Table of Contents >> Show >> Hide
- What Is Pemphigus Foliaceus?
- Pemphigus Foliaceus Symptoms
- What Causes Pemphigus Foliaceus?
- Is Pemphigus Foliaceus Contagious?
- How Pemphigus Foliaceus Is Diagnosed
- Pemphigus Foliaceus Treatment Options
- Living With Pemphigus Foliaceus
- When to See a Doctor
- Pemphigus Foliaceus vs. Pemphigus Vulgaris
- Can Pemphigus Foliaceus Be Cured?
- Practical Experience: What Managing Pemphigus Foliaceus Can Feel Like
- Conclusion
Note: This article is for general educational purposes and is based on current dermatology and medical references. It is not a substitute for diagnosis, treatment, or personalized medical advice from a licensed healthcare professional.
Pemphigus foliaceus is one of those medical terms that sounds like it belongs in a wizard spellbook, but it is actually a real autoimmune skin disease. It causes fragile blisters, crusted sores, scaling, itching, and inflammationmost often on the face, scalp, chest, upper back, and other sun-exposed areas. The good news? While pemphigus foliaceus can be uncomfortable, stubborn, and emotionally exhausting, it is usually more superficial than pemphigus vulgaris and does not commonly affect the mouth or deeper mucous membranes.
Still, “more superficial” does not mean “ignore it and hope your skin politely sorts itself out.” Pemphigus foliaceus needs proper diagnosis and treatment from a dermatologist because the condition can spread, become painful, increase infection risk, and affect daily life. With the right care plan, many people can control flares, protect their skin barrier, and reduce the need for long-term high-dose medication.
What Is Pemphigus Foliaceus?
Pemphigus foliaceus is a rare autoimmune blistering disorder. In plain English, the immune system mistakenly attacks proteins that help skin cells stick together. When those connections weaken, the top layers of the skin separate, creating shallow blisters and erosions. These blisters are often so delicate that they break before a person even notices them. What remains may look like red, crusty, scaly, or flaky patches.
The main protein involved in pemphigus foliaceus is desmoglein 1, which acts like a tiny piece of biological Velcro between skin cells. When antibodies target desmoglein 1, the upper epidermis becomes fragile. Because desmoglein 1 is especially important in the outer skin and less dominant in many mucous membranes, pemphigus foliaceus usually affects the skin rather than the inside of the mouth.
This condition is not contagious. You cannot catch it from touching someone’s skin, sharing a towel, sitting next to them, or borrowing their hoodie. Pemphigus foliaceus is caused by immune system activity, not germs jumping from person to person like tiny villains in a soap commercial.
Pemphigus Foliaceus Symptoms
The symptoms of pemphigus foliaceus can vary from mild patches to widespread skin involvement. Some people notice a few crusty spots that come and go. Others develop larger areas of redness, scaling, and open erosions that require stronger treatment.
Common Signs and Symptoms
Typical pemphigus foliaceus symptoms include:
- Fragile, shallow blisters that rupture easily
- Crusted sores or scaly patches
- Red, inflamed, or irritated skin
- Itching, burning, tenderness, or pain
- Flaking that may resemble severe dandruff when the scalp is affected
- Skin that peels or breaks down with minor rubbing
- Lesions on the face, scalp, chest, shoulders, and upper back
- Occasional spread to larger areas of the body
Because the blisters are so thin and easy to break, many people never see a classic “bubble-like” blister. Instead, they notice crusts, raw patches, or areas that look like eczema, seborrheic dermatitis, psoriasis, impetigo, or an allergic rash. This is one reason diagnosis can sometimes take time.
Where Does Pemphigus Foliaceus Usually Appear?
Pemphigus foliaceus most commonly affects areas rich in sebaceous glands or exposed to sunlight. These include the scalp, forehead, cheeks, nose, upper chest, upper back, and shoulders. The scalp may develop greasy-looking crusts and flakes, which can be mistaken for stubborn dandruff. On the face, lesions may look like scaly red patches that refuse to behave no matter how many gentle cleansers or moisturizers you try.
Unlike pemphigus vulgaris, pemphigus foliaceus usually does not cause painful mouth ulcers. If mouth, throat, eye, or genital sores appear, a dermatologist may evaluate for another form of pemphigus or a different blistering disease.
What Causes Pemphigus Foliaceus?
