Table of Contents >> Show >> Hide
- What Is Rheumatoid Arthritis, Really?
- Why Disease Progression Matters
- How Rheumatoid Arthritis Progresses
- Common Early Signs That Should Not Be Ignored
- What Can Make RA Progress Faster?
- How Doctors Track Disease Progression
- Can Rheumatoid Arthritis Progression Be Slowed?
- Flares, Remission, and the Myth of a Straight Line
- Complications Beyond the Joints
- Living Well While Managing Progression
- When to Call a Doctor
- Conclusion
- Experiences Related to Rheumatoid Arthritis Disease Progression
Rheumatoid arthritis, or RA, is one of those conditions that sounds simple until you actually meet it. On paper, it is an autoimmune disease that causes inflammation in the joints. In real life, it can feel more like your immune system hired the wrong security team, panicked, and started tackling your own joints for no good reason. The result is pain, stiffness, swelling, fatigue, and, if the disease stays active for too long, progressive damage that can affect movement, independence, and even organs outside the joints.
The good news is that rheumatoid arthritis progression is not a straight, unstoppable slide. Modern treatment has changed the outlook dramatically. Many people now reach low disease activity or remission, and some avoid the joint damage that used to be much more common. Still, understanding how RA can progress matters, because early recognition and timely treatment make a huge difference.
What Is Rheumatoid Arthritis, Really?
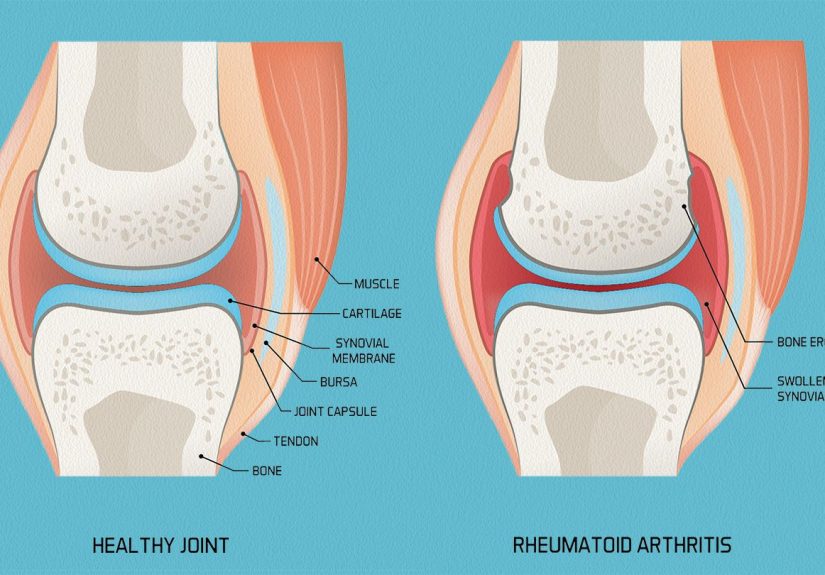
RA is a chronic inflammatory autoimmune disease. Instead of attacking germs, the immune system mistakenly targets the synovium, the lining around the joints. That inflammation can thicken the joint lining, increase pain and stiffness, and gradually damage cartilage and bone. RA often starts in smaller joints such as the hands, wrists, and feet, and it tends to affect both sides of the body in a fairly symmetrical pattern.
Unlike osteoarthritis, which is often described as wear and tear, rheumatoid arthritis is driven by an immune response. That distinction matters because disease progression in RA is not just about aging joints. It is about ongoing inflammation. And inflammation, unfortunately, does not always stay politely inside one knuckle. RA can also affect the eyes, lungs, heart, blood vessels, skin, and more.
Why Disease Progression Matters
When people hear the word “progression,” they often imagine a neat timeline. RA rarely behaves that way. It is more like a moody weather system. Some days are mild. Some are stormy. Some people have long quiet periods. Others deal with repeated flares that slowly add up over time. Disease progression in rheumatoid arthritis is less about one dramatic event and more about what happens when inflammation hangs around too long.
