Table of Contents >> Show >> Hide
- What Is a Nerve Conduction Velocity Test?
- Why Would You Need an NCV Test?
- NCV vs. EMG: What Is the Difference?
- How to Prepare for a Nerve Conduction Study
- What Happens During the Test?
- Is a Nerve Conduction Velocity Test Painful?
- What Do NCV Results Mean?
- What an NCV Test Cannot Tell You
- Risks and Safety
- After the Test: What Comes Next?
- Examples of How NCV Results Help in Real Life
- Real-World Experiences With Nerve Conduction Velocity Testing
- Conclusion
If your doctor says, “We’d like to do a nerve conduction velocity test,” you may immediately picture something between a science experiment and a robot handshake. The good news is that a nerve conduction velocity test, often called an NCV or nerve conduction study, is far less dramatic than it sounds. It is a common diagnostic tool used to see how well your nerves are sending electrical signals. In plain English, it helps answer a very important question: are your nerves doing their job at full speed, or are they lagging like weak Wi-Fi in the back bedroom?
This test is often used when someone has numbness, tingling, burning pain, weakness, muscle cramps, or unexplained changes in sensation. It can help identify whether the problem is happening in a nerve, how severe the issue may be, and whether the pattern points toward a condition such as peripheral neuropathy, carpal tunnel syndrome, ulnar nerve entrapment, radiculopathy, or another nerve disorder. Because nerve symptoms can be vague and annoyingly similar from one condition to another, NCV testing gives doctors objective information instead of guesswork.
Below, we will break down what an NCV test is, why it is done, what the procedure feels like, how results are interpreted, and what patients commonly experience before, during, and after testing. No medical jargon avalanche. No dramatic TV-show hospital scenes. Just the facts, explained like a normal person would want to hear them.
What Is a Nerve Conduction Velocity Test?
A nerve conduction velocity test measures how fast an electrical impulse travels through a peripheral nerve. Peripheral nerves are the communication lines that carry messages between your brain, spinal cord, muscles, skin, and organs. When these nerves are healthy, signals travel efficiently. When they are damaged, compressed, inflamed, or stripped of their protective myelin covering, those signals may slow down, weaken, or fail to travel properly.
During the test, small electrodes are placed on the skin over a nerve and the muscle or sensory area connected to it. A brief electrical pulse stimulates the nerve, and the machine records how quickly and strongly the signal travels. That timing and response help clinicians figure out whether a nerve problem is present and what kind of problem it may be.
You may also hear the test called a nerve conduction study or NCS. The term NCV refers specifically to the speed of conduction, but in everyday practice, people often use NCV and NCS interchangeably.
Why Would You Need an NCV Test?
Doctors usually order an NCV test when symptoms suggest a nerve problem rather than, or in addition to, a muscle or joint problem. Common reasons include persistent tingling in the hands or feet, numbness, burning pain, weakness, hand clumsiness, foot drop, muscle cramps, or pain that suggests a pinched nerve.
Common conditions an NCV test may help evaluate
- Carpal tunnel syndrome
- Ulnar nerve compression at the elbow or wrist
- Peripheral neuropathy, including diabetic neuropathy
- Sciatic or other nerve injuries
- Guillain-Barré syndrome and chronic inflammatory demyelinating neuropathies
- Brachial plexus or peroneal nerve injuries
- Neuromuscular disorders when combined with EMG
An NCV test is especially useful because symptoms alone cannot always tell the full story. For example, hand numbness could come from carpal tunnel syndrome, a pinched nerve in the neck, generalized neuropathy, or even a combination of issues. A nerve conduction study helps narrow that down by showing where the signal slows, how much it slows, and whether the abnormality fits a known pattern.
NCV vs. EMG: What Is the Difference?
This is where many patients get tripped up. A nerve conduction study and an electromyography test, or EMG, are related but not identical.