Pemphigus foliaceus happens when the immune system produces antibodies that attack desmoglein 1. The exact reason this immune confusion starts is not always clear. Like many autoimmune diseases, pemphigus foliaceus may involve a mix of genetic susceptibility, environmental triggers, medications, infections, ultraviolet exposure, and immune system changes.
Autoimmune Activity
The core cause is autoimmune activity. The immune system is supposed to defend the body from harmful invaders. In pemphigus foliaceus, it accidentally targets a normal skin protein. Think of it like your home security system mistaking your couch for a burglar. The alarm is real, but the target is wrong.
Possible Triggers
Potential triggers may include certain medications, intense sun exposure, infections, stress on the immune system, and genetic background. Some cases have been associated with drugs such as penicillamine, certain blood pressure medications, and other immune-modifying agents, though not everyone with pemphigus foliaceus has a clear medication trigger.
There is also an endemic form called fogo selvagem, historically described in parts of Brazil and associated with environmental and immune factors. Most cases in the United States are sporadic, meaning they occur without a clear geographic cluster.
Is Pemphigus Foliaceus Contagious?
No. Pemphigus foliaceus is not contagious. It is not caused by poor hygiene, and it is not spread by skin contact. Because the lesions can become crusted or raw, people may worry that the condition is infectious. However, the underlying disease is autoimmune. That said, open skin can become secondarily infected with bacteria, so proper wound care is important.
How Pemphigus Foliaceus Is Diagnosed
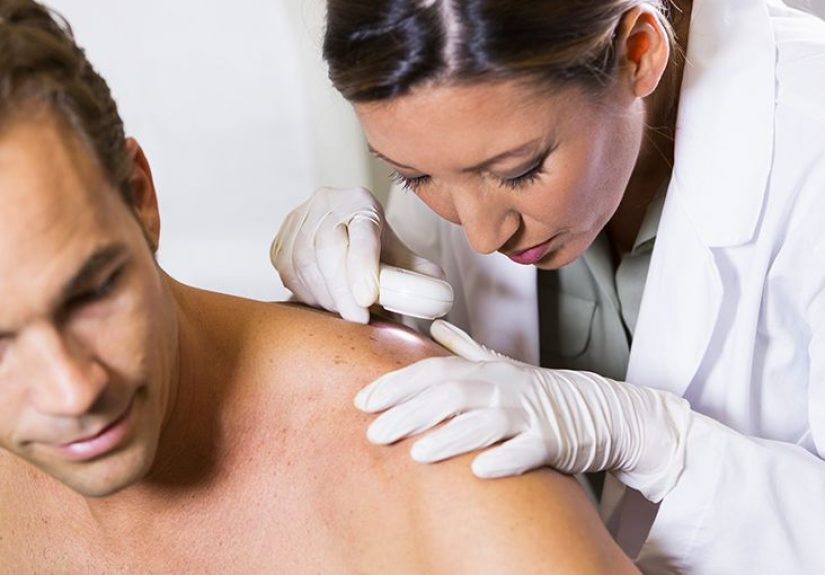
A dermatologist usually diagnoses pemphigus foliaceus using a combination of skin examination, medical history, biopsy, and immune testing. Because the rash can mimic several common skin conditions, testing is important before starting long-term treatment.
Skin Exam and Medical History
The doctor may ask when symptoms began, where they started, whether the rash itches or burns, which medications you take, and whether sun exposure seems to worsen the condition. They may gently examine the skin for fragility, crusting, and the pattern of lesions.
Skin Biopsy
A skin biopsy is one of the most important diagnostic tools. A small sample of affected skin is removed and examined under a microscope. In pemphigus foliaceus, the blistering typically occurs high in the epidermis, the outer layer of the skin.
Direct Immunofluorescence
Direct immunofluorescence testing checks for antibody deposits in the skin. A sample is usually taken from skin near a fresh lesion. This test helps distinguish pemphigus foliaceus from other blistering diseases, such as bullous pemphigoid, dermatitis herpetiformis, and pemphigus vulgaris.
Blood Tests
Blood tests may look for circulating antibodies against desmoglein 1. These tests can support the diagnosis and sometimes help monitor disease activity over time. Doctors may also order general blood work before treatment, especially if systemic medications are being considered.
