Table of Contents >> Show >> Hide
- What is a PET scan, exactly?
- Why doctors order PET scans for breast cancer
- How to prepare for a breast cancer PET scan
- What happens during the appointment
- What a PET scan feels like for most people
- What the scan can and cannot tell you
- Risks and side effects
- How results are read and what happens next
- Questions to ask your doctor before the scan
- Bottom line
- Experiences related to breast cancer PET scans: the human side nobody puts on the appointment card
- SEO Tags
Few medical appointments can make time move slower than a breast cancer scan. Five minutes feels like five business days, your phone suddenly becomes your emotional support device, and even the waiting room clock seems dramatic. If your doctor has ordered a PET scan, it helps to know what the test is for, what actually happens during the appointment, and what the results can and cannot tell you.
A PET scan can be a useful tool in breast cancer care, but it is not the star of every scene. It is not usually the first imaging test used to find a new breast cancer, and it is not routinely ordered for every person with early-stage disease. Instead, it is often used when doctors need a clearer picture of whether cancer has spread, come back, or is responding to treatment. In other words, a PET scan is less “routine errand” and more “specialist detective with expensive equipment.”
This guide walks you through what to expect before, during, and after a breast cancer PET scan in plain English, without the medical fog machine.
What is a PET scan, exactly?
PET stands for positron emission tomography. The test uses a tiny amount of radioactive tracer to show how tissues in the body are functioning. In breast cancer, the most common tracer is FDG, a radioactive form of sugar. Because many cancer cells use more glucose than normal cells, areas of concern can appear brighter on the scan.
Most breast cancer PET exams are actually PET/CT scans. That combination matters. The PET portion shows metabolic activity, while the CT portion helps pinpoint where that activity is happening in the body. Think of PET as the “something is happening here” map and CT as the “here is the exact address” map.
There is also a newer type called FES PET, which is used in certain cases of recurrent or metastatic estrogen receptor-positive breast cancer. Instead of tracking sugar use, it helps show estrogen receptor-positive lesions. This can be especially helpful when your oncology team is trying to answer a more targeted question about hormone-sensitive disease.
Why doctors order PET scans for breast cancer
It is usually not a screening test
One of the biggest misunderstandings about PET scans is that “more advanced” automatically means “better for everything.” Not quite. PET scans are not typically used to screen for a brand-new breast cancer, especially a very small one. Mammograms, ultrasound, MRI, and biopsy still do most of the heavy lifting there.
When a PET scan may be helpful
Your doctor may order a breast cancer PET scan to:
- check whether cancer may have spread beyond the breast and nearby lymph nodes
- look for signs that breast cancer has returned after treatment
- evaluate how well treatment is working
- clarify uncertain findings from other imaging tests
- help assess metastatic breast cancer over time
That is why PET scans are more common in people with suspected recurrence, locally advanced disease, or metastatic breast cancer than in someone with a small, newly diagnosed, low-risk tumor.
How to prepare for a breast cancer PET scan
Follow your imaging center’s instructions
Every facility has its own protocol, and your care team’s directions beat the internet every single time. Still, there are a few common themes most patients can expect.
Food, exercise, and timing
Many patients are asked to fast for about 4 to 6 hours before the scan. Water is often allowed, and staying hydrated may be encouraged. You may also be told to avoid strenuous exercise the day before or for a couple of days before the test. That is because hard exercise can affect how muscles use glucose, which can make the scan harder to interpret.
This is not the day for a heroic spin class, a surprise boot camp session, or finally proving you can do burpees with excellent form. Your scan does not care.
Diabetes, pregnancy, and breastfeeding
If you have diabetes, tell your care team ahead of time. Blood sugar levels can affect the scan, and you may get special instructions about insulin, diabetes medications, and meal timing.
You should also tell the team if you are pregnant, think you might be pregnant, or are breastfeeding. PET scans involve radiation exposure, so these details are not paperwork fluff. They matter.
Medications and hormone therapy
Bring a list of your medications. In certain cases, especially with FES PET scans, hormone-related medications may matter because they can affect how the tracer works. Your doctor will tell you whether anything needs to be adjusted before the test.
What happens during the appointment
Step 1: Check-in and prep
When you arrive, the staff will review your information, confirm your medical history, and explain the process. In some centers, your blood sugar may be checked first, especially if the exam uses FDG.
