Table of Contents >> Show >> Hide
- What Is Dermatillomania (Excoriation Disorder)?
- What Causes Dermatillomania?
- Signs You Might Be Dealing With Skin-Picking Disorder
- How Dermatillomania Is Diagnosed
- How to Treat Dermatillomania
- Practical Strategies That Make Treatment Work Better
- How to Support Someone With Dermatillomania
- When to Seek Medical Care Quickly
- FAQs
- Conclusion: You’re Not “Broken,” You’re Stuck in a Loop
- Real Experiences: What Dermatillomania Can Feel Like (and What Helps)
Dermatillomania (also called skin-picking disorder or excoriation disorder) is one of those conditions that sounds like a spell from a fantasy novel, but is actually a very real, very common mental health issue. It’s not “bad habits,” “lack of willpower,” or “you just need gloves.” It’s a brain-and-body loop that can be stubborn, sneaky, andyestreatable.
If you’ve ever looked down and thought, “How did my hands end up here again?” you’re not alone. People with dermatillomania often describe picking as automatic (happening without noticing) or focused (a strong urge that feels impossible to ignore). Either way, the behavior can cause distress, take up time, affect confidence, and make everyday thingslike mirrors, makeup, or short sleevesfeel complicated.
This guide breaks down what dermatillomania is, why it happens, and what actually helps, including therapy approaches like habit reversal training and CBT, plus medication options that may be considered with a clinician.
What Is Dermatillomania (Excoriation Disorder)?
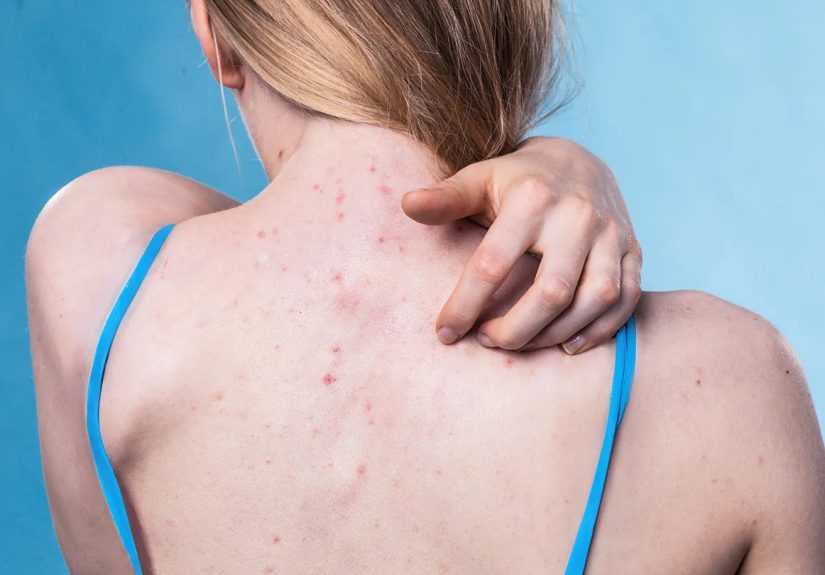
Dermatillomania is a condition involving recurrent skin picking that leads to skin damage and is paired with repeated attempts to stop. It becomes a disorder when it causes meaningful distress or interferes with school, work, relationships, or daily life.
It’s More Than “Everyone Picks Sometimes”
Lots of people pick at a hangnail or absentmindedly scratch a bump. With dermatillomania, the picking is persistent and difficult to control. It can also be time-consumingsometimes happening in short bursts many times a day, or in longer sessions without realizing how much time passed.
Where It Fits in Mental Health
Excoriation disorder is classified under Obsessive-Compulsive and Related Disorders. That doesn’t mean everyone with skin-picking disorder has OCD, but it does mean the behavior shares features like repetitive urges, relief after the behavior, and difficulty resistingeven when you really, really want to stop.
What Causes Dermatillomania?
There isn’t one single cause. Dermatillomania usually comes from a mix of brain biology, emotions, learning patterns, and environmental triggers. Think of it less like a “character flaw” and more like a habit loop with jet fuel.
The Urge–Relief–Regret Loop
Many people experience a pattern like this:
- Trigger: stress, boredom, a rough patch of skin, a mirror, bright bathroom lighting, a deadline
- Urge: tension, restlessness, “just one more,” or a strong need to “fix” something
- Behavior: picking (automatic or focused)
- Short-term payoff: relief, calm, satisfaction, “it feels smoother”
- After-effect: guilt, embarrassment, frustration, avoidance… which becomes the next trigger
Common Triggers and Risk Factors
Triggers vary, but these show up often:
- Stress and anxiety: picking can act like a pressure valve
- Boredom or understimulation: hands look for “something to do”
- Perfectionism and “fixing” urges: wanting to remove perceived imperfections
- Sensory factors: the feel of a bump, scab, dry patch, or uneven texture
- Skin conditions: acne, eczema, dry skin, or irritation can become “targets”
- Transitions and routines: after showers, during studying, while watching TV, scrolling, or gaming
Research and clinical guidance also note that skin-picking disorder frequently overlaps with conditions like anxiety and depression, and may occur alongside other body-focused repetitive behaviors (BFRBs) such as hair pulling or nail biting.
