Table of Contents >> Show >> Hide
- What Is Shingles?
- Can You Get Shingles If You’ve Never Had Chickenpox?
- Chickenpox vs. Shingles: Same Virus, Different Performance
- Who Is Most at Risk for Shingles?
- Symptoms of Shingles to Watch For
- Can Shingles Be Contagious?
- What If You’re Not Sure Whether You Had Chickenpox?
- Chickenpox Vaccine vs. Shingles Vaccine
- How Is Shingles Treated?
- Possible Complications of Shingles
- When Should You Call a Doctor?
- Practical Prevention Tips
- Common Myths About Shingles and Chickenpox
- Real-Life Experiences and Practical Scenarios
- Conclusion
Here is the quick answer, served without medical confetti: usually, you cannot get shingles if you have truly never had chickenpox and have never been infected with the varicella-zoster virus. Shingles is not a brand-new infection that drops in uninvited like a neighbor with a leaf blower. It is the return of a virus already hiding in the body after a past chickenpox infectionor, rarely, after chickenpox vaccination.
But life, viruses, and childhood memories are messy. Many adults say, “I never had chickenpox,” when what they really mean is, “Nobody remembers me looking like a connect-the-dots puzzle.” Mild childhood chickenpox can be forgotten, misdiagnosed, or mistaken for another rash. That is why the real answer to “Can you get shingles if you’ve never had chickenpox?” is: not if you were never exposed to varicella-zoster virus, but plenty of people have been exposed without realizing it.
This guide explains how shingles works, why chickenpox history matters, whether the chickenpox vaccine changes the answer, how shingles spreads, what symptoms to watch for, and when to call a healthcare provider instead of asking the internet to become your dermatologist.
What Is Shingles?
Shingles, also called herpes zoster, is a painful rash caused by the reactivation of the varicella-zoster virus. This is the same virus that causes chickenpox. After a person recovers from chickenpox, the virus does not fully leave the body. Instead, it settles quietly in nerve tissue, behaving like a tiny viral roommate who promised to move out but never signed the paperwork.
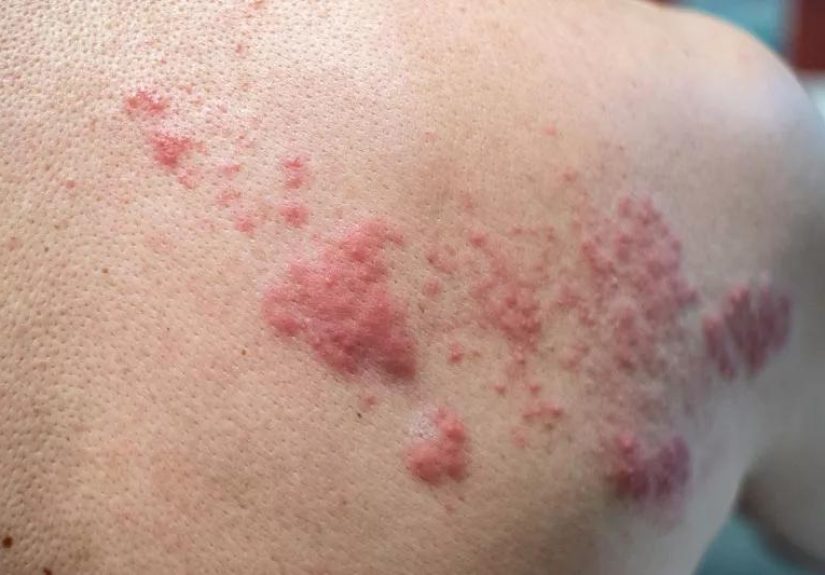
Years or decades later, the virus can wake up and travel along nerve pathways to the skin. That reactivation causes shingles. The rash often appears as a stripe or band on one side of the body, although it can also affect the face, scalp, eye area, or other regions. Common symptoms include burning, tingling, itching, sensitivity, and clusters of fluid-filled blisters.
