Table of Contents >> Show >> Hide
- What Colon Cancer and Shingles Actually Are
- Is There a Proven Link Between Colon Cancer and Shingles?
- Why People With Colon Cancer May Have a Higher Risk of Shingles
- Symptoms: How the Two Conditions Differ
- Colon Cancer Prevention: The Big Levers That Actually Matter
- Shingles Prevention: Do the Obvious Smart Thing
- What Prevention Looks Like When Both Risks Are on Your Mind
- Practical Examples
- Experience-Based Section: What This Can Feel Like in Real Life
- Conclusion
At first glance, colon cancer and shingles seem like two strangers trapped in the same elevator. One affects the digestive tract. The other shows up as a painful rash caused by a virus that decided retirement was boring. But researchers and clinicians have spent years asking whether there is any meaningful connection between the two.
The answer is more nuanced than a dramatic headline suggests. Shingles does not cause colon cancer. Colon cancer does not magically produce shingles. Still, the two conditions can intersect in important ways, especially when the immune system enters the chat. Some people with cancer, including people undergoing treatment for colon cancer, may face a higher risk of shingles because cancer and certain therapies can weaken immune defenses. At the same time, shingles itself is not considered a proven warning sign that someone has colon cancer.
That distinction matters. It keeps people from panicking over the wrong thing while paying attention to the right ones: screening, vaccination, symptom awareness, and prevention. In other words, less doom-scrolling, more real strategy.
What Colon Cancer and Shingles Actually Are
Colon cancer in plain English
Colon cancer begins in the colon, which is part of the large intestine. It often starts as a polyp, a growth that may be harmless at first but can become cancer over time. That is why screening matters so much. It does not just find cancer early. In many cases, it helps prevent cancer by catching and removing precancerous polyps before they become a bigger problem.
Common warning signs of colon cancer can include blood in the stool, changes in bowel habits, ongoing abdominal discomfort, unexplained weight loss, fatigue, or anemia. The tricky part is that early colon cancer may cause no symptoms at all. That is why waiting until your body sends a dramatic memo is not a great prevention plan.
Shingles in plain English
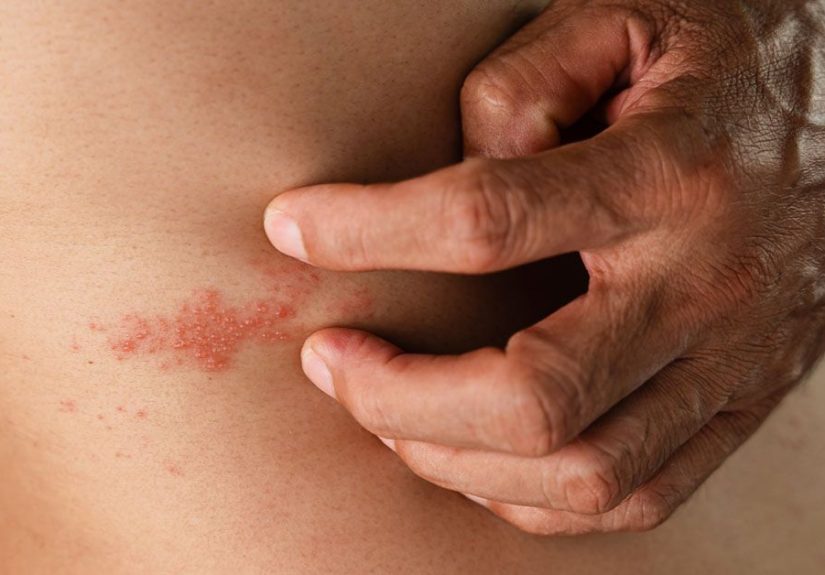
Shingles, also called herpes zoster, happens when the varicella-zoster virus reactivates years after a person has had chickenpox. Instead of staying quiet forever, the virus can wake up and cause a painful rash, usually on one side of the body or face. Before the rash appears, people may notice burning, tingling, itching, or pain in a specific area. Then come the blisters, because apparently the virus enjoys theatrics.
Shingles can be miserable on its own, but the bigger concern is complications. The best-known one is postherpetic neuralgia, which is long-lasting nerve pain that can stick around well after the rash clears. In some cases, shingles can also affect the eyes, hearing, or nervous system.
Is There a Proven Link Between Colon Cancer and Shingles?
The most accurate answer is this: there is no proven evidence that shingles causes colon cancer, and there is no standard medical rule saying that everyone with shingles should be investigated for colon cancer just because they had shingles.
However, researchers have explored whether shingles may sometimes appear more often in people with weakened immune systems, including some people who already have cancer or later turn out to have a malignancy. The results are mixed. Some observational studies have reported an association between shingles and certain later cancer diagnoses, while other studies have found no overall increase in cancer risk after shingles in the general population.