Persistent inflammation can lead to:
Joint pain that becomes more frequent or severe.
Morning stiffness that lasts longer.
Reduced range of motion.
Damage to cartilage and bone.
Joint deformity and loss of function.
Fatigue that feels bigger than “just being tired.”
Complications outside the joints.
This is exactly why doctors focus so heavily on early diagnosis, regular follow-up, and “treat-to-target” care. The target is usually remission or, at minimum, low disease activity.
How Rheumatoid Arthritis Progresses
Not everyone moves through RA the same way, and not every doctor uses a strict staging system. Still, it helps to think of rheumatoid arthritis progression in broad phases.
1. Early Inflammation
In the earliest stage, the immune system is already active, and inflammation is building in and around the joints. A person may feel sore, stiff, or unusually tired before obvious swelling shows up. This is one reason RA can be tricky early on. People may blame long workdays, bad sleep, stress, aging, or a suspiciously aggressive jar lid.
During this phase, joint damage may not yet be visible on X-rays. But symptoms are real. Hands may feel puffy in the morning. Feet may ache before the first coffee. Wrists may protest during typing, driving, or carrying groceries. Early RA often whispers before it shouts.
2. Cartilage Damage and Loss of Motion
If inflammation continues, it can begin to damage cartilage, the tissue that helps joints move smoothly. This is where stiffness may last longer, flexibility starts to drop, and daily tasks become oddly dramatic. Opening a bottle, buttoning a shirt, or turning a doorknob can begin to feel like a personal insult.
This middle phase often brings more noticeable functional problems. You may still look “fine” from across the room, but your joints may strongly disagree.
3. Bone Erosion and Structural Changes
Ongoing inflammation can eventually erode bone. At this point, rheumatoid arthritis is no longer just causing symptoms; it may be reshaping the joint itself. Pain can become more persistent, grip strength may weaken, and deformities may begin to appear. The hands and feet are especially vulnerable, though many joints can be affected.
This is the part of RA progression doctors work hard to prevent, because structural joint damage can be irreversible.
4. Advanced Disease and Systemic Impact
In advanced RA, the consequences may extend well beyond the joints. Some people develop nodules, dry eyes, dry mouth, lung problems, cardiovascular issues, osteoporosis, nerve compression, or other inflammatory complications. Function may be significantly limited, and simple tasks can require planning, pacing, and adaptive tools.
That said, “advanced” does not mean “inevitable.” With earlier and more targeted treatment, many people never reach the most severe forms of rheumatoid arthritis progression.
Common Early Signs That Should Not Be Ignored
One of the biggest mistakes with RA is assuming it has to look dramatic right away. It often does not. Early signs can be subtle, annoying, and weirdly easy to dismiss.
Watch for patterns such as:
Morning stiffness lasting 30 minutes or more.
Pain, swelling, or tenderness in more than one joint.
Symptoms affecting the same joints on both sides of the body.
Ongoing fatigue, low-grade fever, or loss of appetite.
Symptoms that last for six weeks or longer.
Trouble with fine motor tasks like typing, gripping, or buttoning clothes.
RA often begins gradually. That slow start can fool people into waiting too long.
What Can Make RA Progress Faster?
Several factors can influence how rheumatoid arthritis behaves. Some are biological, some are lifestyle-related, and some come down to how quickly treatment begins.
Delayed Diagnosis
The earlier RA is recognized and treated, the better the chance of slowing damage. Waiting months or years gives inflammation more time to settle in and leave a mess behind.
Uncontrolled Inflammation
Frequent flares, persistent swelling, and elevated disease activity can all push progression forward. RA does not need to be dramatic every day to cause damage. A steady simmer can be just as troublesome as a boil.
