Table of Contents >> Show >> Hide
- What Is Prostate Ultrasound, Exactly?
- How Ultrasound Helps Diagnose Prostate Cancer
- When Ultrasound Becomes Treatment: Meet HIFU
- Can HIFU Cure Prostate Cancer?
- Who Might Be a Good Candidate for HIFU?
- Benefits of Ultrasound-Based Prostate Cancer Treatment
- Limitations and Risks You Should Not Ignore
- Ultrasound vs. MRI vs. Surgery vs. Radiation
- What Doctors Mean by “Focal Therapy”
- So, Can an Ultrasound Help Fight Prostate Cancer?
- Real-World Experiences: What This Journey Often Feels Like
- Conclusion
Let’s start with the short answer: yes, ultrasound can help fight prostate cancer, but not in the magical “wave a wand and poof, problem solved” kind of way. In the real world, ultrasound helps in two big roles. First, it helps doctors find, target, and sample suspicious areas of the prostate during diagnosis. Second, a more powerful version called high-intensity focused ultrasound (HIFU) can actually destroy selected prostate tissue by heating it with concentrated sound waves.
That sounds futuristic because, honestly, it is a little futuristic. But it is also very real. The important catch is that not every ultrasound is a treatment tool, and not every person with prostate cancer is a good fit for HIFU. For many men, standard options like active surveillance, surgery, radiation, hormone therapy, or combinations of these still play a bigger role. Ultrasound is often part of the team, not always the star quarterback.
If you have been wondering whether ultrasound can help diagnose prostate cancer, guide a biopsy, reduce unnecessary treatment, or even destroy a tumor without removing the entire prostate, this guide walks through the science in plain English. No medical mumbo-jumbo pileup. No superhero promises. Just the facts, with a little personality so the reading experience feels less like homework and more like a useful conversation.
What Is Prostate Ultrasound, Exactly?
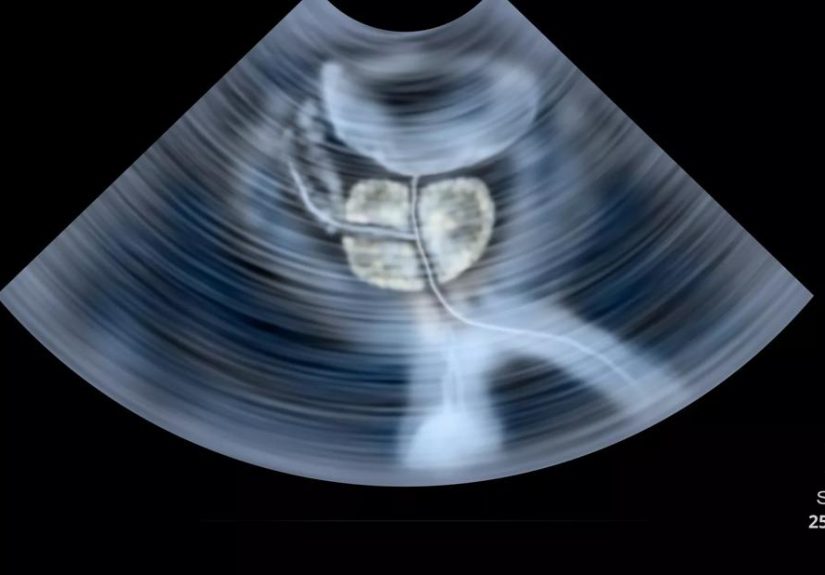
Ultrasound is an imaging method that uses sound waves to create pictures of structures inside the body. In prostate care, doctors often use transrectal ultrasound, sometimes called TRUS. A small probe is placed in the rectum so the prostate can be seen up close. It is not glamorous, but it is practical. Medicine has a way of trading elegance for accuracy, and this is one of those moments.
Standard prostate ultrasound is useful because it shows the shape, size, and location of the gland. It can help a doctor guide a biopsy needle to the right areas. What it does not do especially well is act like a perfect radar screen that lights up every prostate cancer. In fact, many prostate cancers are not clearly visible on regular ultrasound alone.
That is why prostate cancer diagnosis usually does not depend on ultrasound by itself. It works best when combined with other tools, such as:
PSA Testing
A prostate-specific antigen blood test can raise the first red flag. A higher-than-expected PSA does not automatically mean cancer, but it can signal that more investigation is needed.
