Table of Contents >> Show >> Hide
- What Is Eagle Syndrome?
- Common Eagle Syndrome Symptoms
- What Causes Eagle Syndrome?
- How Eagle Syndrome Is Diagnosed
- Conditions That Can Mimic Eagle Syndrome
- Eagle Syndrome Treatment Options
- Eagle Syndrome Surgery: What to Know
- Questions to Ask Your Doctor
- Living With Eagle Syndrome: Practical Tips
- Experience-Based Insights: What Eagle Syndrome Can Feel Like in Real Life
- Conclusion
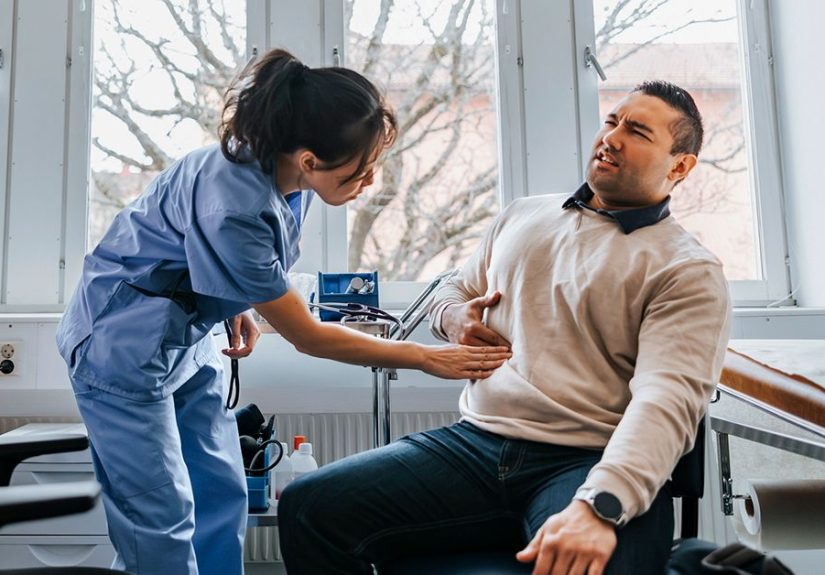
Eagle syndrome sounds like something a patriotic superhero might develop after too many Fourth of July parades. In reality, it is a rare but very real pain condition involving a small, pointed bone near the base of the skull called the styloid process. When this bone becomes unusually long, angled, or associated with a hardened stylohyoid ligament, it can irritate nearby nerves, muscles, blood vessels, and throat structures. The result may be throat pain, ear pain, facial pain, neck discomfort, trouble swallowing, headaches, dizziness, or symptoms that seem to wander around like they forgot to bring a map.
Because Eagle syndrome can mimic dental problems, temporomandibular joint disorder, glossopharyngeal neuralgia, sinus trouble, migraine, throat disease, or even vascular problems, many people spend months or years looking for an explanation. One person may be told it is “just TMJ.” Another may be treated for recurring tonsil pain. Someone else may bounce between dentists, neurologists, and ear, nose, and throat specialists before a CT scan finally points to the culprit.
The good news: Eagle syndrome is diagnosable, and many people improve with the right treatment. Some mild cases respond to medication, injections, physical therapy, or careful symptom management. More severe or persistent cases may need styloidectomy surgery, a procedure that shortens or removes the problematic portion of the styloid process. Let’s walk through what Eagle syndrome is, how it feels, how doctors diagnose it, and what treatment and surgery may involve.
What Is Eagle Syndrome?
Eagle syndrome is a condition in which an elongated styloid process or a calcified stylohyoid ligament causes symptoms by pressing on or irritating nearby tissues. The styloid process is a slender, spike-like bone that projects downward from the temporal bone of the skull, just below the ear. The stylohyoid ligament connects this area to the hyoid bone in the front of the neck.
Normally, this little structure minds its own business. It helps support muscles and ligaments involved in swallowing, speaking, and head movement. But if it becomes too long, too sharply angled, or associated with bony ligament calcification, it may become a tiny anatomical troublemaker. Imagine a coat hook in a hallway: harmless when placed correctly, annoying when it pokes you every time you turn your head.
Classic Eagle Syndrome vs. Vascular Eagle Syndrome
Doctors often describe Eagle syndrome in two broad patterns:
- Classic Eagle syndrome: This usually involves throat, tonsil, ear, jaw, face, or neck pain. Symptoms may worsen when swallowing, chewing, talking, yawning, or turning the head.
- Vascular Eagle syndrome: This occurs when the styloid process or calcified ligament affects nearby blood vessels, especially the carotid artery or jugular vein. Symptoms may include dizziness, fainting, visual changes, headache, transient neurologic symptoms, or, rarely, stroke-like episodes.