That means shingles is best understood as a possible signal of immune stress in some situations, not as a direct cause of colon cancer and not as a reliable shortcut to diagnosing it. A painful rash on your side is not your colon sending Morse code.
What the research suggests
Research has consistently shown that cancer can raise the risk of shingles, especially when treatment suppresses immune function. This is more clearly established than the reverse question. People with solid tumors and blood cancers may be more vulnerable to shingles after starting immunosuppressive treatment, and the risk may be higher in the period after diagnosis or during active therapy.
For colon cancer specifically, the most relevant issue is not that shingles predicts the cancer. It is that colon cancer treatment may leave some patients more susceptible to infection or viral reactivation. That is where prevention becomes especially important.
Why People With Colon Cancer May Have a Higher Risk of Shingles
The immune system is deeply involved in both cancer surveillance and infection control. When cancer develops, or when treatment targets rapidly dividing cells, the immune system can become less efficient. That creates an opening for the dormant varicella-zoster virus to reactivate.
Several factors may increase shingles risk in a person with colon cancer:
- Chemotherapy: Some chemotherapy regimens reduce white blood cell counts and overall immune resilience.
- Steroids or other immunosuppressive drugs: These medications may be used during treatment and can make viral reactivation more likely.
- Older age: Colon cancer becomes more common with age, and shingles risk also rises as people get older.
- General health stress: Surgery, poor nutrition, fatigue, and chronic illness can all make recovery harder.
- Other medical conditions: Diabetes, kidney disease, or other immune-related conditions may add to the risk.
This overlap is one reason oncologists and primary care clinicians increasingly talk about vaccination and infection prevention earlier in the care journey, not as an afterthought once the patient is already exhausted and living on crackers.
Symptoms: How the Two Conditions Differ
Colon cancer and shingles usually do not look alike, which is helpful. Colon cancer tends to affect bowel habits, stool, abdominal comfort, weight, and energy levels. Shingles tends to announce itself with nerve pain, tingling, and a one-sided rash with blisters.
Still, confusion can happen. A person undergoing colon cancer treatment may develop new pain or fatigue and assume it is “just treatment.” Someone with shingles may focus on the rash and ignore other symptoms like rectal bleeding or persistent bowel changes. Bodies rarely submit one issue at a time like polite office coworkers.
If symptoms do not fit neatly into one box, that is a good reason to call a clinician instead of trying to win a diagnostic guessing game online.
Colon Cancer Prevention: The Big Levers That Actually Matter
1. Get screened on time
For adults at average risk, colorectal cancer screening now starts at age 45. Screening is one of the strongest prevention tools in modern medicine because it can find polyps before they become cancer. Colonoscopy gets much of the spotlight, but it is not the only option. Stool-based tests and other approved screening methods may also be appropriate depending on personal risk, access, and medical guidance.
If you have a family history of colorectal cancer, inflammatory bowel disease, a history of certain polyps, or hereditary syndromes such as Lynch syndrome or familial adenomatous polyposis, you may need earlier or more frequent screening. In that situation, “I’ll deal with it later” is not a strategy. It is a scheduling error wearing a fake mustache.
2. Pay attention to family history
Family history can significantly change risk. If a parent, sibling, or child has had colorectal cancer, your clinician may recommend earlier screening. The same goes for a family pattern of colon, uterine, ovarian, or other related cancers that could point to an inherited syndrome.
3. Protect the basics
While no lifestyle plan can guarantee prevention, several habits are associated with lower colorectal cancer risk. These include staying physically active, maintaining a healthy weight, avoiding smoking, limiting alcohol, and choosing a diet that emphasizes fruits, vegetables, whole grains, and other high-fiber foods while cutting back on processed meat and excessive red meat.
This is not glamorous advice. Nobody is printing “Walk More, Eat Beans” on a luxury yacht. But boring prevention habits often outperform dramatic wellness trends.
4. Do not ignore symptoms
Blood in the stool, unexplained anemia, persistent constipation or diarrhea, narrow stools, ongoing abdominal pain, or weight loss without trying deserve medical evaluation. Not because every symptom equals cancer, but because waiting for certainty can cost valuable time.
Shingles Prevention: Do the Obvious Smart Thing
1. Get vaccinated if eligible
The shingles vaccine, Shingrix, is recommended for adults age 50 and older. It is also recommended for adults age 19 and older who are immunocompromised or will become immunocompromised because of disease or therapy. It is given in two doses.
For people with cancer, timing matters. The best time to receive vaccines may depend on when treatment starts and what kind of therapy is planned. This is not a DIY calendar project. If you have colon cancer or are preparing for treatment, ask your oncology team when shingles vaccination makes the most sense.
2. Take symptoms seriously and act early
If you develop tingling, burning pain, or a one-sided blistering rash, get medical attention quickly. Antiviral treatment started early can help reduce severity and complications. This is especially important for people with weakened immune systems and for anyone with rash near the eye.