NCV/NCS looks at how electrical signals move along the nerve. EMG looks at how muscles respond to nerve signals and records electrical activity inside the muscle using a thin needle electrode. In many cases, doctors order both tests together because they answer different parts of the same question.
Think of it this way: if your body were a concert stage, the nerve conduction study checks whether the microphone cable is transmitting sound, while the EMG checks whether the speaker is actually producing music. One tests the wiring, the other tests the performance.
How to Prepare for a Nerve Conduction Study
Preparation is usually simple, but a few small details matter more than people expect.
Before the test
- Skip lotions, creams, oils, sunscreen, and perfume on the day of the test because they can interfere with electrode contact.
- Tell your provider if you have a pacemaker, implanted defibrillator, deep brain stimulator, or another implanted device.
- Tell the clinic if you take blood thinners, especially if a needle EMG will also be performed.
- Try to stay warm. Cold skin can slow nerve conduction and distort results.
- Wear loose, comfortable clothing that can be rolled up easily.
Most people do not need to fast, stop routine medications, or arrange recovery time after a basic NCV test. If your appointment also includes EMG, your clinician may give extra instructions depending on your health history.
What Happens During the Test?
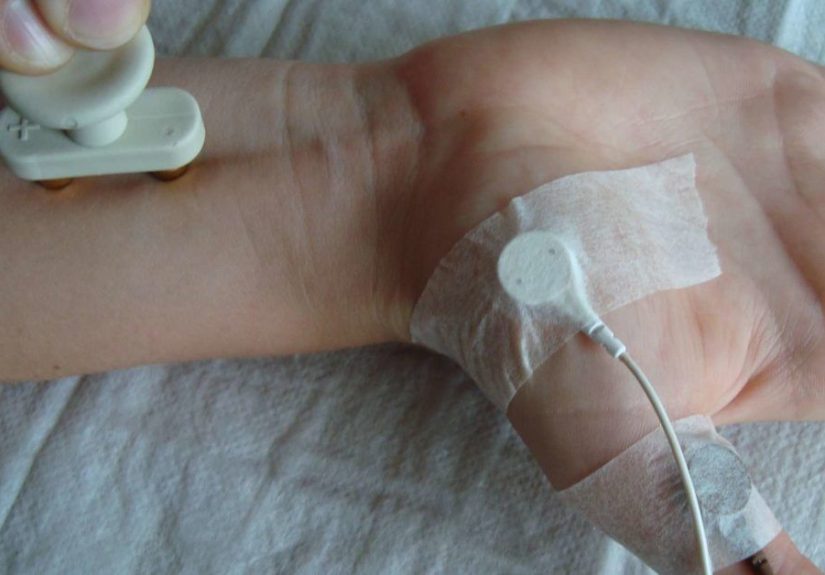
The procedure is usually done in an outpatient clinic, neurology office, or hospital lab. You will sit or lie down while the technician or physician places flat electrodes on your skin. Another electrode delivers tiny electrical pulses at specific points along the nerve.
When the pulse is delivered, you may feel a quick tingling, tapping, zapping, or static-shock sensation. It is not exactly fun, but it is usually brief. Many patients describe it as startling rather than painful. Others say it is mildly uncomfortable but very manageable. The experience depends on which nerves are tested, how sensitive you are, and whether EMG is added afterward.
The provider may test several nerves in one arm, one leg, or multiple limbs. The machine records the speed of the response, the delay before the response begins, and the size of the response. These measurements help determine whether the nerve signal is normal, slowed, blocked, or reduced.
How long does an NCV test take?
A simple study may take 15 to 30 minutes. A more detailed evaluation, especially one combined with EMG, can take 45 minutes to an hour or longer. The length depends on how many nerves need to be checked and how complex the symptoms are.
Is a Nerve Conduction Velocity Test Painful?
“Painful” may be too strong a word for most people, but “weirdly unpleasant for a few seconds at a time” is pretty fair. The electrical pulses can feel sharp, sudden, and surprising, but they are very short. Many patients tolerate the test without much trouble and go right back to work, school, or normal activities afterward.