Not everyone with an elongated styloid process has Eagle syndrome. Many people have anatomical elongation on imaging but no symptoms at all. The syndrome is diagnosed when the abnormal styloid or ligament matches the person’s symptoms and clinical findings.
Common Eagle Syndrome Symptoms
Eagle syndrome symptoms can be frustrating because they are often one-sided, intermittent, and oddly specific. A person may feel mostly fine until they swallow, turn their head, chew, sing, sneeze, or sleep in the “wrong” position. Then the pain arrives like an uninvited guest with excellent timing and terrible manners.
Throat and Swallowing Symptoms
Many people describe a persistent sensation that something is stuck in the throat. This is sometimes called a foreign body sensation. Others report pain around the tonsil area, pain when swallowing, or discomfort that radiates from the throat to the ear. Some people say it feels like a fish bone, popcorn shell, or small sharp object is lodged in the throat, even though nothing is there.
Possible throat-related symptoms include:
- Throat pain, often on one side
- Pain near the tonsil area
- Difficulty swallowing, also called dysphagia
- Pain with chewing, talking, yawning, or singing
- Feeling of a lump, pressure, or object in the throat
- Voice discomfort or fatigue in some cases
Ear, Jaw, Face, and Neck Pain
Because the styloid process sits close to several nerves and muscles, pain may travel. A person may feel discomfort in the ear, lower jaw, cheek, side of the face, neck, or under the angle of the jaw. The pain can be dull and nagging, sharp and electric, or a strange pressure that is hard to describe without sounding dramatic. Fortunately, dramatic descriptions are welcome in medicine; they often help doctors understand the pattern.
These symptoms may include:
- Ear pain without an ear infection
- Jaw pain that mimics TMJ disorder
- Facial pain or tenderness
- Pain under the jaw or behind the jawbone
- Neck pain that worsens with movement
- Headache, especially near the temple or side of the head
Neurologic and Vascular Symptoms
In vascular Eagle syndrome, the elongated styloid process may irritate or compress nearby arteries or veins. This is less common than classic throat and facial pain, but it can be more serious. Symptoms may be positional, appearing when a person turns, flexes, or extends the neck.
Warning signs may include:
- Dizziness or lightheadedness
- Fainting or near-fainting
- Blurred vision or visual disturbances
- One-sided weakness, numbness, or facial drooping
- Speech changes
- Severe sudden headache
- Stroke-like symptoms that come and go
Any stroke-like symptom should be treated as an emergency. Even if symptoms disappear, urgent medical evaluation is important because transient ischemic attacks and vascular compression need careful assessment.
What Causes Eagle Syndrome?
Eagle syndrome is linked to an elongated styloid process, a calcified stylohyoid ligament, or an abnormal angle of the styloid process. Why this happens is not always clear. Several theories exist, and more than one factor may be involved.
Possible Contributing Factors
- Natural anatomical variation: Some people are simply born with longer styloid processes.
- Ligament calcification: The stylohyoid ligament may harden or partially turn into bone over time.
- Prior tonsillectomy: Eagle syndrome was historically described in some people after tonsil removal, possibly due to scar tissue or altered local anatomy.
- Trauma or neck injury: Injury may irritate tissues or make a previously silent anatomical feature symptomatic.
- Aging-related changes: Ligaments may lose flexibility or calcify with age.
- Mechanical irritation: Repeated movement, posture, or local inflammation may contribute to symptoms in susceptible people.
It is important to avoid oversimplifying the condition. Having a long styloid process does not automatically mean a person has Eagle syndrome. The key question is whether the anatomy matches the symptoms.
How Eagle Syndrome Is Diagnosed
Diagnosis usually requires a combination of medical history, physical examination, imaging, and careful exclusion of other conditions. Because Eagle syndrome can imitate several more common disorders, the process may take time.
Medical History and Symptom Pattern
A clinician may ask when the pain started, whether it is one-sided, what triggers it, and where it travels. Details matter. Pain that worsens with swallowing, chewing, yawning, or head rotation may raise suspicion. So may a history of unexplained throat pain, ear pain without infection, or symptoms that have not responded to dental or TMJ treatment.
Physical Examination
In some cases, a doctor may gently palpate the tonsillar area inside the mouth or examine the side of the neck. If touching the tonsillar fossa reproduces the familiar pain, Eagle syndrome becomes more likely. However, not everyone has a styloid process that can be felt, and a normal-feeling exam does not rule it out.
Imaging Tests
Imaging is central to diagnosis. A standard X-ray may show styloid elongation, but computed tomography, especially a CT scan with 3D reconstruction, is often more useful because it can show length, angle, side-to-side differences, and relationship to nearby structures.
