Table of Contents >> Show >> Hide
- Rubella at a Glance
- Causes: What Actually Triggers Rubella?
- Symptoms: What Rubella Looks and Feels Like
- Rubella vs. Measles: Same Nickname Energy, Different Disease
- Complications: When Rubella Becomes a Bigger Problem
- Diagnosis: How Rubella Is Confirmed
- Treatments: What Helps, What Doesn’t, and What to Avoid
- Prevention: The Real Rubella Superpower
- What to Do After Exposure
- When to Seek Medical Care
- Conclusion
- Real-Life Experiences and Lessons (What Rubella Looks Like Beyond the Textbook)
Rubellaoften nicknamed “German measles”is one of those illnesses that sounds scarier than it usually is… until you add one crucial detail:
pregnancy. For most people, rubella is a mild viral infection that can look like a short “three-day” rash with low-grade fever and some sniffly, flu-ish vibes.
But for an unborn baby, rubella can be devastating. That’s why public health takes it seriously, even in a country where the vaccine has made rubella uncommon.
Also, quick clarification: rubella is not the same as measles (rubeola). They share a similar “rash guest star” moment, but they’re caused by different viruses and don’t behave the same way.
Think of rubella as measles’ quieter cousinless dramatic symptoms, less chaos in most cases, but with a high-stakes plot twist for pregnancy.
Rubella at a Glance
- What it is: A contagious viral infection that often causes a mild rash and fever.
- How it spreads: Mainly through respiratory droplets (coughing/sneezing) and close contact.
- Why it matters: Infection during pregnancy can lead to miscarriage, stillbirth, or congenital rubella syndrome (CRS).
- Why you don’t hear about it much: Routine vaccination has made rubella rare in the U.S.but “rare” is not the same as “gone forever.”
Causes: What Actually Triggers Rubella?
Rubella is caused by the rubella virus. Humans are the natural hostmeaning this isn’t a “caught it from my cat” situation.
The virus primarily spreads through the air when an infected person coughs or sneezes, or through close contact with their respiratory secretions.
How long after exposure do symptoms show up?
Rubella has a sneaky runway. The incubation period (time between exposure and symptoms) is typically about 2–3 weeks.
This matters because someone can be contagious before they realize anything’s wrong.
When is someone contagious?
People with rubella are generally most contagious around the time the rash appears. But the virus can spread before the rash shows up and continue spreading for about a week after.
Translation: by the time you say, “Hmm, that rash is new,” the virus may have already RSVP’d to a few other people’s calendars.
Symptoms: What Rubella Looks and Feels Like
Rubella symptoms can range from “barely noticeable” to “I feel gross but still capable of scrolling social media.”
In fact, a significant number of people infected with rubella have no symptoms at allyet they can still transmit the virus.
Common rubella symptoms
- Rash: Often starts on the face and then spreads downward to the trunk, arms, and legs.
- Low-grade fever: Usually mild compared with many other viral illnesses.
- Swollen lymph nodes: Especially behind the ears and at the back of the neck.
- Cold-like symptoms: Runny nose, sore throat, mild cough (not always).
- Headache, fatigue, general malaise: The “I’d like to be a blanket burrito today” feeling.
- Joint aches (arthralgia): More common in teens and adults, especially women.
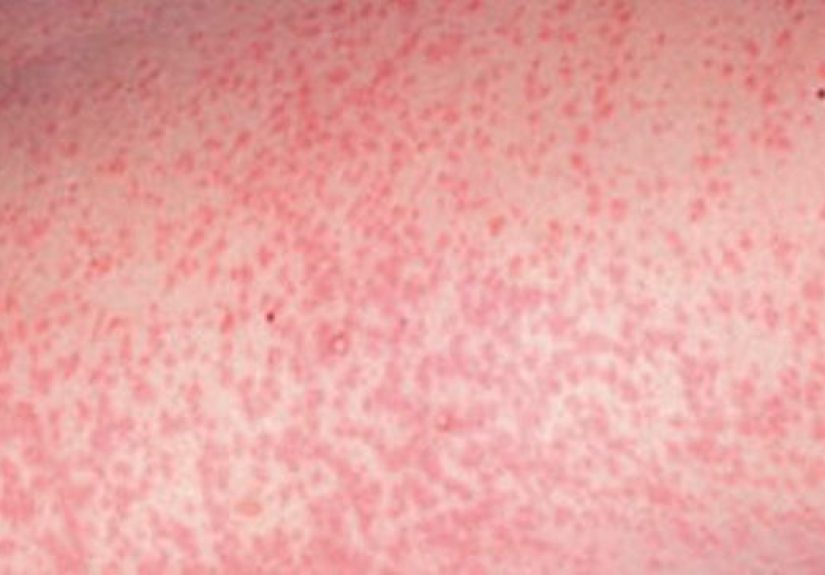
The rubella rash: the “three-day cameo”
The rash is often described as pink or light red and may be subtle, especially on some skin tones. It typically lasts a few days.