The most important idea is this: shingles comes from a virus already inside the body. It is not the same as catching chickenpox for the first time.
Can You Get Shingles If You’ve Never Had Chickenpox?
If you have truly never had chickenpox, never received the chickenpox vaccine, and never been infected with varicella-zoster virus, then you would not be expected to develop shingles. The virus needs to be present in your body first before it can reactivate later.
However, there are three big “but wait” situations:
1. You May Have Had Chickenpox Without Knowing It
Some people had very mild chickenpox as children. They may have had only a few spots, a brief fever, or a rash that parents thought was bug bites, heat rash, or “something from daycare.” Childhood medical records can disappear faster than leftover pizza at a sleepover, so many adults are unsure.
In the United States, many people born before widespread chickenpox vaccination were exposed during childhood. That means a person may honestly believe they never had chickenpox while still carrying the virus that can later cause shingles.
2. The Chickenpox Vaccine Can Rarely Lead to Shingles Later
The chickenpox vaccine contains a weakened form of varicella-zoster virus. It is designed to protect against chickenpox, and it has greatly reduced chickenpox illness. In rare cases, the vaccine-strain virus can become latent and reactivate later as shingles. This is uncommon, and vaccinated children generally have a lower risk of shingles than children who had natural chickenpox.
So, if someone says, “I never had chickenpox, but I did get vaccinated,” shingles is still possible, though much less likely than after natural infection.
3. You Can Get Chickenpox From Someone With Shingles
You cannot catch shingles from another person. But if you have never had chickenpox and have never been vaccinated, direct contact with fluid from shingles blisters can transmit varicella-zoster virus and cause chickenpox. Later in life, after that first infection, shingles could become possible.
In plain English: exposure to shingles does not give you shingles today. It may give a non-immune person chickenpox, and shingles could happen years later.
Chickenpox vs. Shingles: Same Virus, Different Performance
Chickenpox and shingles are caused by the same virus, but they behave differently.
Chickenpox Is the First Act
Chickenpox is usually the first infection with varicella-zoster virus. It often causes fever, tiredness, and an itchy rash that spreads across the body. Before vaccination became routine, chickenpox was a common childhood illness in the United States. Many people remember oatmeal baths, calamine lotion, and being told not to scratch while absolutely scratching anyway.
Shingles Is the Comeback Tour
Shingles happens when the old virus reactivates. Instead of a widespread rash, shingles usually appears in a more localized pattern, often on one side of the body. Pain can begin before the rash appears, which makes shingles tricky at first. Some people think they pulled a muscle, developed a mysterious sunburn, or angered their laundry detergent.
The difference matters because someone who never had the first act cannot usually have the comeback tour.
Who Is Most at Risk for Shingles?
Anyone who has had chickenpox can develop shingles, but risk increases with age. Adults over 50 are more likely to get shingles because immune protection naturally weakens over time. People with weakened immune systems also face a higher risk. This includes people receiving certain cancer treatments, transplant medications, long-term high-dose steroids, or other immune-suppressing therapies.
Stress, illness, and major physical strain may also be associated with shingles outbreaks, though the immune system is complicated and does not always send a calendar invite explaining its decisions.
Symptoms of Shingles to Watch For
Shingles can start subtly. Before the rash appears, a person may notice pain, burning, tingling, itching, or unusual skin sensitivity in one area. Then a rash develops, often forming small blisters. The rash may be very painful and commonly appears on one side of the torso, but it can also show up near the eye, ear, face, or scalp.
Common Symptoms
- Burning, stabbing, or tingling pain
- A rash on one side of the body
- Clusters of fluid-filled blisters
- Itching or skin sensitivity
- Fatigue, headache, fever, or chills
- Pain that begins before the rash
If shingles appears near the eye, it should be treated as urgent. Eye involvement can lead to serious complications, including vision problems. Do not wait to see whether it “just chills out.” Viruses are famously bad at taking hints.
Can Shingles Be Contagious?