Digital Rectal Exam
A doctor may feel for lumps or irregularities. Not exactly anyone’s favorite calendar event, but still useful.
MRI and MRI/Ultrasound Fusion
Multiparametric MRI can identify suspicious lesions more clearly than standard ultrasound. During a fusion biopsy, those MRI images are matched with live ultrasound images so doctors can target the biopsy more precisely.
How Ultrasound Helps Diagnose Prostate Cancer
When people ask, “Can an ultrasound help fight prostate cancer?” the first honest answer is this: it helps fight prostate cancer by improving diagnosis. And in cancer care, better diagnosis is not a side note. It is everything. If doctors cannot find the right lesion, grade the cancer correctly, or map where it sits in the prostate, treatment decisions become a lot less accurate.
Here is where ultrasound earns its paycheck:
1. It Guides the Biopsy Needle
A biopsy is the test that confirms whether prostate cancer is really present. During a biopsy, ultrasound helps the doctor see the prostate in real time and guide the needle into the gland. This makes the procedure more controlled and more accurate than flying blind.
2. It Works With MRI to Target Suspicious Areas
Traditional systematic biopsy samples multiple parts of the prostate, almost like taking several random bites out of a muffin to check for blueberries. MRI/ultrasound fusion biopsy is smarter. If an MRI shows a suspicious lesion, the doctor can use live ultrasound during the biopsy to target that specific area while also taking standard samples.
3. It Helps Some Men Avoid Missed Significant Cancers
Fusion-guided biopsies can improve the detection of clinically significant prostate cancer. That matters because the real goal is not simply to find any cancer. The goal is to identify the cancers that are more likely to grow, spread, or require treatment.
4. It Can Support Safer Biopsy Techniques
Many centers now use transperineal biopsy, where the needle enters through the skin between the scrotum and anus instead of through the rectum. Ultrasound can help guide that approach too. One reason doctors like it is the lower infection risk compared with the traditional transrectal route.
When Ultrasound Becomes Treatment: Meet HIFU
Now for the more dramatic part of the story. Standard ultrasound helps doctors see and guide. High-intensity focused ultrasound, or HIFU, is different. It helps doctors treat.
HIFU works by focusing intense sound waves on a specific area of prostate tissue. That energy creates heat. The heat damages or destroys the targeted cells. In prostate cancer care, this is often used as a form of focal therapy, meaning treatment is aimed at the tumor or the most dangerous part of the prostate rather than removing or radiating the whole gland.
That is the key distinction. HIFU is not just taking a picture. It is using sound energy as a therapeutic tool.
How HIFU Is Performed
Most HIFU procedures are done with a probe placed in the rectum. The device delivers focused ultrasound energy into the prostate. The treatment is planned carefully using imaging, and the goal is to destroy the target while sparing as much healthy surrounding tissue as possible.
Because HIFU is usually a minimally invasive outpatient procedure, it can sound appealing to people who want an alternative to major surgery or full-gland radiation. And yes, that appeal is understandable. If someone says, “You may be able to treat the tumor and keep more of the prostate untouched,” most people will listen very closely.
Can HIFU Cure Prostate Cancer?
This is where nuance matters more than hype.
For selected men with localized prostate cancer, HIFU may control or eliminate the targeted area of disease. Some cancer centers in the United States use it as a focal therapy option for carefully chosen patients. But HIFU is not a guaranteed cure, and it is not the best or standard answer for everyone.
Why not? Because prostate cancer is not one-size-fits-all. Some tumors are tiny and slow-growing. Some are more aggressive. Some are confined to one visible lesion. Others are multifocal, meaning there are several cancer spots in different parts of the prostate. If cancer is spread beyond the gland, HIFU is usually not the right tool to solve the bigger problem.
That means the real question is not just, “Can ultrasound fight prostate cancer?” The better question is, “Which kind of ultrasound, for which patient, at which stage, with what goal?”
Who Might Be a Good Candidate for HIFU?
HIFU is generally considered for men with localized prostate cancer, especially when the cancer appears to be in a limited area that can be targeted. Some specialists describe the ideal patient as someone with a visible lesion on MRI, biopsy-confirmed disease in a defined region, and a prostate anatomy that allows the treatment to reach the target safely.
