Table of Contents >> Show >> Hide
Tenosynovial giant cell tumor, or TGCT, is one of those conditions that sounds like a password you would forget immediately, yet it can have a very real effect on daily life. It develops in the synovium, tendon sheath, or bursa around a joint. In plain English, it is a growth that starts in the soft tissue that helps joints and tendons move smoothly. The good news is that TGCT is usually benign, which means it is not considered cancer in the usual sense. The less-fun news is that “benign” does not always mean “harmless.” TGCT can still grow, crowd a joint, damage nearby structures, limit movement, and make simple tasks feel far more dramatic than they should.
For some people, TGCT begins as a small lump near a finger or wrist. For others, it shows up as a stubbornly swollen knee, aching ankle, or stiff hip that just will not cooperate. Because the symptoms can imitate sports injuries, arthritis, or other joint problems, diagnosis is often delayed. That is one reason this condition deserves more attention than its obscurity suggests.
This guide breaks down the main types of TGCT, the symptoms to watch for, how doctors diagnose it, what treatment looks like today, and what the patient experience often feels like in real life. In other words, everything you wanted to know about TGCT but were too busy icing your knee to ask.
What Is Tenosynovial Giant Cell Tumor?
TGCT is a rare tumor-like growth that forms in the lining of joints, tendon sheaths, or bursae. Older terms still show up often, which can make the topic confusing fast. Localized disease in smaller structures, especially around the fingers and hand, has long been called giant cell tumor of the tendon sheath. Diffuse disease affecting a larger joint, especially the knee, is often referred to as pigmented villonodular synovitis, or PVNS. Today, these conditions are generally grouped under the broader umbrella of TGCT.
Although TGCT usually does not spread to distant parts of the body, it can behave in a locally aggressive way. That means it may thicken the joint lining, trigger inflammation, press on nearby tissue, erode bone, and gradually interfere with motion. A small lesion may be annoying. A diffuse lesion can be life-disrupting. Malignant TGCT exists, but it is extremely rare, and most cases people read about online are not malignant.
Types of TGCT
Localized TGCT
Localized TGCT is the more limited form. It usually appears as a single nodule or small lesion and is often found in the hands, wrists, fingers, or around a tendon sheath. It tends to grow more slowly and is less likely than diffuse disease to invade an entire joint. Many people first notice it as a lump that seems oddly persistent, like an unwelcome houseguest with no sense of timing.
This type is often easier to remove surgically, and outcomes are generally better when the lesion can be fully excised. That does not mean recurrence never happens, but localized disease usually behaves in a more manageable way than the diffuse form.
Diffuse TGCT
Diffuse TGCT is the more aggressive sibling. Instead of one tidy nodule, it can involve broad areas of synovial lining and spread throughout a joint. The knee is the classic trouble spot, but the ankle, hip, shoulder, foot, elbow, and other joints can also be affected. Diffuse disease is more likely to cause pain, swelling, repeated fluid buildup, stiffness, locking, and long-term joint damage.
Because diffuse TGCT can infiltrate tissue rather than sit politely in one spot, it is harder to remove completely. That is why recurrence is a major part of the conversation. In real-world studies and patient registries, diffuse disease has shown a much heavier burden of repeat procedures, recurring symptoms, and quality-of-life problems than localized disease.
Symptoms of TGCT
TGCT symptoms vary by size, location, and type, but the usual pattern includes joint pain, swelling, stiffness, and reduced range of motion. Some people notice warmth around the joint or a catching, locking, or popping sensation when they move. If the tumor is near the surface, especially in localized disease, there may be a visible or palpable lump.
Diffuse disease tends to be sneakier. Instead of a clearly defined mass, it may feel like a joint that is always irritated, always swollen, and always one bad stair climb away from a complaint letter. The knee is especially common in diffuse TGCT, and patients often report recurring swelling and pain that seem out of proportion to any obvious injury.
One important detail is that symptoms may linger for months or even years before a correct diagnosis is made. In patient registry data, many people reported that symptoms started at least a year before diagnosis, and about half reported some form of misdiagnosis before TGCT was finally identified. That delay is not because patients are imagining things. It is because TGCT can impersonate more common joint problems with impressive confidence.
What Causes TGCT?
Researchers do not think TGCT is caused by anything a patient did wrong. It is not the result of eating the wrong snack, stretching too little, or angering the gods of orthopedics. Current evidence points to abnormal cellular signaling, especially involving the colony-stimulating factor 1 pathway, commonly shortened to CSF1. In many TGCTs, a genetic rearrangement leads to overexpression of CSF1, which then attracts inflammatory cells and helps drive tumor growth.
