Table of Contents >> Show >> Hide
- What Is Cataract Surgery?
- The Purpose of Cataract Surgery
- Preparing for Cataract Surgery
- What Happens During the Procedure?
- Benefits of Cataract Surgery
- Risks and Possible Complications
- Cataract Surgery Recovery Timeline
- How to Support a Smooth Recovery
- Real-World Experiences: What Cataract Surgery Often Feels Like
- Conclusion
Cataract surgery sounds dramatic, like something involving lasers, heroic doctors, and a soundtrack. In real life, it is usually much calmer: a skilled ophthalmologist removes a cloudy natural lens and replaces it with a clear artificial lens called an intraocular lens, or IOL. The goal is simple but powerfulto help light enter the eye properly again so vision becomes brighter, sharper, and less like looking through a fogged-up bathroom mirror.
Cataracts are extremely common, especially with age. They happen when the eye’s natural lens becomes cloudy. At first, symptoms may be mild: brighter lamps help, new glasses seem useful, and night driving is only slightly annoying. Eventually, however, cataracts can interfere with reading, driving, recognizing faces, watching television, or enjoying colors that no longer look as lively as they used to. When daily life starts losing its crisp edges, cataract surgery becomes worth discussing with an eye doctor.
This guide explains the purpose of cataract surgery, how the procedure works, possible risks, recovery tips, and real-world experiences that patients often care about but do not always remember to ask during appointments.
What Is Cataract Surgery?
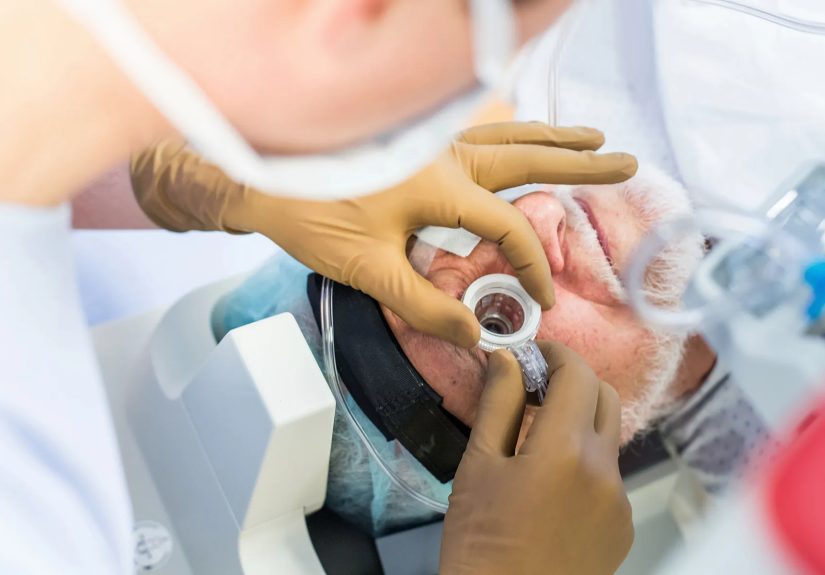
Cataract surgery is an outpatient eye procedure used to treat cataracts. During the operation, the cloudy lens inside the eye is removed and replaced with a clear artificial lens. Most people stay awake, but the eye is numbed so the procedure is not painful. The operation is usually done on one eye at a time, even if both eyes have cataracts.
The artificial lens is designed to stay in the eye permanently. It does not need cleaning, polishing, charging, or motivational speeches. Once it is placed, it becomes part of the eye’s focusing system. Depending on the lens selected, it may improve distance vision, astigmatism, or a range of vision. Some people still need glasses afterward, especially for reading or fine detail, but many notice a major improvement in visual clarity.
The Purpose of Cataract Surgery
The main purpose of cataract surgery is to restore vision affected by a cloudy lens. Cataracts can cause blurry vision, glare, halos around lights, faded colors, double vision in one eye, and trouble seeing at night. These symptoms often develop slowly, so people may not realize how much vision has changed until after surgery. A common patient reaction is, “Wait, white walls are actually white?”
When Is Cataract Surgery Recommended?
Doctors usually recommend cataract surgery when cataracts begin to affect quality of life. That may mean difficulty driving, reading medication labels, cooking safely, using a computer, watching television, or enjoying hobbies such as sewing, golfing, woodworking, or painting. Surgery may also be recommended if cataracts make it harder for the doctor to monitor or treat other eye conditions, such as diabetic retinopathy or macular degeneration.