3. Support immune health during treatment
No supplement stack can turn you into a superhero, but practical steps still matter. Follow your treatment plan, eat as well as you can, stay hydrated, rest, report fevers or new rashes promptly, and keep up with infection-prevention guidance from your care team. Small habits become very large habits when the immune system is under pressure.
What Prevention Looks Like When Both Risks Are on Your Mind
If you are worried about both colon cancer and shingles, the smartest plan is not panic. It is prioritization.
First, know your colorectal cancer screening status. If you are 45 or older and average risk, make sure screening is on your calendar. If you are younger but have strong risk factors, ask whether earlier evaluation is appropriate.
Second, know your shingles vaccine status. If you are 50 or older, or if you are immunocompromised, talk with your clinician about Shingrix. If you are already in cancer treatment, ask about timing rather than assuming it is too late or automatically off the table.
Third, pay attention to symptoms that do not belong to your normal routine. Colon cancer symptoms and shingles symptoms usually point in different directions, but both deserve timely care. A new one-sided painful rash is not something to “watch for a month.” Neither is recurring rectal bleeding.
Practical Examples
Example 1: A 52-year-old adult with no major symptoms delays colon cancer screening because work is busy and life is chaos. They also skip the shingles vaccine because they “feel fine.” That person is missing two strong prevention opportunities that could dramatically reduce future health trouble.
Example 2: A 63-year-old patient starting chemotherapy for colon cancer asks the oncology team about infection risk and vaccines before treatment begins. That conversation may help guide vaccine timing, symptom monitoring, and faster treatment if shingles appears.
Example 3: A person develops shingles and becomes convinced it means they have colon cancer. In reality, shingles alone is not a diagnosis of underlying colon cancer. The more sensible move is to treat the shingles, review routine screening needs, and evaluate any actual colorectal symptoms or risk factors.
Experience-Based Section: What This Can Feel Like in Real Life
Health articles often sound polished and tidy, but real life is usually neither. People rarely experience “colon cancer risk” or “shingles prevention” as clean academic topics. They experience them as a weird mix of fear, procrastination, denial, scheduling conflicts, and late-night internet rabbit holes.
One common experience is the person who feels completely normal and therefore assumes screening can wait. They are not reckless. They are busy. They have work, family, bills, and a talent for putting awkward medical tasks behind literally anything else, including reorganizing a junk drawer. Then a friend gets diagnosed, or a headline about early-onset colorectal cancer appears, and suddenly the idea of screening becomes less abstract. Many people describe this moment as the point when prevention stops feeling optional and starts feeling personal.
Another common experience happens in cancer treatment itself. A person already dealing with surgery, scans, treatment decisions, and side effects may not have “ask about shingles” at the top of the list. That is understandable. When your calendar already looks like a medical scavenger hunt, adding one more issue can feel absurd. But patients and caregivers often say that seemingly small preventive conversations become incredibly valuable later. Knowing what shingles looks like, when to call, and whether vaccination is appropriate can reduce stress because there is finally a plan instead of a vague cloud of worry.
Caregivers have their own version of the experience. They are often the ones noticing changes first: a rash, a complaint about burning pain, a strange level of fatigue, a stubborn refusal to schedule screening. They also live with the emotional whiplash of not wanting to overreact while being terrified of underreacting. That balancing act is exhausting. Many families find relief when they replace “Should we panic?” with “What is the next smart step?” Usually that means calling a clinician, reviewing symptoms clearly, and sticking to evidence-based prevention rather than guesses.
There is also the emotional side of mixed medical information. People hear that shingles is linked to immune problems, then read something about cancer, and suddenly every symptom feels loaded with hidden meaning. This is where clear communication matters. The most helpful message is not “ignore it” and not “assume the worst.” It is “take the right action for the right reason.” Treat shingles early. Stay current on screening. Talk to your doctor about family history, vaccine timing, and treatment-related risk. Let medicine do the detective work.
In the end, the experience many people remember most is not the article they read or the statistic they memorized. It is the moment they stopped avoiding the issue and did the practical thing: booked the screening, asked the vaccine question, reported the rash, or followed up on symptoms that had been easy to dismiss. Prevention often feels unremarkable in the moment. Later, it can feel like one of the smartest decisions a person ever made.
Conclusion
Colon cancer and shingles are not the same disease, and shingles is not a proven cause of colon cancer. But the two can overlap through one important pathway: immune vulnerability. People with colon cancer, especially those receiving immunosuppressive treatment, may have a higher risk of shingles. That makes prevention more practical than theoretical.
The take-home message is simple. Stay current with colorectal cancer screening. Know your personal risk factors. Consider shingles vaccination if you are eligible. If you are living with colon cancer or preparing for treatment, ask your care team about infection risk and vaccine timing. And if your body starts sending unusual signals, do not negotiate with them like they are spam emails.