Potential candidates may include men who:
- Have low- to intermediate-risk localized prostate cancer in a clearly defined area
- Want a focal therapy option instead of whole-gland treatment
- Are trying to reduce the risk of side effects such as urinary leakage or sexual dysfunction
- Need treatment for recurrent localized disease after prior radiation in selected cases
On the other hand, HIFU may be less suitable for men with:
- Large or difficult-to-reach prostate anatomy
- Cancer in multiple areas of the gland
- High-risk disease that may need broader treatment
- Evidence that the cancer has spread beyond the prostate
This is why treatment planning often includes PSA trends, biopsy results, MRI findings, pathology grade group, prostate size, symptoms, age, overall health, and the patient’s priorities. Cancer treatment is part medical science, part strategy, and part very honest conversation.
Benefits of Ultrasound-Based Prostate Cancer Treatment
When HIFU is used in the right setting, it offers some real advantages.
Less Invasive Than Surgery
There is no large incision, no removal of the entire prostate, and typically a shorter recovery compared with radical prostatectomy.
Focused Treatment
Because the ultrasound energy is aimed at the target, healthy tissue may be spared. That is the whole point of focal therapy.
Potentially Fewer Side Effects
Many men are interested in HIFU because it may lower the risk of some urinary, bowel, and sexual side effects compared with more aggressive whole-gland treatments. That does not mean zero side effects. It means the side-effect profile may be more favorable in some carefully chosen cases.
Outpatient Convenience
HIFU is often done as an outpatient procedure, which can be attractive for people who would rather not spend extra time in a hospital bed wearing socks with suspiciously low self-esteem.
Limitations and Risks You Should Not Ignore
Every treatment has trade-offs, and HIFU is no exception.
It Does Not Replace Every Standard Treatment
For many men, surgery or radiation remains the most established choice, especially when the cancer is more extensive or aggressive.
Long-Term Cancer Control Is Still Being Studied
HIFU is promising, but long-term data are not as mature as they are for radical prostatectomy or radiation therapy. That makes some experts cautious, especially for younger men or those with higher-risk tumors.
Follow-Up Is Essential
Even after HIFU, patients often need ongoing PSA testing, MRI imaging, and sometimes repeat biopsy. In other words, HIFU is not a “one and done, never think about your prostate again” coupon.
Side Effects Can Still Happen
Possible complications may include urinary symptoms, retention, infection, erectile dysfunction, urethral stricture, and, more rarely, injury to nearby tissues. The risk profile depends on the treatment approach, anatomy, and whether the area has been treated before.
Ultrasound vs. MRI vs. Surgery vs. Radiation
These options are not exactly competing in the same lane.
Standard ultrasound is mostly a guidance tool. It helps biopsy and procedural planning.
MRI is usually better for finding suspicious lesions and staging localized disease.
MRI/ultrasound fusion biopsy combines the strengths of both.
HIFU is a treatment option for selected cases of localized prostate cancer.
Surgery and radiation remain the most established definitive treatments for many men, especially when doctors want a proven whole-gland approach.
Active surveillance is often the smartest option for low-risk prostate cancer, because some cancers grow so slowly that immediate treatment may create more trouble than the cancer itself.
The best treatment is not the newest gadget. It is the option that matches the biology of the cancer and the goals of the patient.
What Doctors Mean by “Focal Therapy”
Focal therapy is a middle path between doing too much and doing too little. Instead of removing or irradiating the whole prostate, focal therapy aims to destroy the most important cancer area while preserving the rest of the gland.
That sounds smart because it is smart, at least in theory and in selected practice. Prostate cancer is often diagnosed earlier than it used to be, and imaging has improved dramatically. That means doctors can sometimes identify exactly where the dangerous lesion is and target it more precisely.
HIFU is one of the best-known focal therapy approaches, but it is not the only one. Other focal therapies include cryotherapy, laser ablation, and transurethral ultrasound ablation. The broader message is that prostate cancer treatment is becoming more personalized. Less sledgehammer, more scalpel.
So, Can an Ultrasound Help Fight Prostate Cancer?
Yes, but the answer has layers.
Regular prostate ultrasound helps fight prostate cancer by improving diagnosis, guiding biopsies, and working with MRI to target suspicious lesions more accurately.