Because many viruses can cause similar rashes, clinicians often avoid “rash-guessing games” and confirm rubella with lab testing.
Kids vs. adults
Young children may have mild symptoms or just a rash. Teens and adults are more likely to notice systemic symptoms like joint pain,
fatigue, and swollen lymph nodes. The overall pattern is still usually mildagain, with the major exception of pregnancy risk.
Rubella vs. Measles: Same Nickname Energy, Different Disease
Because rubella is called “German measles,” people assume it’s basically measles with a fancy passport stamp. Not quite.
Here are some practical differences:
- Cause: Rubella virus (rubella) vs. measles virus (measles/rubeola).
- Typical severity: Rubella is often mild; measles can be severe and lead to serious complications.
- Fever: Rubella tends to have a mild fever; measles often comes with higher fever and more intense illness.
- Classic extras: Measles is known for cough, runny nose, red eyes, and Koplik spots; rubella is known for lymph node swelling and joint aches.
- Pregnancy concern: Rubella is especially notorious for fetal harm (CRS) if infection occurs during pregnancy.
Complications: When Rubella Becomes a Bigger Problem
Most people recover from rubella without lasting issues. But complications can happen, and the risk profile changes dramatically if the infected person is pregnant.
Possible complications (non-pregnancy)
- Arthritis/arthralgia: Joint pain and swelling can linger, particularly in adult women.
- Rare neurologic complications: In uncommon cases, encephalitis (brain inflammation) can occur.
- Secondary infections: Like many viral illnesses, rubella can sometimes set the stage for other issues, depending on overall health.
Rubella in pregnancy: why doctors take it personally
Rubella infection during pregnancy can pass to the fetus and cause serious harm. The earlier in pregnancy infection occurs,
the higher the risk of severe fetal outcomes.
Congenital Rubella Syndrome (CRS)
When a fetus is infected in utero, the result may be congenital rubella syndrome, a set of birth defects and developmental problems.
CRS can involve:
- Hearing loss
- Eye problems (including cataracts)
- Heart defects
- Growth and developmental delays
- Other systemic complications depending on severity
CRS doesn’t have a magic “undo” button. Many effects are permanent, which is why preventionespecially vaccination before pregnancy and community immunityis the main strategy.
Diagnosis: How Rubella Is Confirmed
Here’s the tricky part: a rubella rash can resemble many other viral rashes. So while history and physical exam matter,
healthcare professionals often rely on lab tests to confirm rubella.
Common diagnostic approaches
- Blood tests for antibodies: Looking for immune markers that suggest recent infection or prior immunity (from vaccination or past infection).
- Viral testing: In certain situations, tests may detect the virus directly (for example, in specialized labs or public health settings).
- Pregnancy-related screening: Many prenatal panels include rubella immunity testing so clinicians know whether a pregnant patient is protected.
Because rubella is a public health concernparticularly due to pregnancy risksuspected cases may be reported to local health departments
so contacts can be identified and outbreaks can be contained.
Treatments: What Helps, What Doesn’t, and What to Avoid
There’s no specific antiviral medication that “cures” rubella in the way antibiotics treat certain bacterial infections.
Treatment is usually supportive, aimed at making you more comfortable while your immune system handles the virus.
Supportive care (typical recommendations)
- Rest: Your immune system does its best work when you’re not trying to power through a “normal schedule” out of spite.
- Fluids: Especially if fever is present.
- Fever/pain relief: Over-the-counter options may help, but choices can vary by age, medical history, and pregnancy status.
- Comfort measures: Light clothing, lukewarm baths, and managing itch if the rash is irritating.
Isolation to prevent spread
A key part of “treatment” is actually protecting others. Because rubella can spread before the rash appears,
it’s especially important to follow a clinician’s guidance on staying home, avoiding close contact, and protecting high-risk peopleparticularly anyone who is pregnant.
If the patient is pregnant
Pregnancy changes the entire medical conversation. A pregnant person with suspected rubella should contact their healthcare professional promptly.
Management may involve confirmatory testing, specialist consultation, and public health guidance. This is not a “wait and see” moment.
Prevention: The Real Rubella Superpower
The reason rubella is now uncommon in the U.S. is simple and powerful: vaccination.
The measles-mumps-rubella vaccine (MMR) protects against rubella and helps prevent the congenital rubella syndrome cases
that historically caused significant disability and pregnancy loss.
MMR vaccine schedule basics
In the U.S., routine childhood vaccination typically includes two doses: one around the end of the first year of life and a second dose in early childhood.
This schedule helps build strong immunity across the community.