Step 2: The tracer injection
You will receive the tracer through an IV, usually in your arm. The injection itself is generally quick. Most people feel little more than a standard needle stick. Serious reactions are uncommon.
Step 3: The waiting period
After the tracer is injected, you usually wait quietly while it circulates through your body and is absorbed by tissues. This often takes around 30 to 60 minutes. The “quietly” part is important. Many centers will ask you to rest, avoid a lot of movement, and keep talking to a minimum during this period.
It is not personal. They are not trying to create a spa of silence. They are trying to improve image quality.
Step 4: The scan itself
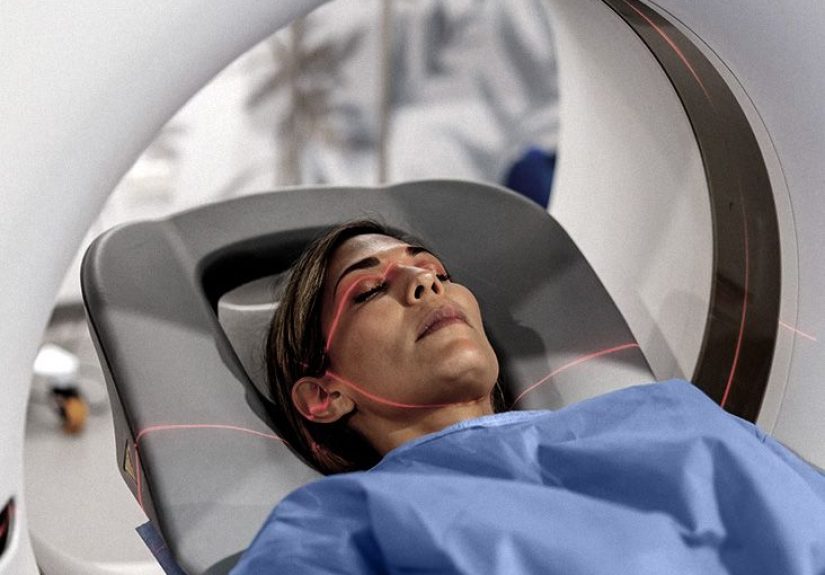
Then you lie on a table that moves through the scanner. The machine is often described as donut-shaped rather than tunnel-shaped, which is mildly comforting and also slightly unfair to donuts. The scan is painless, but you will need to stay still.
The imaging portion often takes around 20 to 30 minutes, though the full appointment is longer because of the prep and waiting time. Some people find the hardest part is not pain but stillness. If you are uncomfortable lying flat or have anxiety in scanners, tell the staff before the test. They deal with this all the time.
What a PET scan feels like for most people
Physically, many patients say a PET scan is easier than they feared. It does not usually hurt beyond the IV placement. The bigger challenge is often emotional. You may feel nervous before the test, impatient during the waiting period, or mentally exhausted by the time it is done.
Some people also feel awkward about the strange combination of high-tech medicine and total stillness. You are lying there, trying not to move, while your brain decides this is the perfect time to remember every unfinished task from the last three years. That is normal. Very annoying, but normal.
What the scan can and cannot tell you
What PET scans do well
PET scans are good at showing areas of abnormal metabolic activity and can help identify whether disease may be present outside the breast. In metastatic or recurrent breast cancer, this information can help guide treatment decisions and monitor response over time.
Where PET scans have limits
PET scans are not perfect. Not every cancer shows up clearly. Very small cancers can be missed. Some breast tumors are less visible on PET than others. At the same time, not every bright area means cancer. Infection, inflammation, healing tissue, and some normal organs can also look bright.
That is why a PET scan result is rarely interpreted in isolation. Doctors often compare it with CT, MRI, prior scans, symptoms, pathology, and lab work. In some cases, a suspicious spot still needs biopsy confirmation.
This is also important with FES PET. It can help show estrogen receptor-positive lesions, but it does not replace biopsy when biopsy is needed. It also does not answer every receptor question. Breast cancer, as always, enjoys being complicated.
Risks and side effects
For most people, PET scans are considered safe, and the amount of radiation involved is relatively low. Still, “low” does not mean “none,” which is why doctors do not order them casually.