That molecular insight matters because it has reshaped treatment. Instead of viewing TGCT only as a surgical problem, specialists now also think about it as a disease with a targetable signaling pathway. That shift helped lead to newer systemic medications for certain adults with symptomatic disease when surgery is not a good option.
How TGCT Is Diagnosed
Diagnosis usually begins with a physical exam and imaging. X-rays may help show pressure effects on nearby bone, but MRI is often the star of the show because it gives a much better look at soft tissue. In localized TGCT, MRI may show a more defined nodular mass. In diffuse disease, MRI may reveal widespread synovial thickening, extensive mass-like tissue, or joint damage.
Ultrasound can also help in some cases, especially for superficial masses. Joint aspiration may be performed if there is swelling, and biopsy is sometimes needed to confirm the diagnosis. That is especially useful when imaging raises concern for other conditions, including soft tissue tumors that need a different treatment plan.
Because TGCT is rare, many patients are eventually referred to orthopedic oncology, musculoskeletal radiology, or a center familiar with complex joint tumors. That referral can make a huge difference. Rare disease plus common symptoms is a recipe for detours.
Treatment Options for TGCT
Surgery
Surgery remains the main treatment for many patients, especially those with localized TGCT. Depending on the tumor’s size and location, the procedure may be done with open surgery, arthroscopy, or a combination of both. In localized disease, surgery is often curative. In diffuse disease, the goal may be to remove as much diseased tissue as possible while preserving joint function.
That balancing act is tricky. If the tumor wraps around critical structures or coats large areas of synovium, complete removal may be difficult. The more diffuse the disease, the greater the chance that symptoms or tumor growth may return after surgery.
Active Surveillance
Not every patient needs immediate aggressive treatment. In selected cases, especially when symptoms are mild or the risks of intervention are high, specialists may recommend active surveillance. This means close monitoring with follow-up exams and imaging rather than rushing straight into an operation. For the right patient, watching carefully can be smarter than treating quickly.
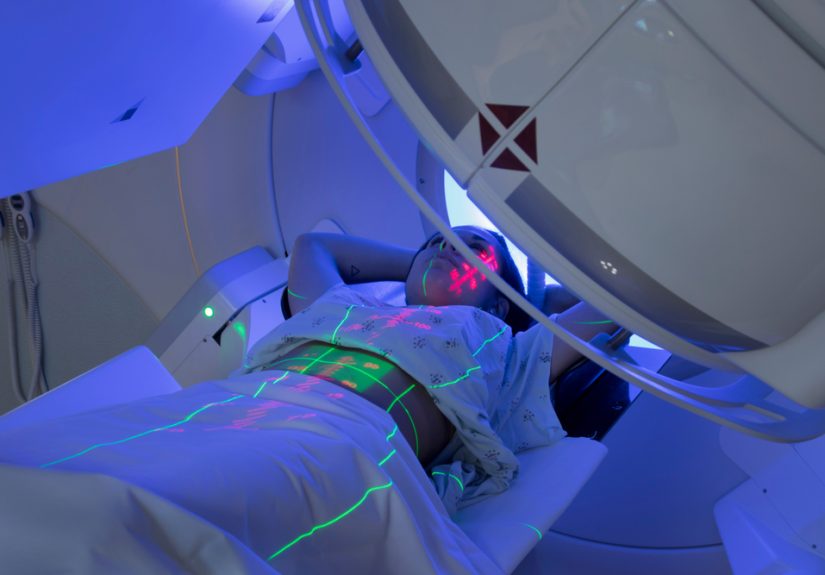
Radiation Therapy
Radiation has been used in some recurrent or difficult diffuse cases, sometimes after surgery, but it is not a routine first-line choice. Some orthopedic sources describe it as an option when standard surgery has not worked or when recurrence risk is especially high. More recent reviews note that many experts use radiation sparingly because of limited evidence and concern about joint complications. In short, it is a tool, but not the favorite tool in the box.
Targeted Drug Therapy
The biggest modern change in TGCT treatment has been targeted therapy aimed at the CSF1 receptor pathway. Pexidartinib became the first FDA-approved systemic treatment for certain adults with symptomatic TGCT not likely to improve with surgery. More recently, vimseltinib also received FDA approval for adults with symptomatic TGCT when surgical resection would likely worsen function or cause severe morbidity.
These drugs are not casual over-the-counter fixes. They are specialist-level treatments used in carefully selected patients, especially those with diffuse, recurrent, or unresectable disease. Pexidartinib, in particular, carries serious liver-related safety concerns and requires monitoring through a restricted risk-management program. Vimseltinib also requires careful monitoring, including liver tests. The takeaway is simple: targeted therapy can be a major advance, but it is not a “pop a pill and forget it” situation.