Cataract surgery is not always urgent. If symptoms are mild, stronger lighting, updated glasses, anti-glare lenses, or magnifiers may help for a while. The key question is not simply, “Do I have cataracts?” It is, “Are cataracts interfering with the life I want to live?”
Preparing for Cataract Surgery
Before cataract surgery, the ophthalmologist performs a detailed eye exam. Measurements are taken to calculate the best power for the intraocular lens. This step is important because choosing an IOL is a little like choosing tires for a car: the basic option works, but lifestyle matters. A person who drives at night, reads constantly, works on screens, or wants less dependence on glasses may have different priorities.
The doctor may review medications, allergies, medical history, and existing eye conditions. Patients may be asked to use prescription eye drops before surgery to lower the risk of infection or inflammation. Some medications may need special planning, but patients should never stop prescribed medicine without clear instructions from their healthcare provider.
Types of Intraocular Lenses
Several types of IOLs may be available. A monofocal lens focuses at one main distance, often distance vision. A toric lens can help correct astigmatism. Multifocal and extended-depth-of-focus lenses may reduce dependence on glasses for multiple distances, although they may not be ideal for everyone and can sometimes cause glare or halos. The “best” lens is not the fanciest lens; it is the lens that fits the eye, the budget, the health of the retina and cornea, and the patient’s daily routine.
What Happens During the Procedure?
On surgery day, the patient usually checks in at an outpatient surgery center or hospital. Eye drops are used to dilate and numb the eye. A mild sedative may be offered to help the patient relax. The surgeon makes a very small incision and commonly uses a technique called phacoemulsification, where ultrasound energy breaks up the cloudy lens so it can be removed. Then the folded artificial lens is inserted through the small opening and positioned inside the eye.
The procedure is typically quick. Patients do not usually see the details of the surgery; they may notice lights, colors, pressure, or movement. Afterward, they rest in a recovery area for a short period. Because vision may be blurry at first and sedation may be used, someone else usually needs to drive the patient home.
Benefits of Cataract Surgery
The biggest benefit is clearer vision. Many people experience brighter colors, better contrast, less glare, and improved confidence with everyday tasks. Reading becomes easier. Driving may feel safer after the doctor confirms it is okay. Faces look sharper. The world stops looking like it was filmed through a dusty windshield.
Cataract surgery may also reduce dependence on thick glasses in some cases. However, results vary. Existing eye diseases, corneal problems, retinal conditions, severe dry eye, glaucoma, or diabetes-related eye changes can affect final vision. That is why a careful preoperative exam matters so much.
Risks and Possible Complications
Cataract surgery is considered common and highly successful, but every surgery has risks. Possible complications include infection, bleeding, swelling, increased eye pressure, inflammation, retinal detachment, drooping eyelid, dislocation of the artificial lens, or persistent blurry vision. These complications are uncommon, but they deserve attention because early treatment can protect vision.
One fairly common later issue is posterior capsule opacification, sometimes called a “secondary cataract.” This is not the cataract growing back. The natural lens is gone, and it does not regenerate like a tiny villain in a science-fiction movie. Instead, the thin capsule holding the artificial lens becomes cloudy. If it affects vision, doctors can often treat it with a quick laser procedure called YAG capsulotomy.
Warning Signs After Surgery
Patients should contact their eye doctor promptly if they develop severe pain, sudden vision loss, increasing redness, flashes of light, new floaters, nausea with eye pain, or discharge from the eye. Mild scratchiness, watery eyes, and temporary blur can happen during healing, but worsening symptoms should never be ignored.
Cataract Surgery Recovery Timeline
Recovery begins immediately after surgery. Vision may be blurry, hazy, or brighter than expected during the first day. Some people notice improvement within a day or two, while others need more time as swelling settles and the eye adjusts. Full recovery commonly takes several weeks, depending on the eye and the person’s overall health.
First 24 to 48 Hours
During the first couple of days, rest is the main job. Patients usually use prescribed eye drops to prevent infection and control inflammation. A protective shield may be worn while sleeping. It is important not to rub the eye, even if it feels itchy. The eye has just had surgery; it deserves gentle treatment, not a wrestling match.