Rubella immunity and pregnancy planning
Because the MMR vaccine is a live attenuated vaccine, it’s generally not given during pregnancy.
For people planning a pregnancy, clinicians often recommend checking rubella immunity and getting vaccinated ahead of time if needed.
Guidance commonly advises receiving rubella vaccination at least about a month before pregnancy (or in the postpartum period if not previously vaccinated).
What about adults?
Adults who aren’t sure about their vaccine statusespecially those who travel internationally, work in healthcare, or are around young childrenmay benefit from reviewing immunization records.
If records are unclear, a clinician can advise whether vaccination or blood testing for immunity makes sense.
What to Do After Exposure
If you’ve been around someone with suspected or confirmed rubella, your next steps depend on your risk level and immunity status.
Here’s a practical, common-sense approach to discuss with a clinician:
- Check vaccination records: Two documented MMR doses usually indicates strong protection.
- Ask about immunity testing: Especially if pregnancy is involved or planned soon.
- Watch for symptoms: Rash, fever, swollen lymph nodes, joint aches.
- Protect pregnant contacts: If you’re sick or possibly contagious, avoid close contact with pregnant people and let your clinician know.
- Follow public health guidance: In certain cases, health departments may provide instructions to reduce spread.
When to Seek Medical Care
Rubella is often mild, but you should contact a healthcare professional promptly if:
- You are pregnant (or might be) and have been exposed or develop symptoms.
- You have a rash plus fever and you’ve recently traveled or were around an outbreak.
- You have symptoms that are severe, persistent, or unusual for you.
- An infant has signs suggestive of congenital infection (this requires urgent medical evaluation).
Conclusion
Rubella is a classic example of a disease that’s usually mild for the individual but potentially severe for a developing fetus.
That’s why it remains medically and socially important: it’s not just about “getting through a rash,” it’s about protecting pregnancies and preventing congenital rubella syndrome.
The good news is that the tools we haveespecially the MMR vaccine and routine immunity screeningare extremely effective at keeping rubella uncommon.
When rubella does appear, quick recognition, lab confirmation, supportive care, and responsible isolation help protect the people who need protection most.
Real-Life Experiences and Lessons (What Rubella Looks Like Beyond the Textbook)
If you ask clinicians who trained after widespread vaccination, many will tell you the same thing: they’ve read about rubella far more than they’ve seen it.
That’s the quiet success story of immunizationlike having a great security system that makes break-ins rare. But when rubella does pop up, it often arrives in
very ordinary moments, which is exactly why it can spread if people dismiss it as “just a little rash.”
One common scenario looks like this: a child comes home from school with a faint rash and low fever. The parent does what parents dochecks temperature,
offers fluids, and starts mentally replaying every snack, soap, and playground plant that could possibly cause a reaction. The next day, the rash spreads,
the fever stays mild, and the child is mostly finemaybe a bit cranky, maybe extra sleepy. It’s easy to assume it’s another routine virus.
But a careful clinician asks about recent travel, vaccination status, and whether anyone in the family is pregnant or trying to conceive.
That’s when rubella shifts from “mild inconvenience” to “important public health puzzle.”
Another experience shows up in young adults: someone in their twenties develops swollen lymph nodes behind the ears, low fever, and joint aches that make
typing feel like a tiny finger workout routine. They might laugh it off“I think I’m allergic to adulthood”until a light rash appears.
Because joint symptoms can be more noticeable in adults (especially women), they may seek care for pain rather than the rash itself.
In these cases, confirming the cause matters, not just for the patient’s comfort but to prevent exposing someone who’s pregnant.
The most emotionally charged stories involve pregnancy. Imagine a person early in pregnancy who learns they were exposed at a gathering where a guest
later developed a rash. Suddenly, every detail becomes urgent: “Was I vaccinated? Am I immune? What does this mean for my baby?”
The next steps typically involve prompt contact with a healthcare professional, blood tests to assess immunity or recent infection,
and sometimes consultation with specialists. Even when results are reassuring, the waiting period can feel endless.
Many people describe this as a moment that transformed “vaccines are a good idea” into “vaccines are a community promise.”
There are also practical, empowering experiences on the prevention side. People planning pregnancy sometimes discover during routine care that they are not immune to rubella.
It can be surprisingespecially if they assume childhood vaccines covered everything. The solution is usually straightforward:
vaccination before pregnancy (with appropriate timing guidance) or vaccination postpartum if already pregnant.
For many, this becomes a “future-me thank you” moment: one small appointment that dramatically reduces risk.
The biggest lesson from real-world rubella moments is that prevention isn’t abstract. It’s a chain of small choiceskeeping vaccine records, getting recommended doses,
checking immunity when planning pregnancy, and staying home when sickthat protects the most vulnerable people you may never even meet.
Rubella is mild enough to be overlooked, which is exactly why taking it seriously is the kindest move in the room.