Recurrence, Recovery, and Long-Term Outlook
The long-term outlook depends heavily on whether the disease is localized or diffuse. Localized TGCT generally has a better prognosis and a lower recurrence burden. Diffuse TGCT is the form that keeps clinicians and patients on their toes. Recurrence after surgery is common enough that follow-up is not optional window dressing. It is a core part of care.
Real-world registry data show just how heavy that burden can be. In one recent observational registry, more than 70% of patients with diffuse TGCT and prior surgery reported at least one recurrence, while recurrence was much lower in localized disease. Other orthopedic sources give somewhat lower surgical recurrence estimates for diffuse PVNS, which reflects how much rates can vary by setting, technique, and patient selection. The broad lesson still stands: diffuse TGCT is the version more likely to come back and keep interrupting life plans.
Recovery also involves more than tumor control. Physical therapy often plays a major role after surgery, especially when stiffness, swelling, or weakness linger. Some patients recover well and move on. Others deal with repeated imaging, repeated procedures, work absences, reduced activity, and the emotional fatigue of wondering whether the joint will flare again.
When to See a Doctor
See a clinician if you have a persistent lump near a tendon or joint, unexplained joint swelling, repeated fluid buildup, ongoing pain, or loss of motion that does not match the usual story of a strain or minor injury. If a joint keeps swelling “for no reason,” or if treatment for more common diagnoses is not helping, it is reasonable to ask whether advanced imaging or referral is needed.
TGCT is rare, but rare does not mean impossible. Sometimes the zebra really is a zebra.
Conclusion
Tenosynovial giant cell tumor is rare, usually benign, and far more disruptive than its noncancer label might suggest. The condition ranges from small localized nodules to diffuse joint disease that can cause pain, stiffness, swelling, repeat surgeries, and long-term functional limits. MRI, biopsy, and specialist evaluation help confirm the diagnosis. Surgery remains central to treatment, but targeted therapies have changed the landscape for selected adults with advanced or hard-to-resect disease.
The most important point is that TGCT is treatable, even when it is frustrating. A good care team, careful imaging, thoughtful treatment selection, and long-term follow-up can make a substantial difference. When a condition is rare, clarity matters. When that condition lives inside a joint, clarity and mobility both matter.
What the TGCT Experience Often Feels Like
Published patient registries and prospective studies show that living with TGCT is often as much a story about delay, uncertainty, and repetition as it is about the tumor itself. Many patients describe a long stretch of feeling that something is wrong before anyone can put the right label on it. A knee swells after activity, then swells again. An ankle becomes stiff for no obvious reason. A hand lump sticks around longer than expected. At first, the symptoms can sound ordinary enough to be dismissed as overuse, tendon irritation, arthritis, or a sports injury. That is one reason so many patients report multiple appointments before reaching the correct diagnosis.
Then comes the imaging phase, which can feel both helpful and surreal. Once MRI enters the picture, patients often move from “maybe it is just inflammation” to “wait, there is an actual mass in there?” That emotional pivot is real. Even when clinicians explain that TGCT is usually benign, the word tumor still lands with force. People hear it and immediately picture worst-case scenarios, future surgeries, or permanent loss of function. The condition may not fit the standard idea of cancer, but it can still disrupt work, sports, caregiving, sleep, and confidence in one’s own body.
For patients with localized TGCT, the experience may center on removal and recovery. There is often relief after surgery, especially if the lesion is well-defined and symptoms improve quickly. For patients with diffuse TGCT, the story is often more complicated. Symptoms may return. Follow-up scans become part of the calendar. Physical therapy sessions stack up. Workouts get modified, then postponed, then replaced by the phrase “I will see how the joint feels tomorrow,” which is not exactly the motivational slogan anyone asked for.
There is also a quality-of-life burden that outsiders may underestimate. Pain is one part of it, but not the whole part. Stiffness, loss of range of motion, recurring swelling, and uncertainty about recurrence can be just as draining. Some patients become very aware of every stair, every squat, every long walk through an airport, every moment their joint decides to be dramatic in public. Others describe frustration with how invisible the condition can look from the outside. A person may appear fine while quietly organizing life around a difficult knee, hip, ankle, or hand.
At the same time, there is a hopeful thread in the TGCT experience. Better imaging, growing awareness, referral to multidisciplinary teams, and targeted therapies have all improved the landscape. Many patients do get meaningful relief. Many return to work, exercise, travel, and daily routines. For others, success looks less like a perfect cure and more like control: fewer flare-ups, better function, smarter treatment timing, and a clearer plan. That may not sound flashy, but in rare joint disease, steady progress is a big deal. Sometimes victory is not a movie ending. Sometimes it is climbing the stairs without negotiating with your knee first.