Signs You Might Be Dealing With Skin-Picking Disorder
Dermatillomania can look different from person to person, but some common signs include:
- Repeated picking that causes noticeable skin damage or ongoing irritated areas
- Difficulty stopping, even with strong motivation to quit
- Spending significant time picking or thinking about picking
- Avoiding social situations, photos, mirrors, or certain clothing because of skin concerns
- Feeling shame, secrecy, or frustration about the behavior
- Picking that gets worse during stress, fatigue, or certain routines
Important note: dermatillomania is not the same thing as intentional self-harm. People usually pick to reduce tension, soothe discomfort, or “fix” skin texturenot to cause pain. Still, the results can be distressing, which is why treatment matters.
How Dermatillomania Is Diagnosed
Diagnosis is typically made by a mental health professional (like a psychologist or psychiatrist). A primary care clinician or dermatologist may also help rule out medical causes and treat skin issues alongside behavioral care.
What Clinicians Look For
Clinicians often focus on:
- Whether picking is recurrent and causes skin damage
- Whether there have been repeated attempts to reduce or stop
- How much the behavior affects daily life and emotional well-being
- Whether symptoms are better explained by another condition, substance use, or a medical issue
If you’re wondering whether you “count,” here’s a practical rule of thumb: if picking feels out of control and is affecting your quality of life, it’s worth bringing up with a professional.
How to Treat Dermatillomania
Effective treatment usually targets two things at once: (1) the picking behavior and (2) the triggers and emotions around it. The good news is that there are evidence-based approachesno magical thinking required.
1) Therapy: CBT and Habit Reversal Training (HRT)
Cognitive behavioral therapy (CBT) is commonly recommended for skin-picking disorder. One of the best-known CBT tools for BFRBs is Habit Reversal Training (HRT).
HRT usually includes:
- Awareness training: noticing where, when, and how picking starts (including “autopilot” picking)
- Competing response: replacing picking with a different action that blocks it (like clenching fists gently, holding a fidget object, or pressing hands flat on thighs for a short time)
- Stimulus control: changing the environment to reduce triggers (more on that below)
Therapy may also include ComB (Comprehensive Behavioral) treatment, which looks at multiple drivers of pickingsensory, cognitive, emotional, environmental, and motor patternsand builds a personalized plan.
2) Acceptance and Commitment Therapy (ACT) and Mindfulness Tools
Some people benefit from adding ACT-style strategies, which focus on building tolerance for urges without acting on them, while staying aligned with values (like health, confidence, or being present with others).
Mindfulness isn’t about “emptying your mind.” It’s about catching the urge earlier and creating a pausejust long enough to choose a different response.
3) Medications: What May Help (With a Clinician’s Guidance)
There’s no single medication that works for everyone, and not everyone needs medication. But clinicians may consider options depending on symptoms, co-occurring anxiety/depression, and past treatment response.
- SSRIs: sometimes used because of the OCD-related nature of the disorder, especially when anxiety or depression is also present
- N-acetylcysteine (NAC): a supplement that has clinical trial evidence showing symptom reduction for some people with skin-picking disorder; it should still be discussed with a clinician because “over-the-counter” doesn’t automatically mean “right for you”
- Other options: may be considered by specialists on a case-by-case basis
If you’re considering NAC or any medication, the safest move is to talk to a healthcare professionalespecially if you take other medicines or have underlying health conditions.
4) Dermatology Support: Treat Skin Kindly, Not Like an Enemy
Because skin picking affects the skin barrier, it can help to involve a dermatologistparticularly if acne, eczema, or irritation is triggering the behavior. Treating underlying skin conditions can reduce “targets” and lower sensory triggers.
Also: gentle, consistent skincare is often more helpful than aggressive routines. If your bathroom cabinet looks like a science fair project, simplifying might actually reduce triggers.
Practical Strategies That Make Treatment Work Better
Therapy is the core for many people, but day-to-day strategies can make the difference between “I have a plan” and “I used the plan.”
Build Awareness Without Turning Your Life Into a Crime Scene Investigation
- Track when urges happen (time of day), where (bathroom, bed, desk), and what’s happening emotionally (stress, boredom, criticism, fatigue).
- Identify your “high-risk moments” (after showering, in front of mirrors, during homework, while watching shows).
Stimulus Control: Make Picking Inconvenient
The goal isn’t punishmentit’s creating friction so you have time to choose.