Common imaging options include:
- CT scan: Helps visualize the styloid process and calcified stylohyoid ligament.
- 3D CT reconstruction: Gives a clearer view of the bone’s length and direction.
- CT angiography: Used when vascular compression is suspected.
- MRI or MR angiography: May be considered when nerve, soft tissue, or vascular concerns need further evaluation.
Conditions That Can Mimic Eagle Syndrome
Eagle syndrome is a master of disguise. Before confirming the diagnosis, clinicians may consider other causes of head, neck, facial, and throat pain.
- Temporomandibular joint disorder
- Dental infection or impacted wisdom teeth
- Glossopharyngeal neuralgia
- Trigeminal neuralgia
- Chronic tonsillitis or throat inflammation
- Sinus disease
- Cervical spine arthritis or disc disease
- Migraine or cluster headache
- Carotid artery dissection or vascular disease
- Head and neck tumors
This is why self-diagnosis is risky. The internet is useful for learning, but it is not a substitute for a trained clinician with imaging, a physical exam, and the ability to rule out more dangerous problems.
Eagle Syndrome Treatment Options
Treatment depends on symptom severity, anatomy, vascular involvement, overall health, and the person’s goals. Mild symptoms may be treated conservatively. Persistent, severe, or vascular cases may require surgery.
Conservative Treatment
Conservative care does not remove the elongated styloid process, but it may reduce irritation and pain. This approach may be reasonable when symptoms are mild, diagnosis is still being confirmed, or surgery is not immediately appropriate.
Non-surgical options may include:
- Over-the-counter or prescription pain relievers
- Anti-inflammatory medications when appropriate
- Nerve pain medications such as gabapentin or similar drugs, when prescribed
- Local anesthetic or steroid injections
- Physical therapy focused on gentle neck mechanics
- Posture support and avoidance of triggering neck positions
- Diet changes during flares, such as softer foods if swallowing is painful
Conservative treatment can be helpful, but it may not solve the structural cause. Think of it as turning down the volume on a noisy radio, not necessarily removing the radio from the room.
When Surgery May Be Recommended
Surgery may be considered when symptoms are severe, persistent, clearly linked to the styloid process, or associated with vascular compression. The operation is called a styloidectomy. Its goal is to shorten or remove the problematic portion of the styloid process or calcified ligament so it no longer irritates nearby structures.
Surgery is not automatically recommended for every elongated styloid process. A careful evaluation is important because operating on an incidental finding may not improve unrelated symptoms. The best surgical candidates are typically those whose symptoms, exam, and imaging all point in the same direction.
Eagle Syndrome Surgery: What to Know
Styloidectomy can be performed through different approaches. The two most commonly discussed are the transoral approach and the transcervical, or external neck, approach. Each has benefits and trade-offs.
Transoral Styloidectomy
In a transoral approach, the surgeon reaches the styloid process through the mouth, often near the tonsillar area. This can avoid an external neck scar and may involve a shorter visible recovery. However, the surgical field is smaller, access may be more limited, and infection risk may be a consideration because the mouth naturally contains bacteria.
Transcervical Styloidectomy
In a transcervical approach, the surgeon makes an incision in the neck to access the styloid process externally. This may provide better visibility of nerves, blood vessels, and surrounding structures, which can be especially important in complex or vascular cases. The trade-off is an external incision and scar, although many neck scars fade significantly with time.
Possible Benefits of Surgery
Many published reports and clinical experiences describe meaningful symptom improvement after styloidectomy in carefully selected patients. Benefits may include reduced throat pain, less ear and jaw pain, improved swallowing comfort, fewer positional symptoms, and better quality of life.
Possible Risks and Recovery
Like all surgery, styloidectomy has risks. These may include bleeding, infection, nerve irritation, swallowing discomfort, temporary numbness, scar sensitivity, first-bite pain, persistent symptoms, or recurrence if a remaining portion continues to irritate tissue. Vascular cases require particularly careful planning.
Recovery varies. Some people notice improvement quickly, while others heal gradually over weeks or months as inflammation settles and irritated nerves calm down. A realistic recovery plan may include soft foods, pain control, wound care, activity restrictions, and follow-up visits.
Questions to Ask Your Doctor
If Eagle syndrome is suspected, bring organized questions to your appointment. A rare condition can make appointments feel like speed dating with medical jargon, so a written list helps.
- Does my imaging show an elongated styloid process, calcified ligament, or abnormal angle?
- Do my symptoms match the side and location of the imaging finding?
- Could my symptoms be caused by TMJ disorder, neuralgia, dental disease, migraine, or cervical spine problems?
- Do I need CT angiography to evaluate blood vessel compression?
- Should I see an ENT, head-and-neck surgeon, neurologist, vascular surgeon, or pain specialist?