First Week
Many normal light activities can resume quickly, but doctors often recommend avoiding heavy lifting, bending deeply, swimming, hot tubs, dusty environments, and eye makeup until cleared. Follow-up appointments allow the doctor to check healing, eye pressure, and vision. If the second eye also needs surgery, it is usually scheduled after the first eye has begun healing.
Weeks Two to Six
Vision often continues to stabilize over several weeks. Glasses prescriptions may change after healing, so doctors usually wait before prescribing new lenses. Some patients feel temporarily unbalanced if one eye has been corrected and the other still has a cataract. This is normal, but it can make depth perception feel odd until both eyes are treated or the prescription is adjusted.
How to Support a Smooth Recovery
The best recovery plan is surprisingly practical: use drops exactly as directed, keep follow-up appointments, avoid rubbing the eye, protect the eye from water and dust, and ask before restarting strenuous activities. Sunglasses can help with light sensitivity outdoors. Artificial tears may help if dryness is present, but patients should confirm which drops are safe to use with their surgeon.
It is also wise to prepare the home before surgery. Place frequently used items at waist level so there is less need to bend. Cook simple meals ahead of time. Keep pets from jumping near the face. If a dog has a personal policy of greeting people like a furry cannonball, consider creating a little recovery space.
Real-World Experiences: What Cataract Surgery Often Feels Like
Many people approach cataract surgery with two emotions: hope and “please do not let anything touch my eye.” That is completely normal. The eye is small, important, and not exactly an area where people enjoy surprises. One reassuring point is that the surgical team does this type of procedure regularly. For the patient, it may feel like a major life event. For the staff, it is a carefully choreographed routine.
A common experience before surgery is frustration with gradual vision loss. Cataracts often sneak in quietly. A person may buy brighter bulbs, clean their glasses five times a day, blame the windshield, blame the television, blame the restaurant menu font, and finally realize the problem is not poor lighting or tiny print created by mischievous graphic designers. It is the cloudy lens.
On the day of surgery, patients often describe feeling nervous during check-in, then calmer once the process begins. The numbing drops, monitoring, and explanations from nurses can make the experience feel more manageable. During the procedure, many people report seeing bright lights or colors rather than anything scary. Some feel pressure but not sharp pain. The surgery may be over sooner than expected, leaving patients surprised that the event they worried about for weeks took less time than assembling a sandwich with too many toppings.
The first look after surgery varies. Some people notice clearer vision almost immediately. Others see blur, glare, or a watery film at first. This does not always mean something is wrong. The eye needs time to heal, and the brain needs time to adjust to the new lens. Colors may look dramatically brighter. Whites may look almost too white. One eye may seem cooler or brighter than the untreated eye, which can make the untreated cataract more obvious.
Recovery also teaches patience. Eye drops can be annoying to remember, especially when there are multiple bottles with different schedules. A written chart or phone reminder helps. Sleeping with a shield may feel awkward, but it protects the eye from accidental rubbing. Avoiding swimming, heavy lifting, and dusty chores may be inconvenient, though some patients secretly enjoy having a medically approved excuse not to clean the garage.
Emotionally, cataract surgery can be more meaningful than expected. Clearer vision may restore independence, confidence, and small pleasures: reading street signs, seeing grandchildren’s faces, noticing leaves on trees, or driving with less glare. Still, expectations should stay realistic. Cataract surgery fixes the cloudy lens, but it does not cure every eye condition. If the retina, optic nerve, or cornea has other problems, vision may improve but not become perfect.
The best patient experience usually comes from asking questions early: Which lens is recommended and why? Will I still need glasses? What symptoms are urgent? When can I drive, exercise, shower normally, or return to work? Clear answers reduce anxiety, and reduced anxiety makes the whole process feel less like a mystery novel and more like a well-planned home improvement projectexcept the renovated room is your vision.
Conclusion
Cataract surgery is performed to improve vision when a cloudy lens interferes with daily life. The procedure removes the cataract and replaces it with an artificial intraocular lens. For many people, the results are brighter colors, sharper vision, and better function. The procedure is usually outpatient and recovery is often straightforward, but risks exist and follow-up care matters.
The smartest approach is simple: get a complete eye exam, understand your lens options, follow pre-surgery and post-surgery instructions, and call your doctor quickly if symptoms seem unusual. Cataract surgery may be common, but your eyes are still one-of-a-kind. Treat them accordingly.
Note: This article is for general educational purposes only and should not replace diagnosis, treatment, or personalized medical advice from an ophthalmologist or qualified healthcare professional.