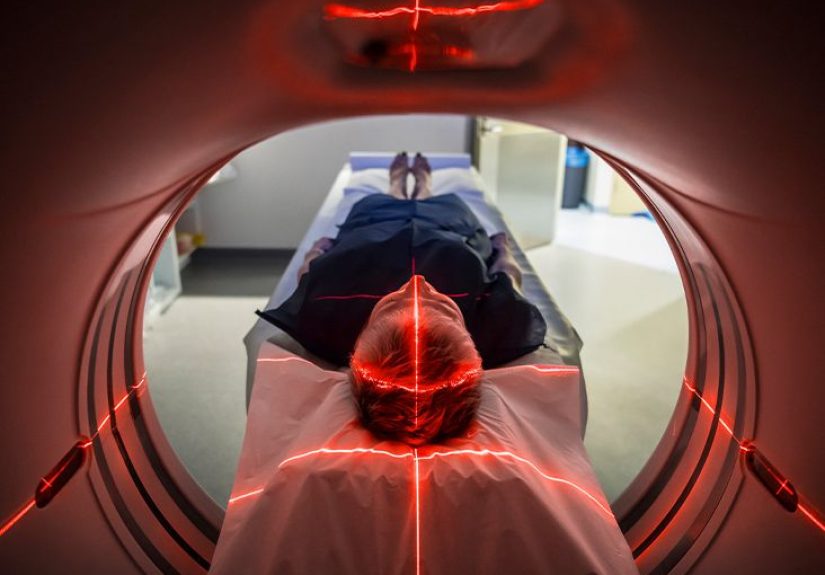
CT or MRI Imaging
A CT scan is often the fastest way to detect bleeding, swelling, hydrocephalus, or mass effect in an emergency.
MRI may provide additional detail in some cases, depending on stability and timing.
ICP Monitoring (In Certain Severe Cases)
In intensive care settingsespecially in severe traumatic brain injurydoctors may use specialized devices to measure ICP directly.
Normal ICP is often described in a low range, and sustained elevations above commonly used thresholds can be dangerous.
A Key Safety Point: Lumbar Puncture Timing Matters
A lumbar puncture (spinal tap) can be essential for diagnosing certain infections or bleeding patternsbut if ICP is dangerously high,
performing it at the wrong time can increase the risk of herniation. That’s why clinicians often consider brain imaging first
when elevated pressure is suspected.
Treatment: How Doctors Reduce Pressure and Protect the Brain
Brain herniation is treated like a race against time. The immediate goals are:
(1) maintain oxygen and blood flow, (2) lower intracranial pressure, and
(3) treat the cause (bleed, tumor, swelling, infection, fluid blockage).
1) Emergency Stabilization (The “ABC” Stuff That Saves Brains)
- Airway and breathing: Ensuring adequate oxygen; some patients need intubation and mechanical ventilation.
- Circulation: Supporting blood pressure so the brain continues to receive blood flow.
- Positioning: Often elevating the head of the bed and keeping the neck in a neutral position to promote venous drainage.
- Temperature and glucose control: Avoiding fever and extreme blood sugar swings, which can worsen brain injury.
- Pain and agitation control: In the ICU, sedation/analgesia may reduce pressure spikes.
2) Medications to Lower Brain Swelling and ICP (Osmotherapy)
Two common emergency options are mannitol and hypertonic saline.
Both pull fluid out of swollen brain tissue by shifting water into the bloodstream (via osmotic effects).
Selection depends on the clinical scenario, lab values (like sodium), and protocols.
- Mannitol: Long used to reduce elevated ICP in severe brain injury. It can be effective but requires careful monitoring
of blood pressure, kidney function, and serum osmolality. - Hypertonic saline: Also used to reduce ICP and cerebral edema. Different concentrations exist, and dosing/monitoring
are tightly managed in hospitals.
Important nuance: these therapies are designed to stabilize physiology and buy time.
They are not “magic erasers,” and they don’t replace treating the underlying cause.
3) Ventilation Strategies (Sometimes a Short-Term Bridge)
In certain emergency settings, clinicians may adjust ventilation to briefly lower carbon dioxide levels, which can reduce cerebral blood volume
and lower ICP temporarily. This is typically a short-term measure while definitive treatment (like surgery or drainage) is arranged,
because overly aggressive or prolonged changes can reduce brain blood flow.
4) Draining CSF to Relieve Pressure
If hydrocephalus or CSF pressure contributes, a neurosurgical team may place an external ventricular drain (EVD) (ventriculostomy)
to drain CSF and monitor pressure.