Focused therapeutic ultrasound, especially HIFU, may help fight prostate cancer by destroying selected areas of cancerous prostate tissue in men with localized disease who are good candidates for focal therapy.
That is the realistic answer. Ultrasound is not a universal cure. It is a powerful tool. In the right hands and for the right patient, it can help doctors diagnose more intelligently and, in selected cases, treat more precisely.
If there is one takeaway worth remembering, it is this: the question is not whether ultrasound is useful, but how it fits into the bigger treatment plan. For some men, it is the map. For some, it is part of the weapon. For others, it is one helpful tool among many.
Real-World Experiences: What This Journey Often Feels Like
When people first hear the phrase “ultrasound for prostate cancer,” they often imagine something simple, quick, and maybe a little miraculous. The real experience is usually more human than that. It often starts with a PSA result that is mildly unsettling, followed by a doctor saying something like, “Let’s take a closer look.” That sentence has launched approximately one billion internet searches and at least several million sleepless nights.
For many men, the diagnostic phase is the strangest part. You may feel completely normal, yet suddenly you are learning terms like Grade Group, lesion, fusion biopsy, and active surveillance. A prostate MRI may find an area of concern, and then ultrasound enters the picture during the biopsy. Patients often describe this stage as emotionally weird because the technology feels incredibly advanced while the waiting feels painfully primitive. The scan happens quickly. The pathology wait feels like it was invented by a villain.
Men who go through an MRI/ultrasound fusion biopsy often say they appreciate the idea that the doctor is not just sampling randomly. There is reassurance in knowing the biopsy is more targeted. Some describe the procedure itself as uncomfortable but manageable, especially when the care team explains each step clearly. Others say the bigger challenge is not physical pain but the mental treadmill afterward: “What did they find, how serious is it, and what happens next?”
When HIFU enters the conversation, reactions are often mixed. On one hand, many patients are relieved to hear there may be a less invasive treatment than surgery or full-gland radiation. On the other hand, they quickly realize that “less invasive” does not mean “no big decision.” Men considering HIFU often ask practical questions: Will I need a catheter? What happens to my PSA afterward? What are the odds I will still need surgery or radiation later? Will this affect urinary control or erections? Those are exactly the right questions, because the experience is not just about killing tissue. It is about living with the outcome.
Families often go through their own version of the same journey. A spouse or partner may hear “focal therapy” and think, “Great, smaller treatment, smaller problem.” Then the specialist explains the need for follow-up PSA tests, repeat imaging, and sometimes another biopsy. That is when many families realize that prostate cancer care is often a marathon of monitoring, not a single dramatic finish line moment.
Some men feel empowered by HIFU because it seems to fit their priorities: treat the target, preserve quality of life, and stay as minimally invasive as possible. Others prefer the certainty of surgery or radiation because they want the most established long-term path. Neither reaction is irrational. In fact, they show exactly why prostate cancer care has become so individualized. The “best” experience is usually the one where the patient understands the trade-offs, trusts the team, and feels the final decision matches his values.
In everyday life, the experience after diagnosis is often less cinematic than expected. People still go to work, answer emails, walk the dog, forget why they opened the refrigerator, and worry quietly between appointments. That may be the most honest picture of all. Prostate cancer care is often not one giant dramatic battle scene. It is a series of careful decisions, small recoveries, repeat checks, and ongoing effort to balance cancer control with normal life. Ultrasound can absolutely help in that journey. It just does its best work as part of a smart, personalized plan.
Conclusion
Ultrasound can help fight prostate cancer, but the real story is bigger than a yes-or-no headline. Standard ultrasound helps doctors guide biopsies and improve diagnosis. MRI/ultrasound fusion makes that process more precise. HIFU takes ultrasound one step further by using focused sound waves to destroy selected prostate tissue in carefully chosen patients with localized disease.
That combination of imaging, targeting, and focal treatment is one reason prostate cancer care is becoming more personalized. Still, ultrasound is not a one-size-fits-all cure. Some men are better served by active surveillance. Others need surgery, radiation, hormone therapy, or a combination approach. The smartest move is not chasing the newest buzzword. It is matching the right tool to the right cancer at the right time.
So yes, an ultrasound can help fight prostate cancer. Sometimes it helps doctors find the enemy. Sometimes it helps them hit the target. And sometimes, that difference is exactly what changes the whole game.