Shingles itself is not contagious in the way a cold is contagious. You do not inhale shingles from someone’s sneeze and wake up with a stripe of blisters. However, the virus inside shingles blisters can spread to someone who is not immune to chickenpox.
A person with active shingles should keep the rash covered, avoid touching or scratching it, wash hands often, and avoid close contact with people at higher risk until the blisters crust over. This is especially important around newborns, pregnant people without immunity, and people with weakened immune systems.
What If You’re Not Sure Whether You Had Chickenpox?
If you are unsure, you are in a very large club. The membership card is invisible and probably stored with your missing childhood vaccine records.
A healthcare provider can help determine whether you likely have immunity. Evidence may include vaccination records, a provider-confirmed history of chickenpox, a history of shingles, or laboratory evidence of immunity. In some situations, a blood test may be used to check for varicella immunity.
If you do not have evidence of immunity, your provider may recommend the chickenpox vaccine, depending on your age, health status, pregnancy status, and medical history. The chickenpox vaccine is not the same as the shingles vaccine.
Chickenpox Vaccine vs. Shingles Vaccine
These two vaccines often get mixed up, so let’s politely separate them before they start borrowing each other’s sweaters.
Chickenpox Vaccine
The chickenpox vaccine helps prevent primary varicella infection. It is recommended for children and for adolescents and adults who do not have evidence of immunity, as long as there are no medical reasons to avoid it.
Shingles Vaccine
The shingles vaccine, commonly known as Shingrix, is used to help prevent shingles and related complications. In the United States, it is recommended for adults age 50 and older, and for certain adults age 18 and older who are or will be immunocompromised. Shingrix is not used to prevent chickenpox.
If you are an adult who never had chickenpox and never received the chickenpox vaccine, ask a healthcare provider what vaccine plan makes sense for you. Do not guess based on vibes, social media comments, or your uncle’s memory of 1987.
How Is Shingles Treated?
Shingles is usually treated with antiviral medication, especially when caught early. Common antivirals include acyclovir, valacyclovir, and famciclovir. Treatment works best when started within about 72 hours after the rash appears, although a provider may still recommend treatment later in certain cases, especially if new blisters are forming or the rash involves the face or eye.
Pain control is also important. Depending on severity, a healthcare provider may suggest over-the-counter pain relievers, prescription medications, cool compresses, soothing lotions, or other strategies. The goal is to shorten the outbreak, reduce discomfort, and lower the chance of complications.
Possible Complications of Shingles
Most people recover from shingles, but complications can happen. The most common complication is postherpetic neuralgia, a nerve pain that continues after the rash clears. This pain can last weeks, months, or longer and may interfere with sleep, clothing comfort, and daily activities.
Other possible complications include bacterial skin infection, scarring, hearing problems, neurological complications, and eye disease if shingles affects the face or eye area. These risks are why early diagnosis matters. Shingles is not just “a rash with ambition.” It deserves medical attention.
When Should You Call a Doctor?
Contact a healthcare provider promptly if you suspect shingles, especially if the rash is painful, appears near the eye, affects the face, spreads widely, or occurs in someone with a weakened immune system. You should also seek care if you are pregnant, caring for a newborn, or unsure whether you are immune to chickenpox after exposure.
Because antivirals work best early, waiting a week to “see what happens” is not ideal. Shingles has a tiny clock, and it is rude enough to start ticking before you fully understand what is going on.
Practical Prevention Tips
The best prevention depends on your situation. If you never had chickenpox and were never vaccinated, talk to your provider about varicella vaccination. If you are age 50 or older, or immunocompromised and eligible, ask about shingles vaccination. If someone in your home has shingles, avoid direct contact with the rash, keep the rash covered, wash hands frequently, and protect anyone who may be vulnerable.
Good prevention is not dramatic. It is usually boring, consistent, and effectivethe health equivalent of flossing, but with fewer lectures from your dentist.
Common Myths About Shingles and Chickenpox
Myth 1: “You Can Catch Shingles From Someone”
You cannot catch shingles itself. A person with shingles can spread varicella-zoster virus to someone without immunity, but that person would develop chickenpox, not shingles.