5) Surgery to Remove the Cause (or Make Space)
When a mass effect is driving herniation, surgery may be the most direct way to save brain tissue:
- Evacuation of a hematoma (removing a blood clot pressing on the brain)
- Tumor surgery (removing or reducing a tumor contributing to swelling/pressure)
- Decompressive craniectomy (temporarily removing part of the skull to allow swelling space)
Decompressive procedures can lower pressure when other measures aren’t enough, but they come with tradeoffs,
and outcomes depend on the person’s overall injury and how quickly treatment begins.
Recovery and Prognosis
Prognosis varies widely. The biggest drivers include:
how quickly pressure rose, how long critical structures were compressed, the underlying cause (bleed vs. tumor vs. infection),
the person’s overall health, and how quickly definitive treatment happened.
Some people recover with minimal long-term issues, especially if treatment occurs early and the cause is reversible.
Others may need longer rehabilitation for challenges such as weakness, speech difficulties, memory problems,
fatigue, or mood changes.
Rehab Often Matters as Much as the ICU
After stabilization, many patients benefit from physical therapy, occupational therapy, speech-language therapy,
and neuropsychological support. Recovery can look less like a straight line and more like a “two steps forward, one step back” dance
frustrating, but still progress.
When to Seek Emergency Care
Call emergency services immediately if someone has any of the following, especially after a head injury or with a known brain condition:
- Sudden severe headache with confusion, fainting, or seizures
- Worsening drowsiness or difficulty waking
- New weakness or numbness (especially one-sided)
- Unequal pupils or unusual eye movements
- Abnormal breathing
Brain herniation is not something to “wait out.” If you’re worried, it’s better to get evaluated and be told “good news”
than to gamble with time.
FAQ
Is brain herniation the same thing as a herniated disc?
Nope. A herniated disc involves spinal discs; brain herniation involves brain tissue shifting due to pressure in the skull.
Same word, wildly different stakes.
Can brain herniation be reversed?
Sometimes, yesespecially if the cause is treated quickly (like evacuating a bleed or draining CSF).
But outcomes depend on how severe the pressure was and how long critical areas were compressed.
What is “increased intracranial pressure” and how does it relate?
Increased intracranial pressure means pressure inside the skull is abnormally high.
It can reduce blood flow and can lead to herniation if severe or not treated promptly.
What treatments are most common first?
In emergencies, teams focus on stabilizing oxygenation and blood pressure, then rapidly lowering pressure with medications
(like hypertonic saline or mannitol), drainage (like an EVD), and/or surgery depending on the cause.
Real-World Experiences (About ): What It Can Feel Like, and What Families Often Notice
Brain herniation is usually discussed in dramatic, clinical language“mass effect,” “midline shift,” “impending herniation.”
But the lived experience often starts with something that doesn’t sound dramatic at all.
Families frequently describe a loved one who just seems “off”: unusually sleepy, slower to answer questions,
not quite tracking the conversation, or complaining of a headache that feels different from their usual headaches.
Sometimes the first clue is repeated vomiting that doesn’t match the situationno stomach bug, no suspicious leftovers,
just sudden nausea that won’t quit.
In emergency rooms, the pace can feel surreal: a rush to get imaging, quick neurological checks,
and a lot of staff repeating the same questions (“What’s your name? What day is it?”).
To clinicians, repetition is data. To families, it can feel like a strange pop quiz at the worst possible moment.
One of the most unsettling things relatives report is watching a person go from talking to confused to barely responsive
over a short span of time. That rapid change is one reason teams treat elevated pressure so aggressively.
ICU experiences often include machines, alarms, and more acronyms than a spaceship control room.
People remember the small details: the head of the bed kept elevated, careful positioning of the neck,
frequent checks of pupil size, and nurses explaining that these are “windows” into what the brain might be doing.
When interventions like osmotherapy are used, families may hear phrases like “We’re trying to buy time”
or “We’re trying to protect the brain while we treat the cause.” That can be oddly comforting:
it frames care as a plan, not chaos.
Recovery stories vary widely. Some patients remember little from the acute phase; others recall flashes
bright lights, fragmented voices, or intense fatigue afterward.
Many people describe the post-hospital period as unexpectedly challenging, even when the crisis is “over.”
Cognitive fatigue (getting mentally exhausted faster than before) is a common theme, as are mood changes.
Families often say the person looks physically “fine” but tires easily, struggles with concentration,
or feels overwhelmed in noisy environments. That’s when rehabilitation and follow-up care become the main event, not an afterthought.
Practical lessons from real-world caregivers tend to repeat:
keep a notebook of symptoms and questions, bring a current medication list,
and ask the care team what warning signs should trigger urgent re-evaluation after discharge.
Many families also recommend arranging help earlyrides, meals, school/work coordinationbecause recovery can be unpredictable.
And if you’re supporting someone after a brain injury or pressure event, patience is not just a personality trait;
it’s part of the treatment plan.