If the appointment includes a needle EMG, that part is more likely to cause soreness or minor bruising afterward. The needle used is thin, but muscles can feel tender for a day or two. That said, severe complications are uncommon, and a standard NCV study alone has no known long-term side effects.
What Do NCV Results Mean?
This is the part everyone wants to skip ahead to, but results are not as simple as “pass” or “fail.” A nerve conduction study generates several measurements, and each one tells part of the story.
Key measurements in an NCV test
- Conduction velocity: how fast the signal travels along the nerve
- Latency: how long it takes the signal to begin after stimulation
- Amplitude: how strong the response is
- Conduction block or temporal dispersion: patterns that may suggest a focal or demyelinating problem
If the signal travels too slowly, the myelin sheath around the nerve may be damaged. Myelin acts like insulation around a wire, helping signals move quickly and efficiently. Slowed conduction can suggest a demyelinating process or localized compression, such as carpal tunnel syndrome.
If the signal is weak, the axon itself, the core of the nerve fiber, may be injured. Reduced amplitude is often more associated with axonal damage. In real clinical practice, though, results are interpreted together rather than in isolation. A provider looks at the full pattern across multiple nerves and compares it with the symptoms and physical exam.
What is considered normal?
Normal values vary by nerve, age, height, limb temperature, and laboratory standards. That is why reading your own report without context can be a little like diagnosing your car by listening to one engine noise on the internet. It may sound impressive, but it usually ends badly.
Children do not have the same expected values as adults, and cold limbs can artificially slow conduction. Different nerves in the body also normally conduct at different speeds. For that reason, the doctor interprets the numbers using the lab’s reference ranges and your clinical situation.
What abnormal results may suggest
- Compressed or trapped nerves, such as carpal tunnel syndrome or cubital tunnel syndrome
- Peripheral neuropathy related to diabetes, toxins, vitamin deficiencies, or autoimmune disease
- Demyelinating neuropathies, where the nerve coating is damaged
- Axonal neuropathies, where the nerve fiber itself is injured
- Nerve trauma or recovery after injury
- Conditions affecting nerve roots, plexuses, or motor neurons when interpreted with EMG
An abnormal NCV result does not automatically point to one diagnosis. Instead, it narrows the field and helps guide the next steps, which may include blood work, imaging, follow-up electrodiagnostic testing, or targeted treatment.
What an NCV Test Cannot Tell You
Although nerve conduction studies are extremely useful, they are not magic. They do not diagnose every nerve condition on their own. Small fiber neuropathy, for example, can cause real symptoms even when standard nerve conduction studies are normal because those tests are better at evaluating larger nerve fibers.
NCV also does not always reveal the root cause of a nerve problem. It can show that a nerve is affected and help characterize the pattern, but further evaluation may still be needed to find out whether the cause is diabetes, autoimmune disease, a vitamin deficiency, a compression injury, a hereditary disorder, or something else entirely.
Risks and Safety
For most people, an NCV test is very safe. The electrical impulses used are low voltage, and there are no known long-term side effects from the stimulation itself. The main downside is temporary discomfort during the test.
If EMG is added, there is a small risk of bruising, bleeding, infection, or localized pain where the needle is inserted. Patients with implanted cardiac devices or certain neurologic implants should tell the care team beforehand so the test can be planned appropriately.
After the Test: What Comes Next?
Most patients can resume normal activity immediately. If you had only the NCV portion, you will likely walk out feeling completely normal except perhaps slightly annoyed that your nerves got such a thorough performance review. If you also had EMG, you might have some mild muscle soreness for a day or two.
Results may be discussed the same day or sent to the referring clinician for interpretation. The report is typically reviewed alongside your symptoms, exam findings, medical history, and any imaging or lab work. This is important because electrodiagnostic testing is one piece of the diagnostic puzzle, not the whole box.