Myth 2: “If You Don’t Remember Chickenpox, You’re Safe”
Not necessarily. Many people do not remember childhood infections. A mild case may have gone unnoticed or undocumented.
Myth 3: “Only Older Adults Get Shingles”
Shingles is more common in older adults, but younger people can get it too, especially if their immune system is weakened.
Myth 4: “Shingles Is Just a Skin Problem”
Shingles affects nerves, which is why it can be so painful and why complications like postherpetic neuralgia can continue after the rash disappears.
Real-Life Experiences and Practical Scenarios
People often arrive at the shingles question through ordinary life moments, not medical textbooks. One common scenario is the adult who says, “I never had chickenpox,” then develops a painful band-like rash on the ribs. At first, they blame a tight bra, a scratchy shirt, a gym injury, or sleeping in a position only a pretzel would respect. A day or two later, blisters appear. The doctor diagnoses shingles, and the patient is confused because they were sure chickenpox never happened. In many cases, the likely explanation is a forgotten or very mild childhood infection.
Another experience involves parents. A child gets the chickenpox vaccine, and years later a parent reads that vaccinated people can rarely get shingles. Cue the worried internet search. The helpful perspective is that vaccination generally lowers the risk compared with natural chickenpox. Rare does not mean impossible, but it also does not mean likely. For most families, vaccination is a major protective tool, not a reason to panic every time a child has an itchy spot.
Some adults discover the issue through exposure. A grandparent develops shingles, and a younger family member who never had chickenpox wonders if they should stay away. The answer depends on immunity. If the younger person has had chickenpox or the chickenpox vaccine, the risk is much lower. If they have no immunity, they should avoid direct contact with the rash and talk to a healthcare provider. The grandparent should keep the rash covered and practice careful hand hygiene until the blisters crust over.
Workplaces can create another awkward situation. Imagine an employee with shingles under clothing who feels well enough to work. Coworkers may hear “shingles” and assume the office has become a viral escape room. In reality, shingles does not spread through casual conversation. The main concern is direct contact with blister fluid, especially for people without chickenpox immunity. Clear information prevents unnecessary fearand unnecessary side-eye in the break room.
There is also the experience of delayed treatment. Some people wait because they think the rash is poison ivy, an allergic reaction, or a weird laundry detergent betrayal. By the time they seek care, the pain is intense. This is why awareness matters: a painful, one-sided rash should raise suspicion for shingles. Calling a provider early may help shorten the illness and reduce the chance of lingering nerve pain.
Finally, many people learn about shingles while caring for aging parents. A parent may describe burning pain before a rash appears, and the family may not connect it to shingles right away. Once diagnosed, the conversation often turns to vaccination, immune health, and whether other family members are protected against chickenpox. These moments are stressful, but they can also be useful reminders: old viruses do not retire; they merely wait for poor timing.
The practical takeaway from these experiences is simple. Do not rely only on memory to decide whether shingles is possible. Do not assume every rash is harmless. Do not panic if you are exposed, but do check your immunity status if you are unsure. And if a painful blistering rash appearsespecially on one side of the body or near the faceget medical advice quickly. Your nerves will appreciate the punctuality.
Conclusion
So, can you get shingles if you’ve never had chickenpox? If you truly never had chickenpox, never received the chickenpox vaccine, and were never infected with varicella-zoster virus, shingles would not be expected. But many people are not completely sure about their childhood chickenpox history. A mild or forgotten infection can leave the virus behind, and that virus can reactivate years later as shingles.
The smartest move is not to play detective with blurry childhood memories. If you are unsure whether you had chickenpox, ask a healthcare provider about immunity and vaccination. If you think you have shingles, seek care early, especially if the rash is painful, near the eye, or you have a weakened immune system. Shingles may be an old virus making a dramatic comeback, but with the right information and timely care, you do not have to give it a standing ovation.