- Am I a candidate for conservative treatment, surgery, or both?
- Which surgical approach do you recommend and why?
- How many Eagle syndrome cases have you treated?
- What are the expected benefits, risks, and recovery timeline?
Living With Eagle Syndrome: Practical Tips
While waiting for diagnosis or treatment, symptom tracking can make a major difference. Write down pain location, triggers, duration, head position, swallowing difficulty, dizziness, and any neurologic symptoms. Bring this record to appointments. Doctors love clear patterns almost as much as coffee and functioning printers.
Some people find it helpful to avoid extreme neck rotation, sleep with supportive pillows, eat softer foods during flares, pause long phone calls, and limit activities that trigger throat or jaw pain. Stress management may not cure Eagle syndrome, but pain and stress are excellent at making each other louder. Gentle relaxation, paced breathing, and good sleep habits can support the nervous system while medical evaluation continues.
Experience-Based Insights: What Eagle Syndrome Can Feel Like in Real Life
Eagle syndrome is not just a diagnosis on a scan. For many people, it is a confusing lived experience. The pain may start quietly: a strange poke in the throat, a recurring earache, a tight feeling under the jaw. At first, it may seem like a dental issue or a stubborn sore throat. Then the symptoms keep returning, even when antibiotics, dental checks, mouthguards, or sinus treatments do not fully explain the problem.
A typical experience might look like this: someone feels sharp pain near one tonsil whenever they swallow. The pain shoots toward the ear, then fades. A few days later, turning the head while driving triggers a jolt along the jaw. The person visits a dentist, who finds nothing alarming. They try a night guard for suspected TMJ. It helps the jaw tension a little, but the throat pain stays. Next comes an ENT visit, perhaps a scope exam, maybe a normal-looking throat, and the phrase every patient both likes and hates: “Everything looks fine.”
The emotional side can be just as challenging as the physical pain. Rare conditions often make people feel like they are overexplaining. They may worry that friends, family, or clinicians think the symptoms are exaggerated. But Eagle syndrome symptoms can be real even when the throat looks normal. The problem may be deeper, near the skull base, nerves, and blood vesselsnot sitting politely on the surface waving a tiny flag.
Another common experience is symptom inconsistency. A person may have a good morning, then pain after lunch because chewing triggered it. They may feel fine while sitting upright, then dizzy when bending the neck. They may have ear pain without ear disease, tooth pain without a bad tooth, or neck pain that physical therapy only partly improves. This inconsistency can make Eagle syndrome difficult to explain in a short appointment.
For people considering surgery, the decision can be emotionally loaded. On one hand, there may be hope: finally, a structural explanation and a possible fix. On the other hand, surgery near the throat, nerves, and blood vessels sounds intimidating. Patients often want to know whether others improved, how painful recovery was, whether swallowing became easier, and whether the scar is noticeable. These are practical questions, not vanity questions. Quality of life matters.
Recovery experiences also vary. Some people report early relief, especially if a clear mechanical trigger was removed. Others experience swelling, nerve sensitivity, first-bite discomfort, or gradual changes over months. Healing is not always a straight line. A good day followed by a flare does not automatically mean surgery failed. Nerves can be dramatic during recovery; they are the divas of the anatomy world.
The most useful experience-based advice is simple: build a team, keep records, and seek clinicians familiar with the condition. Bring imaging discs or digital files, not just reports. Ask whether the styloid length, angle, and relationship to vessels were evaluated. If symptoms are positional or neurologic, ask about vascular imaging. If one specialist dismisses the possibility but symptoms strongly match, a second opinion from an experienced ENT or head-and-neck surgeon may be worthwhile.
Living with Eagle syndrome can be exhausting, but getting the right diagnosis can turn confusion into a plan. The goal is not to chase a rare label for the sake of it. The goal is to connect symptoms, anatomy, and treatment in a way that actually improves daily life.
Conclusion
Eagle syndrome is rare, but for people who have it, the symptoms can be anything but small. An elongated styloid process or calcified stylohyoid ligament can cause throat pain, ear pain, facial pain, jaw discomfort, swallowing problems, headaches, neck pain, and, in vascular cases, dizziness or neurologic warning signs. Because the symptoms overlap with many common conditions, diagnosis often requires persistence, detailed history, physical examination, and the right imagingespecially CT or CT angiography when vascular involvement is suspected.
Treatment ranges from conservative pain management to styloidectomy surgery. The best approach depends on symptom severity, imaging findings, vascular risk, and whether the anatomy truly explains the symptoms. If Eagle syndrome is suspected, the smartest move is to work with clinicians who understand head and neck anatomy and can separate “interesting scan finding” from “actual source of pain.” In other words, do not let a tiny bone boss your whole life around without a proper investigation.