Examples of How NCV Results Help in Real Life
Example 1: Suspected carpal tunnel syndrome
A person has nighttime hand numbness, dropping objects, and tingling in the thumb, index finger, and middle finger. An NCV study may show slowing across the wrist in the median nerve, which strongly supports carpal tunnel syndrome.
Example 2: Tingling in both feet
A person with diabetes develops burning pain and numbness in both feet. The NCV study may show a length-dependent peripheral neuropathy affecting sensory and motor nerves, which helps confirm that the symptoms are related to nerve damage rather than a circulation issue or simple muscle fatigue.
Example 3: Foot drop after leg injury
A patient develops difficulty lifting the foot after prolonged leg crossing or trauma near the knee. An NCV test may show a peroneal nerve lesion, helping localize the injury and estimate severity.
Real-World Experiences With Nerve Conduction Velocity Testing
For many patients, the hardest part of a nerve conduction study is not the test itself. It is the uncertainty leading up to it. People arrive wondering whether the numbness in their fingers means permanent damage, whether the burning in their feet is getting worse, or whether their weakness is “just stress” or something more serious. By the time they reach the electrodiagnostic lab, many are equal parts worried, tired, and eager for answers.
A common experience is surprise at how fast the appointment moves. Patients often expect something dramatic, but the setup is usually straightforward. Electrodes are placed on the skin, the provider explains what will happen, and then the first electrical pulse lands with that classic reaction: “Oh! That’s weird.” It is a very specific kind of weird. Not exactly painful for everyone, but definitely attention-grabbing. Many patients say the anticipation was worse than the test itself.
People being evaluated for carpal tunnel syndrome often describe relief when the results finally match what they have been feeling for months. Hand numbness at night, tingling while driving, weakness when opening jars, and that irritating tendency to drop a phone at the worst possible moment can seem vague or easy to dismiss. When the study shows slowing across the wrist, patients often feel validated. They are not imagining it, and now there is a clearer path toward treatment.
Others have the opposite experience: symptoms are real, but the standard nerve conduction study comes back normal. That can feel frustrating at first, especially for those with burning pain or sensory changes. But a normal study does not mean nothing is wrong. In some cases, it pushes the evaluation in a more useful direction, such as small fiber neuropathy testing, blood work, imaging, or a closer look at medication effects and autoimmune causes. In that sense, even a normal test can be helpful because it rules out certain patterns of nerve injury.
Patients with more widespread symptoms, such as diabetic neuropathy or suspected inflammatory neuropathy, often describe the test as an important turning point. Before the study, their symptoms may feel random: numb toes, balance issues, leg cramps, strange buzzing sensations, weakness climbing stairs. After the study, the pattern can start to make sense. Even if the diagnosis is not finalized that day, the results often give the doctor a map for what to investigate next.
Emotionally, one of the most powerful parts of the experience is finally getting objective data. Nerve symptoms can be invisible. Friends cannot see them. Coworkers may not understand them. Some patients even start doubting themselves. A nerve conduction study can provide concrete evidence that the nerve signal is slowed, reduced, or blocked. That clarity matters. It turns a mysterious symptom into something measurable and gives both patient and clinician a better starting point for treatment decisions.
In the end, most people leave saying some version of the same thing: “I wouldn’t call it enjoyable, but I’m glad I did it.” That is probably the most honest review possible. The test is brief, useful, and often far less intimidating than its name suggests.
Conclusion
A nerve conduction velocity test is a valuable tool for diagnosing peripheral nerve problems, locating areas of nerve damage, and helping distinguish between conditions that can otherwise look very similar. It is often paired with EMG to provide a more complete picture of nerve and muscle function. While the test can be temporarily uncomfortable, it is generally safe, fast, and highly informative.
If you are scheduled for an NCV study, the best thing to remember is this: the test is designed to answer questions, not create new mysteries. It helps your care team move from “something seems off” to “here is what the nerve is doing.” And when it comes to treating numbness, tingling, weakness, or pain, that kind of clarity is a big step forward.