- Dim harsh mirror lighting or limit “inspection time”
- Keep nails trimmed if that reduces damage (not as a cure, but as harm reduction)
- Use a fidget object during TV/scrolling time
- Cover mirrors temporarily if mirrors are a major trigger
- Moisturize dry skin so texture triggers are less intense
Replace the Function, Not Just the Habit
If picking reduces anxiety, you’ll need other anxiety reducers. If picking fights boredom, you’ll need other stimulation. Examples:
- For stress: short breathing exercises, a quick walk, stretching, journaling
- For boredom: hands-busy activities (knitting, doodling, modeling clay)
- For sensory needs: textured fidgets, stress balls, smooth stones
How to Support Someone With Dermatillomania
If someone you care about struggles with skin picking, the most helpful things are usually the least dramatic:
- Skip “Just stop.” (If it worked, they’d be done already.)
- Use neutral language: “Do you want support right now?” beats “What did you do to your skin?”
- Encourage treatment gently: offer help finding a therapist trained in BFRBs
- Celebrate small wins: progress often comes in inches, not miles
When to Seek Medical Care Quickly
Consider prompt medical attention if there are signs of infection (like increasing warmth, spreading redness, swelling, or drainage), if pain is worsening, or if emotional distress is escalating. A clinician can help with both skin care and mental health support.
FAQs
Is dermatillomania the same as OCD?
Not exactly. It’s classified in the OCD-related disorders category, and there can be overlap, but many people with skin-picking disorder don’t meet criteria for OCD.
Does dermatillomania go away on its own?
Some people improve over time, but many find it’s persistent without targeted treatment. The good news is that behavioral therapies like HRT and CBT can be very effective.
What’s the most effective treatment?
Evidence commonly points to CBT approaches, especially habit reversal training and related behavioral models, as first-line treatment. Medication may help some people as an add-on.
Can teens have dermatillomania?
Yes. Skin picking often begins around adolescence, especially if acne or stress is present. Early support is a big advantage.
What if I pick “without realizing it”?
That’s common. Treatment still worksawareness training, stimulus control, and competing responses are designed for automatic patterns too.
Conclusion: You’re Not “Broken,” You’re Stuck in a Loop
Dermatillomania is tough precisely because it often works in the short termit reduces tension, fixes a perceived imperfection, or fills empty moments. But the long-term cost can be high. The most effective path forward is usually a combination of evidence-based therapy (especially CBT and habit reversal training), support for triggers and stress, andwhen appropriatemedical or medication support.
And if you take only one idea from this article, make it this: recovery isn’t about never having an urge again. It’s about building skills so the urge doesn’t run the show.
Real Experiences: What Dermatillomania Can Feel Like (and What Helps)
People often say the hardest part of dermatillomania is that it can feel both automatic and intensely personal. It’s not unusual to promise yourself, “I’m done,” and then find your hands back at it laterespecially during quiet moments. One common experience is “mirror time.” Someone might step into the bathroom to wash their hands and accidentally end up scanning their face or arms for texture. It starts with a quick check, then shifts into a focused “fixing” mode. A tiny bump can feel like a flashing neon sign. The brain says, “Just smooth it out,” and the action follows before the person fully realizes what’s happening.
Others describe picking as a stress response that shows up when the day finally slows down. A student might get through school holding it together, then start picking while doing homework, scrolling, or watching videosalmost like the nervous system is trying to “unwind,” but picked the wrong tool for the job. Some people call it “the aftershock”: the picking doesn’t always happen during peak stress, but right after, when adrenaline drops and the brain searches for relief.
Many people also talk about how shame keeps the cycle alive. They hide irritated areas with clothing or makeup, avoid bright lighting, and skip activities they actually want to do. The secrecy adds pressure. Then pressure triggers picking. It’s a frustrating feedback looplike your brain is playing a prank, but forgot to tell you the punchline.
In therapy, a big turning point is often learning to treat the behavior like data, not a moral failing. Instead of “I messed up again,” it becomes “Interestingthis happened after I stayed up late,” or “This is worse when I’m hungry and scrolling in bed.” That shift matters because it leads to action. People start building “friction” into high-risk moments: keeping hands busy with a fidget while studying, changing bathroom lighting, setting a short timer for skincare routines, or doing a two-minute grounding exercise before mirror time. These aren’t magic tricks; they’re practical ways to reduce autopilot behavior.
Another common win is learning a competing response that actually fits the situation. For example, someone who picks while watching TV might hold a textured object and keep both hands occupied. Someone who picks in the bathroom might switch to a simple routine: wash, moisturize, step awayno inspections. Someone who picks at rough skin might focus on gentle skincare and hydration to reduce the sensory “hook” that starts the urge. The goal is not perfectionit’s fewer triggers, shorter episodes, and faster recovery when it happens.
People in recovery often describe progress as “two steps forward, one step back,” but with a meaningful difference: the setbacks get smaller, and the bounce-back gets faster. Over time, many learn that urges are not orders. They’re signalssometimes that you’re stressed, overtired, lonely, bored, or anxiousand signals can be answered with healthier tools. That’s when dermatillomania starts shrinking from a life-rule into a manageable challenge.