Smoking
Smoking is strongly associated with rheumatoid arthritis risk and worse outcomes. If RA needed a worst friend, tobacco would be near the top of the list.
High-Risk Antibody Patterns
Blood tests such as rheumatoid factor and anti-CCP antibodies can help support diagnosis. In some cases, these markers are also associated with a higher chance of more persistent or damaging disease.
Medication Gaps
Stopping medication without medical guidance, stretching doses, or avoiding follow-up appointments can let inflammation regain momentum. RA loves unattended chaos.
How Doctors Track Disease Progression
There is no single magic test for rheumatoid arthritis. Diagnosis and monitoring usually rely on a combination of symptoms, physical examination, blood work, and imaging.
Medical History and Joint Exam
Doctors look for patterns: which joints hurt, how long stiffness lasts, whether symptoms are symmetrical, and how much daily life is affected.
Blood Tests
Common tests include ESR and CRP, which reflect inflammation, plus rheumatoid factor and anti-CCP antibodies. These results help build the picture, but none of them work as a solo act.
Imaging
X-rays, ultrasound, and MRI can help detect inflammation or damage. Imaging is especially useful when symptoms and lab results do not tell the full story.
Disease Activity Scores
Rheumatologists often use structured scoring tools to monitor whether RA is active, improving, or slipping out of control. That helps guide medication changes instead of relying only on guesswork or vibes.
Can Rheumatoid Arthritis Progression Be Slowed?
Yes, and this is the most important part of the whole conversation. RA progression can often be slowed significantly, and in many people it can be controlled well enough to preserve function and quality of life.
DMARDs
Disease-modifying antirheumatic drugs are the backbone of treatment because they target the disease process, not just the pain. Methotrexate is often the first major player on the team, though other conventional DMARDs may be used too.
Biologics and Targeted Therapies
If standard DMARDs are not enough, biologic drugs or targeted synthetic medications may be added. These treatments focus on specific inflammatory pathways and can be highly effective in reducing disease activity.
Corticosteroids and NSAIDs
These may help control symptoms and calm inflammation, especially during flares, but they are usually not the long-term foundation for preventing progression.
Physical and Occupational Therapy
These therapies help protect joints, improve movement, and make daily tasks easier. Sometimes the smallest adjustment, like a new grip aid or better hand positioning, feels absurdly helpful.
Lifestyle Support
Low-impact exercise, smoking cessation, good sleep, stress management, balanced nutrition, and maintaining muscle strength all support long-term joint health. No, kale is not a miracle drug. But lifestyle choices do matter.
Flares, Remission, and the Myth of a Straight Line
RA progression is not always linear. Many people cycle through flares and quieter periods. A flare can bring worse pain, swelling, stiffness, and fatigue for days, weeks, or sometimes longer. Triggers may include infections, stress, smoking, overexertion, or suddenly stopping medications. Sometimes there is no clear trigger at all, because RA occasionally likes to be mysterious just for fun.
Remission, on the other hand, means there are few or no visible signs of disease activity. That is wonderful, but it does not necessarily mean RA is cured. Remission is better understood as controlled disease, not a permanent eviction notice.
Complications Beyond the Joints
Rheumatoid arthritis is a systemic disease, which means it can involve more than joints. That is one reason disease progression deserves respect.
Possible complications include:
Dry eyes and dry mouth.
Rheumatoid nodules under the skin.
Anemia.
Carpal tunnel syndrome.
Osteoporosis, especially with long-term inflammation or steroid use.
Lung inflammation or interstitial lung disease.
Increased cardiovascular risk.
Higher infection risk, partly because some treatments suppress the immune system.
This does not mean every person with RA will develop these issues. It means monitoring matters, and “it only affects my hands” is not always the full story.
Living Well While Managing Progression
Living with RA is often a balancing act between staying active and not overdoing it, between being hopeful and being realistic, and between wanting independence and accepting help when help is smart. Many people with RA become experts in pacing, joint protection, strategic rest, and the fine art of pretending a heating pad is medical equipment and not a best friend.