Pemphigus Foliaceus Treatment Options
Treatment depends on severity, how much skin is involved, the person’s overall health, and how the disease responds over time. The goals are to stop new blisters, heal existing erosions, prevent infection, reduce itching and pain, and use the lowest effective dose of medication.
Topical Corticosteroids
For mild or localized pemphigus foliaceus, high-potency topical corticosteroids may be enough. These creams or ointments reduce inflammation and immune activity in the skin. They are often applied directly to affected areas under a dermatologist’s instructions.
Topical steroids can be very helpful, but they should be used correctly. Overuse can thin the skin, especially on delicate areas like the face. This is one reason treatment should be supervised rather than improvised like a kitchen recipe.
Oral Corticosteroids
Moderate to severe disease may require oral corticosteroids such as prednisone. These medications can quickly reduce inflammation and help control blister formation. However, long-term high-dose steroid use can cause side effects, including weight gain, high blood sugar, bone thinning, mood changes, high blood pressure, and increased infection risk.
Because of these risks, doctors often try to taper steroids once the disease is controlled and may add steroid-sparing medications.
Steroid-Sparing Immunosuppressants
Medications such as azathioprine, mycophenolate mofetil, methotrexate, or other immune-modifying drugs may be used to reduce reliance on corticosteroids. These medicines work more slowly than steroids but can help maintain disease control. Regular blood tests are usually needed to monitor safety.
Rituximab and Biologic Therapy
Rituximab, a monoclonal antibody that targets certain immune cells, has become an important treatment option for pemphigus diseases. It may be considered for more severe, persistent, or relapsing cases. It is not a casual medication, and doctors evaluate infection risk, vaccination status, and overall health before use.
Antibiotics and Infection Care
Antibiotics do not treat the autoimmune cause of pemphigus foliaceus, but they may be needed if open skin becomes infected. Signs of infection can include increasing pain, warmth, swelling, pus, fever, or rapidly worsening redness. Some treatment plans may also include anti-inflammatory antibiotics in selected cases.
Wound Care and Skin Protection
Gentle wound care is a major part of treatment. This may include mild cleansers, nonstick dressings, petroleum-based ointments, and avoiding harsh scrubbing. The skin barrier is already under stress, so aggressive exfoliation is not the moment to audition for a skincare influencer award.
Living With Pemphigus Foliaceus
Living with pemphigus foliaceus can be frustrating because the condition may flare, improve, and flare again. Some people feel self-conscious about visible lesions on the face or scalp. Others feel tired from itching, discomfort, medication schedules, and doctor visits.
Daily Skin Care Tips
A gentle daily routine can help reduce irritation. Use fragrance-free cleansers, avoid hot showers, pat skin dry instead of rubbing, and apply moisturizer as recommended. Choose soft clothing and avoid rough fabrics that may irritate fragile skin. For scalp involvement, medicated shampoos may be recommended, but harsh scrubbing should be avoided.
Sun Protection
Sun exposure may worsen pemphigus foliaceus in some people. Daily sun protection can be helpful, especially for lesions on the face, scalp, chest, and shoulders. Broad-spectrum sunscreen, wide-brimmed hats, protective clothing, and shade are practical tools. Your skin is already dealing with enough drama; ultraviolet rays do not need a guest role.
Medication Safety
People taking immunosuppressive medications should follow their doctor’s monitoring plan. This may include blood tests, infection precautions, bone health support, vaccination planning, and regular checkups. Never stop prescribed treatment suddenly without medical guidance, especially corticosteroids, because abrupt changes can cause serious problems.
When to See a Doctor
You should see a dermatologist if you develop unexplained blisters, crusted sores that do not heal, widespread scaling, painful erosions, or a rash that keeps returning despite basic care. Seek urgent medical attention if you have fever, rapidly spreading redness, severe pain, signs of infection, dehydration, or extensive skin peeling.
Early diagnosis matters. The sooner pemphigus foliaceus is identified, the sooner treatment can beginand the less time you spend wondering why your skin has apparently launched a tiny rebellion.
Pemphigus Foliaceus vs. Pemphigus Vulgaris
Pemphigus foliaceus and pemphigus vulgaris are related autoimmune blistering disorders, but they behave differently. Pemphigus vulgaris often affects the mouth and deeper mucous membranes and can cause more severe erosions. Pemphigus foliaceus usually affects the upper layers of the skin and rarely involves the mouth.