Possible downsides include:
- radiation exposure from the tracer and the CT portion of a PET/CT
- minor discomfort, bruising, or soreness at the IV site
- rare allergic reaction to the tracer
- special concerns if you are pregnant or breastfeeding
If you are claustrophobic, uncomfortable lying still, or in pain from surgery or treatment, mention it before the scan starts. Small adjustments can make the experience easier.
How results are read and what happens next
After the scan, a radiologist or nuclear medicine specialist reviews the images and writes a report for your oncology team. You may hear terms like uptake, lesion, metabolic activity, or SUV. SUV stands for standardized uptake value, which is one way of measuring how much tracer a spot absorbs.
Important note: an SUV number is not a crystal ball. A higher number can be concerning, but it does not automatically prove cancer, and a lower number does not automatically rule it out. Context matters, which is why your oncologist’s explanation is far more useful than trying to decode a report like you are cracking a spy file.
The next step after a PET scan may be simple reassurance, a comparison with older imaging, another scan, a change in treatment, or a biopsy of a suspicious area. The scan is a tool, not the whole story.
Questions to ask your doctor before the scan
- Why are you ordering this PET scan for me specifically?
- Is this an FDG PET or an FES PET?
- Do I need to fast, avoid exercise, or adjust medications?
- How will my diabetes, if I have it, affect the prep?
- How will the results change my treatment plan?
- If the scan shows something unclear, what usually happens next?
Bottom line
A breast cancer PET scan is not usually a first-stop screening tool, but it can be extremely valuable when doctors need to look for spread, recurrence, or treatment response. The process is usually straightforward: some prep, an injection, a waiting period, then a scan that requires you to lie still and let the machine do its work.
The bigger challenge is often emotional, not physical. Knowing what to expect can make the entire day feel less mysterious and a little less intimidating. And in cancer care, sometimes “less intimidating” is a major win.
Experiences related to breast cancer PET scans: the human side nobody puts on the appointment card
For many people, the PET scan experience starts long before they enter the imaging room. It starts the minute the test is ordered. Suddenly, everyday life develops a soundtrack of background worry. You may still answer emails, fold laundry, drive to work, and nod through conversations, but part of your brain has already moved into the scan appointment and unpacked a suitcase labeled what if.
Patients often describe the day of the scan as oddly quiet. There is paperwork, a waiting room, an IV, and a lot of polite instructions, but underneath all that routine is a huge emotional question: What will this show? Even people who look calm on the outside may feel like their thoughts are doing cartwheels in dress shoes.
Then there is the strange in-between phase after the tracer injection. You are told to rest, stay still, and relax. Relaxing on command, of course, is one of humanity’s least reliable skills. Some people pray. Some count ceiling tiles. Some rehearse possible conversations with their oncologist. Some decide that the chair is suddenly the most interesting chair ever made because focusing on upholstery is easier than focusing on fear.
During the scan itself, people often report two simultaneous truths. First, the test is usually physically manageable. Second, it feels emotionally enormous. The machine may hum. The room may be cool. The staff may sound reassuring in that calm, practiced way that medical professionals do so well. And still, your mind may wander from practical thoughts to existential ones in about six seconds flat.
Afterward, many patients feel relief simply because the test is over. But that relief can be short-lived because the next phase begins: waiting for results. This is where “scanxiety” tends to show up in full costume. A completely normal ache suddenly becomes suspicious. A harmless headache starts auditioning for a dramatic role. You may check your patient portal too often, then pretend you are not checking it too often, then check it again for accuracy.
It also helps to know that people experience results in very different ways. A clear scan can bring gratitude, tears, and exhaustion all at once. An unclear scan can feel maddening because it does not give the neat answer you wanted. A scan that shows progression can be heartbreaking, but it can also provide the information needed to change course and make a smarter treatment plan. In that sense, even difficult scans can still be useful scans.
One of the most common lessons patients share is this: do not go through PET scan days pretending you are made of concrete. Bring support. Ask questions. Clear your schedule if you can. Let someone drive if you feel emotionally drained. Have a plan for the waiting period after the appointment, whether that means soup, a favorite show, a walk, a nap, or simply ignoring all nonessential humans for the afternoon.
The medical side of a PET scan matters, of course. But so does the human side. Breast cancer imaging is not just about tracer uptake and scan reports. It is also about courage in ordinary clothes, patience you did not ask to develop, and the weirdly heroic act of showing up, lying still, and facing uncertainty one appointment at a time.