The emotional side is real too. Pain is tiring. Fatigue is frustrating. Invisible symptoms can make people feel misunderstood. That is why long-term RA care works best when it includes not only medications and monitoring, but also support, education, and practical coping tools.
When to Call a Doctor
Seek medical attention if you notice new joint swelling, worsening morning stiffness, ongoing fatigue, reduced function, or flares that are becoming more frequent. Prompt care is especially important if you develop shortness of breath, chest pain, major vision changes, signs of infection, or severe medication side effects.
In rheumatoid arthritis, “I’ll wait and see” sometimes turns into “I wish I had called sooner.”
Conclusion
Rheumatoid arthritis disease progression is best understood as the result of ongoing inflammation over time. It often begins quietly, may unfold in waves, and can range from mild intermittent symptoms to significant joint and systemic complications. But modern RA care has changed the script. Early diagnosis, disease-modifying treatment, regular monitoring, and healthy daily habits can slow progression, protect joints, and help many people live full, active lives.
If there is one takeaway worth taping to the fridge, it is this: rheumatoid arthritis is serious, but it is also treatable. The earlier it is recognized and addressed, the better the chances of staying ahead of the disease instead of constantly chasing it.
Experiences Related to Rheumatoid Arthritis Disease Progression
The following experiences are written as realistic composite examples based on common patient patterns, not as direct individual testimonials.
One common experience with early RA progression is confusion. A person may wake up with stiff fingers, blame too much typing, and move on. Then the same thing happens again. A few weeks later, the wrists hurt too. Then the feet join the rebellion. At first it can feel random, almost silly, because the symptoms come and go. People often say they started wondering whether they were just tired, stressed, overworked, or somehow suddenly bad at sleeping. That uncertainty is part of why RA can be diagnosed later than ideal.
Another common experience is the mismatch between appearance and reality. Someone with RA may look perfectly fine while quietly fighting to open a water bottle, hold a steering wheel, or stand up after sitting for too long. Morning routines can become miniature obstacle courses. Brushing hair, fastening a bra, making breakfast, or walking downstairs may take twice the effort and ten times the patience. By the time the person is dressed and smiling in public, they may already feel like they have completed an Olympic event that nobody else saw.
Flares also shape the lived experience of disease progression. People often describe them as interruptions that arrive without good manners. A flare can cancel plans, derail work, wreck sleep, and make ordinary tasks feel heavy. The hardest part is sometimes not the pain itself but the unpredictability. You make plans based on Tuesday’s body, and Wednesday’s body files a formal complaint. That unpredictability can create anxiety, especially when someone is trying to stay employed, care for family, or simply feel dependable.
Medication can be both a relief and a learning curve. Many people feel hopeful when treatment starts, then frustrated when it does not work instantly. Some RA medications take time, and that waiting period can feel long when your hands are throbbing and your socks suddenly seem designed by your enemies. But when the right treatment plan clicks, the difference can be dramatic. People often describe getting back pieces of life they did not realize they had been losing: cooking without pain, walking farther, typing faster, sleeping better, laughing more, and thinking less about every single joint in their body.
There is also a powerful emotional shift that happens when people understand that remission is possible, even if cure is not. That idea changes the story from “my body is falling apart” to “this is something I can manage.” Many people become more attentive to sleep, smoking cessation, exercise, stretching, stress, and follow-up care because they can see the payoff in real time. They learn the signs of an oncoming flare. They keep track of fatigue. They speak up earlier. They stop trying to tough it out for no reason other than pride and begin working with the disease instead of pretending it does not exist.
Perhaps the most encouraging shared experience is this: people often become far more capable than they expected. Not because RA is easy, but because education, treatment, support, and consistency make a real difference. Progression is not just about what RA does. It is also about what patients and clinicians do in response. And that response can change everything.