Both conditions require medical care, but the location and depth of blistering help guide diagnosis and treatment. This distinction is one reason biopsy and immune testing are so valuable.
Can Pemphigus Foliaceus Be Cured?
There is no simple overnight cure for pemphigus foliaceus, but many people can achieve good control or remission with treatment. Remission means symptoms are quiet and new blisters are not forming. Some people need long-term maintenance therapy, while others may taper medication after the disease becomes stable.
The outlook depends on disease severity, response to treatment, medication side effects, infection prevention, and ongoing follow-up. Modern therapy has greatly improved quality of life for people with pemphigus diseases.
Practical Experience: What Managing Pemphigus Foliaceus Can Feel Like
For many people, the hardest part of pemphigus foliaceus is not only the rash itselfit is the uncertainty. At first, the symptoms may look like dandruff, eczema, a stubborn allergic reaction, or a skin infection. Someone might try a new shampoo, switch moisturizers, stop wearing makeup, change laundry detergent, and still watch the crusted patches return like an unwanted subscription service.
A common experience is the “why won’t this heal?” stage. A spot on the scalp flakes and crusts. A patch near the nose becomes red and tender. A sore on the chest improves, then reappears after sun exposure or stress. Because the blisters rupture quickly, the person may never see obvious fluid-filled bumps. Instead, they see raw skin, scaling, and irritation. This can delay diagnosis, especially when symptoms are mild at first.
Once a dermatologist suspects pemphigus foliaceus, the biopsy process can feel both intimidating and relieving. Nobody cheers for a skin biopsy like it is a birthday cupcake, but getting a clear diagnosis often brings peace of mind. Finally, there is a name for the problem. More importantly, there is a treatment plan.
Daily life with pemphigus foliaceus often becomes a balancing act. People learn which products are too harsh, which fabrics rub the wrong way, and how much sun exposure their skin can tolerate. A gentle cleanser may replace a strong exfoliating wash. A wide-brimmed hat may become less of a fashion choice and more of a loyal bodyguard. The medicine cabinet may start looking like it has its own ZIP code, but each item has a purpose.
Treatment can also require patience. Topical medications may take time. Oral steroids may work quickly but come with side effects. Immunosuppressive medicines may require regular lab monitoring. Some days, the skin looks calmer; other days, a new patch appears and tests everyone’s emotional flexibility. That up-and-down pattern can be discouraging, so it helps to track symptoms, take photos for doctor visits, and celebrate small winsless itching, fewer crusts, better sleep, or a lower medication dose.
Emotionally, visible skin disease can be surprisingly heavy. Lesions on the face or scalp can make people feel self-conscious in public, at work, or in social situations. Friends may ask, “What happened to your skin?” even when they mean well. A simple, prepared response can help: “It’s an autoimmune skin condition. It’s not contagious, and I’m treating it with my dermatologist.” That sentence can save energy and reduce awkward explanations.
Support matters. A good dermatologist, clear instructions, realistic expectations, and careful follow-up can make the condition feel more manageable. Family members can help by understanding that pemphigus foliaceus is not “just dry skin.” It is an immune-driven disease that needs medical attention, gentle care, and patience.
Over time, many people become experts in their own triggers and routines. They know when to call the doctor, when to protect their skin, when to avoid certain products, and when a flare may be starting. Pemphigus foliaceus may be rare, but people living with it are not powerless. With the right information and treatment, the skin can become calmer, life can feel more predictable, and the mirror can stop feeling like a daily mystery novel.
Conclusion
Pemphigus foliaceus is a rare autoimmune blistering disease that affects the upper layers of the skin. It can cause fragile blisters, crusted sores, scaling, itching, burning, and visible inflammation, especially on the scalp, face, chest, and upper back. Although it is usually less likely than pemphigus vulgaris to affect the mouth, it still deserves serious attention.
Diagnosis often requires a skin biopsy and immune testing, while treatment may include topical corticosteroids, oral steroids, immunosuppressive medications, biologic therapy, wound care, and sun protection. The best results usually come from early diagnosis, consistent follow-up, and a treatment plan tailored to disease severity.
If you suspect pemphigus foliaceus, do not try to solve it with random creams, internet guesses, or heroic amounts of coconut oil. See a dermatologist, get the right tests, and build a plan that protects both your skin and your quality of life.